Three-dimensional endodontic obturation the safest and easiest way possible
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.
When we talk about three-dimensional obturation, various thermoplastic techniques come to mind. Studies have shown that thermoplasticized gutta-percha obturation results in a larger volume of gutta-percha in the canal compared to cold lateral and vertical condensation and obviously single-point obturation. The higher volume of gutta-percha has been taken as proof of a superior seal when, in fact, the seal is dependent upon the intimate relationship of the cement to both the gutta-percha and the canal walls. Consequently, the inference of a higher volume of gutta-percha being proof of a superior seal is secondary to the fact that the cement is forced into a more intimate relationship with the canal walls.
ALSO BY DR. BARRY MUSIKANT |Endodontic insight into safety, efficiency, and cost savings
Thermoplastic obturation takes several different forms. Carrier-based thermoplastic systems have evolved away from metal and plastic carriers to the point where they are now constructed of two different phases of gutta-percha, with the outer layer thermoplasticized far more than the inner core, which acts as the carrier. All thermoplastic techniques require the minimum placement of cement, because the coronal pathway for the release of excess cement is occluded first, eliminating the escape valve when room temperature systems are employed. Another thermoplastic approach is the use of a heated spreader that first requires the placement of a conventional gutta-percha point to the constriction followed by heated vertical condensation within 5 mm of the apex and conventional condensation within 2 mm of the apex. This form of thermoplastic obturation adapts the gutta-percha to the walls of the canal within the last 2-3 mm of the canal. Interestingly, the gutta-percha that was placed at room temperature is not affected by the heat introduced by the spreader and remains more or less in the same position as when it was originally placed. Strictly speaking, the most apical placement of the gutta-percha has not been thermoplasticized and is essentially a single-point fill. The advantage is no shrinkage.
ADDITIONAL READING |Trauma and horizontal root fractures of the anterior teeth: A review and case report
After adaptation of the point to the canal wall via the heated spreader, a void extending from the most apical 2 mm of gutta-percha to the orifice is present. This space is then filled using one of several available glue guns that deposit thermoplasticized gutta-percha through a thin, silver needle. Being thermoplasticized, the entire deposited body of gutta-percha will shrink as it cools to body temperature again, compromising the concept of a true three-dimensional fill. The same problem occurs when the squirt technique is applied, a form of obturation that skips a heated spreader and goes directly to the extrusion of molten gutta-percha from the constriction to the orifice. Again, shrinkage is unavoidable.
While thermoplastic obturation results in shrinkage, it minimizes the excessive stresses that cold lateral and vertical condensation can be transferred to the root. The application of heat can also be excessive, resulting in thermal shock to the dentin as well as potentially damaging the surrounding periodontal ligament. In fact, one should realize when using a thermoplastic spreader that the duration of the application of heat is critical. Manufacturers suggest no more than a two-second application of 201-degree heat. A duration longer than that increases the temperature to the ligament beyond 10 degrees C that has been documented to damage the ligament. This type of thermoplastic obturation imposes a narrow window for success and subsequently a large window for unintentional iatrogenic damage.
For me, the most irrational aspect of cold vertical and lateral condensation is the application of force via a tapered spreader that can easily exceed the tensile strength of dentin. From a practical point of view, it is difficult to determine whether this particular criterion is being met and even if it is, is the generation of excessive stress truly avoided? This is a perfect example of where a route that completely avoids these possibilities is the safest.
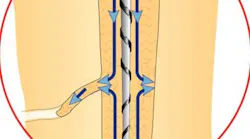
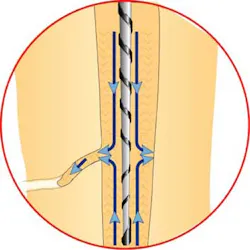
With thermoplastic obturation in its several forms and cold lateral and vertical condensation producing voids and the potential for excess stresses to the roots, my choice for trauma-free obturation is a single-point technique. It is a passive technique that will not generate excessive stresses. The question asked by those using alternate techniques is whether or not it is an effective means for canal obturation. Like all obturation systems, the effectiveness of the single-point technique is based on the cement. However, the single-point technique requires that the cement be an effective seal in both thick and thin layers and that it be present in sufficient quantity that it can fill all the gaps between the master gutta-percha cone and the walls of the canal. For this to happen, we need an instrument that can flood the canal with cement prior to the placement of the prefitted gutta-percha point.
One last question that someone might ask is what do we do when the canals are highly oval with a lot of buccal and lingual space after the master point has been placed? One can go two ways. The cement already flooding the canal is occupying that space effectively and needs no further gutta-percha points. Alternatively, one can use a spreader to create a lateral space for the placement of an auxiliary point with the proviso that the pressure applied to the spreader does not exceed the weight of one’s hand. We have no desire to mold the gutta-percha that would induce the rebound effect or expose the roots to any further stress. Rather, we apply just enough pressure to create a space where a subsequent well-coated point is then placed.
By using a passive obturation technique, we scrupulously avoid the introduction of stresses, maintain the accurate placement of the gutta-percha point, and avoid the introduction of voids that would compromise the seal. The fact that the employment of this technique is simpler and far less expensive is a wonderful marketing feature, but does not surpass the fact that it is safer and kinder to the tooth.
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.
References
1. Lee CQ, Chang Y, Cobb CM, Robinson S, Hellmuth EM. Dimensional stability of thermosensitive gutta-percha. Journal of Endodontics 1997;22(12).
2. Shemesh H, Bier CAS, Wu MK, Tanomaru-Filho M, Wesselink PR. The effects of canal preparation and filling on the incidence of dentinal defects. Int Endod J. 2009;42(3):208-213.
3. Kumaran P, Sivapriya E, Indhramohan J, Gopikrishna V, Savadamoorthi KS, Pradeepkumar AR. Dentinal defects before and after rotary root canal instrumentation with three different obturation techniques and two obturating materials. J Conserv Dent. Nov. 2013;16(6):522-526.
4. Weathers K, Wahl P. EZ-Fill obturation system lives up to its name. Practical Endodontics 1999;(8):5.