This is the case of a 71-year-old white female who was referred to the office for a second opinion by her general dentist. Chief complaint: A painful right lower jaw and moderate-to-large growth in the right posterior mandible behind tooth no. 31. The patient stated that the “lump” had begun to grow only two weeks prior, although the pain in her right jaw (which was constant and throbbing) had been present for about six weeks. It had begun with some numbness in her right lip. She had already been to one surgical specialist prior to the mass forming. The specialist performed a clinical exam and x-ray imaging, but could not find any abnormalities. He referred the patient to testing for trigeminal neuralgia.
The patient’s medical history is significant for morbid obesity, high cholesterol, hypertension, coronary artery disease, and endometrial carcinoma 14 months ago that was treated with radiation and chemotherapy.
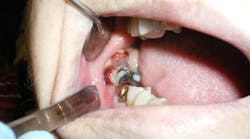
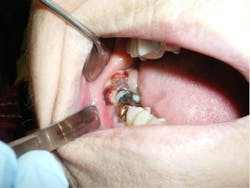
While performing a clinical exam, a 2.5 cm diameter round, greyish-pink mass was observed directly behind tooth no. 31. There was no tenderness to palpation, although the tissue was friable and bled easily. Tooth no. 31 was mobile (class II), with little tenderness to palpation. The other teeth in that quadrant were normal, as was the rest of the intraoral exam. There was no extraoral swelling, no bony expansion with palpation of the mandible, and no cervical lymphadenopathy. The right mandibular division of the trigeminal nerve showed paresthesia upon nerve testing.
Differential diagnosis
- Squamous cell carcinoma of the right retromolar trigone
- Central squamous cell carcinoma
- Metastasis to the oral cavity
- Pyogenic granuloma
- Infection of the oral cavity
Recommended treatment
Metastasis to the oral cavity is a condition that may arise when metastatic disease from a distant carcinoma spreads via a hematogenous route to either the soft tissues of the oral cavity or to either of the jaws. This condition is thought of as a relatively rare occurrence, although it may happen more often than we think due to the terminal nature of most of these patients and the condition going undiagnosed during the final months of the patient’s life.1,2 Prevalence for this disease seems to favor the mandible over the maxilla, and the jaws far more than the oral soft tissues.2 Most common originating primary site is the breast, followed by the lungs, and then the kidneys.2
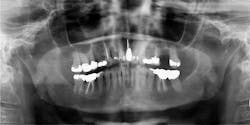
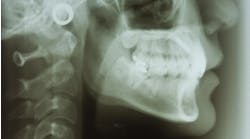
Clinically, patients can exhibit a variety of symptoms—from nonspecific pain in the jaw, to numbness in one division of V3 or V2.1,2 When a lesion develops enough in the jaws to reach the dentition, it is common to find what appears to be a large periodontal defect around a tooth, periodontally failing teeth, or a (usually) large mass from a recent extraction socket or from around the PDL of a tooth.1 Most of these masses are painless upon palpation and not ulcerated. Imaging early in the metastatic process often show no lesions on panorex. Later changes include a lytic-type lesion or "moth-eaten" lesion, with poorly defined borders.1,2
Diagnosis of these lesions requires a biopsy, with appropriate follow-up cancer staging imaging via a PET scan or PET CT.
In this patient's case, due to the suspicious nature of the lesion being a malignancy, a biopsy was taken at the initial visit. A consultation was also done with the patient’s oncologist, who recommended scheduling a PET CT. Biopsy confirmed metastatic endometrial carcinoma, and the PET CT showed multiple metastatic lesions in the patient’s liver, thoracic aorta, and vertebrae. Most often, prognosis with these lesions is very poor, given that this diagnosis puts patients into a Stage IV situation involving their original cancer.1,2 This held true with our patient; these were not resectable or treatable metastatic lesions.
Palliative care was offered, which involved extractions of tooth nos. 30 and 31. Radiation was targeted at the right mandibular lesion in an attempt to prevent a pathologic fracture and regrowth of the oral lesion. Chemotherapy was also restarted in an attempt to slow the growth of the metastatic lesions.
References
- Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and Maxillofacial Pathology. Philadelphia, PA: Saunders; 2002:582-583.
- Marx RE, Stern E. Oral and Maxillofacial Pathology: A Rationale for Diagnosis and Treatment. Hanover Park: IL: Quintessence; 2003:822-825.