Subgingival anomalies and pathologies viewed with the Perioscope: root fractures (Part 3)
In the abstract “A Review of Root Fractures: Diagnosis, Treatment and Prognosis,” by Malhotra, Kundabala and Acharaya**, root fractures are defined as fractures involving the dentin, cementum and pulp and occur in less than 8 percent of traumatic injuries to permanent teeth.
Root fractures are broadly classified as horizontal (transverse) and vertical root fractures (VRF) and can vary in severity.
Treatment of root fractures depends on a number of factors and is typically determined by the extent of the subgingival fracture, remaining coronal tooth structure, location of the fracture line, pulp vitality and length and morphology of the roots. Frequently, an interdisciplinary or multidisciplinary approach is required for complete rehabilitation of the tooth.
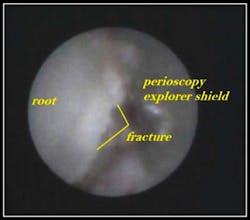
Case #1: Horizontal Root Fracture #9
By Robert Gottlieb, DDS, and Suzanne Newkirk, RDH
Root fractures that develop communication between the gingival sulcus and the fracture site have a poor prognosis because of bacterial contamination.
Due to the extent of the above fracture, treatment recommendations for this patient included extraction and immediate implant placement, which the patient proceeded with.
The video “Horizontal Root Fractures: Why Guess about a fracture?” may be viewed at:
http://www.youtube.com/watch?v=t-coebmV6cM
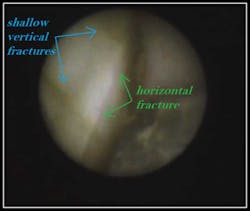
Case #2: Horizontal Hair Line Fracture #19
By Robert Gottlieb, DDS, and Suzanne Newkirk, RDH
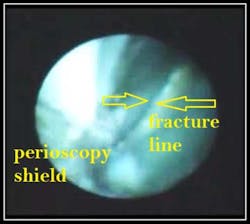
By Dr. John Y. Kwan Vertical root fractures typically extend through the long axis of the root toward the apex and commonly occur in endodontically treated teeth. Depending upon the severity of the fracture, an interdisciplinary and/or multidisciplinary approach may be required for functional and esthetic rehabilitation of the tooth. Intraosseous fractures typically create deep, narrow, sharply defined isolated periodontal pockets and radiographic examination may reveal unilateral thickening of PDL along the fracture side of the root. If the fracture is not apparent radiographically, diagnostic tests may be considered using a bite-test, transillumination test, or confirmation of the VRF via surgical exploration. Confirmation of root fractures with Perioscopy provides the most minimally invasive, non-surgical method available. The below photo and corresponding video clearly show a vertical root fracture.