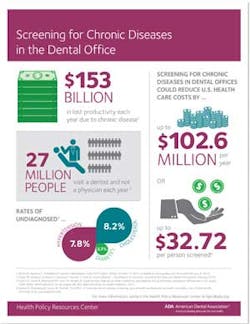
Are you screening in your dental office?
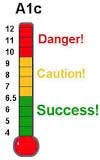
In this field trial, the researchers assess the feasibility of screening for diabetes and prediabetes in dental practices and in a community health center. The patients were over age 45, and had not been diagnosed with diabetes. They were screened for diabetes risk with an American Diabetes Association (ADA) Diabetes Risk Test and with hemoglobin HbA1c measurement. Participants with an HbA1c level of 5.7 percent or greater were referred to their physicians for diagnosis.
The study results show that screening for prediabetes and diabetes is indeed practical in a dental office, with good acceptance by the dentist and dental office staff members, patients’ physicians and patients. Patients from the community health center showed good adherence with referrals to medical providers (78.8%). On the other hand, adherence was much worse (21.5%) among those in the private dental offices.
The authors deduced that opposition to follow up could be due to a number of factors, such as: denial, optimism, bias, fear of receiving a diagnosis of diabetes, costs, lack of motivation in patients who are asymptomatic, lack of access to medical care and behavioral issues.(7) Dental hygienists are in a prime position to monitor and follow up with patients to ensure that they heed the medical referral. Dr. Genco mentioned that there are barriers to implementing testing, such as lack of financial incentives for the dental office.(8)
I think it is obvious that screening for diseases like diabetes in the dental office is not only practical, but our responsibility. Interprofessional collaboration is necessary if we wish to end the deadly cycle of chronic diseases. The researchers at the University of Buffalo and ADA Health Policy Resources Center (HPRC) have proposed incentive and a chronic care model whereby dental and medical health care professionals can work together for the health of the patient. Who knows, we might just save a life!