Improving endodontic success rates: Optimizing preoperative dental case assessment
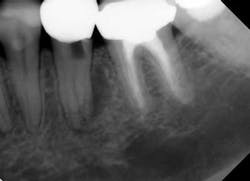
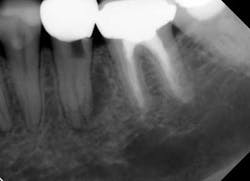
Knowing when a tooth is restorable (and when it is not) is a key diagnostic skill and a predictor of future endodontic success. Taken at face value, this concept seems obvious, but, for example, assessing when a tooth is vertically fractured and/or has a risk of future vertical fracture is not always clear, as is illustrated by the case shown in Fig. 1.
Endodontic success rises exponentially when therapy is performed only on those teeth possessing a reasonable clinical prognosis and predictable failures are extracted. This clinical article was written to identify nonrestorable teeth and provide preoperative treatment-planning suggestions to optimize results.
As a starting place, when contemplating endodontic treatment, clinicians should ask themselves the following questions:
- Can this tooth be restored?
- Should this tooth be restored?
- If the tooth is not now restorable, can it be made restorable?
- If the tooth has a guarded prognosis, has the patient been made aware of the risks involved in retaining the tooth?
To help guide decision making, assuming no clinical means exist to remediate the parameters below (crown lengthening, orthodontic extrusion, grafting procedures, etc.), nonrestorability is primarily related to inadequate:
- Coronal tooth structure
- Bone support
- Crown root ratio
As an aside, among other considerations beyond the scope of this article, one critical consideration impacts treatment feasibility. If, after informed consent, the patient does not want endodontic therapy for whatever reason, the tooth should be extracted.
In a general sense, endodontic treatment can be broken down into three primary phases: preoperative planning, the procedure, and the postendodontic coronal seal/restoration.
Numerous risk factors and findings determine the technical feasibility of treatment. These risk factors and findings should be assessed in the preoperative phase mentioned above. These include but are not limited to:
- Inadequate clinician training, experience, equipment, materials, time, and staff limitations
- Anatomic and pathologic factors (curved and calcified canals, atypical anatomy, root resorption, tipped and rotated teeth, dens in dentae, high furcation, immature roots, open apices, etc.
- Access through crowns and bridges
- Strategic and functional value of the tooth
- Failed previous endodontic orthograde or retrograde treatment and previous access
- Iatrogenic issues (perforation, separated files, etc., among many other possible misadventures)
- Inadequate access to the tooth, including limited opening, gagging, hyperactive tongue, etc.
- Trauma cases
- Behavioral, phobia, and patient management issues
If, after assessing the above, the clinician believes the tooth is restorable but beyond his or her capabilities, referral is indicated.
Coincident to the clinical case details above, how the clinician obtains, records, and assesses the case is critical in making sound decisions. At a minimum, preoperative case assessment suggestions include:
- A detailed assessment of the patient’s medical and dental history prior to evaluation for endodontic treatment.
- Assessing each case with a SOAP (subjective, objective, assessment, plan) analysis. In essence, first recording the subjective and objective findings and then making a case assessment and a plan for treatment (based on the results of the informed consent).
- Informed consent might be charted in a PARQ (procedure, alternative, risks, questions) format. The procedure, alternatives, and risks of treatment should be discussed with the patient and all questions answered.
- Inherent in the SOAP analysis at a minimum is obtaining adequate radiographic evaluation, possibly a CBCT as needed; recording the percussion, palpation, mobility, and probing for all the relevant teeth in the area; and evaluating the periodontal condition.