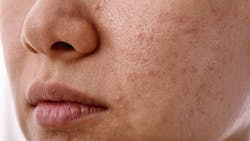
Skin care in the age of N95s
The coronavirus pandemic has significantly changed personal protective equipment (PPE) requirements for dental professionals. The N95 respirator is emerging as the new standard for aerosol protection against the smallest of microorganisms. While regulatory requirements currently do not mandate the use of these high filtration masks, many clinicians are following this recommended guideline to ensure an elevated level of facial protection.
Unfortunately, for some, the regular and prolonged use of N95s has brought some pretty undesirable effects to the skin. Clinicians are now reporting higher incidences of breakouts, acne, irritation, rash, scarring, inflammation, and abrasions. Facial skin tends to be more sensitive and fragile than skin on other parts of the body and is more reactive to N95 respirators. It has been reported that 97% of frontline workers are reporting skin problems directly resulting from the use of N95s.1
Clinicians will likely find that their skin care routines may need some adjustments in order to sustain regular use of N95s. This article will review the anatomy of healthy and irritated skin, discuss the three primary root causes of skin irritation associated with wearing N95 respirators, and offer a guideline for skin care in the new age of personal protective equipment
The three layers of skin
The thinnest, outermost layer is the epidermis. This layer contacts the N95. Since it is the thinnest, it can be easily irritated and torn. The epidermis is made up of pores that communicate between the environment and the deeper layers of skin.
The dermis is the next layer of skin that contains sweat glands for thermoregulation and a vascular complex to nourish the skin. Even though the dermis is thicker than the epidermis, it is still prone to irritation from environmental sources.
The hypodermis is the deepest layer that contains the fatty components of skin along with larger vascular vessels. Running through all three layers is the hair follicle that can also be a communication channel for irritants.
Healthy skin relies on having a clean surface, minimal irritation, and the ability to thermoregulate. When any of these factors are impacted, a person can experience any of the symptoms listed above. The regular wearing of N95 respirators places clinicians directly in the path of compromising these factors.
Three sources of irritation
The many skin irritations resulting from N95 respirator usage seem to fall into one or more of the following categories:
- The material as a contact irritant
- The inability to thermoregulate
- Exhalation contamination
According to Thomasnet.com, an industrial sourcing platform and marketing company used by major manufacturers such as 3M and Honeywell, N95 respirators are constructed from nonwoven polypropylene that goes through a layered melting and bonding process known as spun-bonding.2 Additionally, masks undergo a needle-punching process in which sharp fibers are punched into the mask layers to further increase the bond strength of fibers. Sometimes, additional layers of chemical additives are used to enhance filtration characteristics. The finished product usually has an aluminum strip that allows for tighter fit across the nose.2,3
For many clinicians, the outbreaks and irritations may be caused by sensitivity to polypropylene or aluminum. While polypropylene is considered a very biocompatible plastic, those with sensitivity to it will have an adverse reaction similar to a contact dermatitis.4,5 Both materials are also capable of causing painful friction abrasions that can be slow to heal with repeated N95 use, resulting in scarring, also called frictional melanosis.5
Due to the tight fit of N95 respirators, the skin’s ability to thermoregulate can become compromised. In order for the body to maintain its optimum temperature, it must be able to release heat through two means: sweating and vasodilation.6-8 Since N95s are minimally porous and fit tightly on the face, the ability to release heat is greatly reduced. In a recent interview with Kasia Cichowicz (June 2020)9, licensed esthetician at Amazing Face in Sunnyvale, California, eccrine sweat glands in the dermis skin layer produce sweat droplets that rise to the skin’s surface to dissipate heat. “Once you start losing moisture from your skin, sebaceous glands then generate and release lipids to lubricate and waterproof the skin to prevent further water loss.”
She further states that oilier skin types tend to produce more oils, which can result in acne breakouts. Water loss in drier skin types tend to result in further uncomfortable dryness and possible abrasions. Sensitive skin types lack an adequate lipid barrier, also leaving clinicians prone to these irritations. Ms. Cichowicz also points out that male skin tends to have a thicker dermis layer along with more hair follicles. These two factors make male skin more resilient to friction abrasions and moisture loss.
In addition to sweating, vasodilation is another thermoregulatory mechanism of skin.6-8 Blood vessels dilate to allow blood to cool in the affected area. As blood flow in the affected area is constricted during N95 wear, the skin can turn excessively red. Clinicians with such sensitivities often report concurrent redness, flare-ups, and breakouts, according to Ms. Cichowicz. She summed up by stating that how skin reacts depends on skin type as well as water and lipid content.
The last source of skin irritation with N95 use is exhalation contamination. It is common knowledge that exhaled air is filled with a variety of microbes ranging from bacteria to viruses to molds and fungi that have their origin in the mouth.10 But what happens when this exhaled air (filled with microbes) does not have an escape path while wearing a near-impervious mask for extended periods of time? These microbes remain in the airspace under the mask and can resettle on skin. The concurrent moisture from sweat and oil secretion during thermoregulation then provides a moist, warm environment for bacteria to thrive on the skin’s surface. As bacterial colonies multiply on the skin surface, acne breakouts, itching, and inflammation can occur.
Skin care
Whether or not the N95 respirator mask will become required PPE is yet to be seen. However, for those clinicians who are currently using N95s as a standard face covering and are having skin outbreaks, having a good skin care strategy is important in managing adverse reactions and supporting its long-term health. In order to do so, it is important to understand the root cause(s) of the outbreak. Most skin outbreaks can be minimized by keeping surfaces as clean as possible and adequately moisturized. According to Ms. Cichowicz, a healthy routine includes washing your face with a soap-free, hypoallergenic, and fragrance-free cleanser. In general, moisturizers with fewer ingredients are preferred.
Dry skin types require delicate care and should avoid washing with hot water, as this tends to strip necessary oils from skin. Prolonged hot showers will also do the same. Once skin is cleansed, a good moisturizing routine is very important. There are many varieties of moisturizers on the market. Key ingredients include glycerin, hyaluronic acid, and high-quality oils such as avocado and argan, which will help lock in moisture. Specialty serums are also often packed with high potency ingredients to restore necessary nutrients such as antioxidants and collagen.11 Breakouts can often be soothed with topical calendula or clay masks targeted for dry skin.
Oily skin types also require a measure of careful cleaning and moisturizing.12 Unlike dry skin, oilier skin types will tolerate higher water temperatures when cleansing. In fact, washing with warmer water helps to open up pores and break up oily molecules more readily. Care must be taken to not strip too much oil from skin as this can also have a negative impact. Once cleansing is done, the use of toners such as zinc and witch hazel helps close up pores. The occasional use of clay masks will also help restore balance and control excess oil production.
Clinicians who wear N95 masks all day long may need to plan mask removal breaks to allow for midday cleansing and give the skin a chance to breathe. When time does not allow for cleansing during the day, using toners is a second-best option. While professional facials have traditionally been considered a luxury, they may very well become a part of routine health care in the age of N95 mask usage.
Clinicians may also want to reevaluate wearing makeup, as this may also increase irritation. If wearing an N95 mask has caused broken skin, there is an increased chance for infection and scarring. Since dry skin can break easily, care must be taken to protect damaged skin from scarring by using topical antibiotics to protect from infection and promote healing. The use of cold compresses will help to minimize inflammatory reactions. In addition to good daily skin care, clinicians should also employ nasal breathing as much as possible while masked to minimize exhalation contamination.
The coronavirus pandemic has certainly created many personal protective equipment challenges for clinicians. While it is not clear whether the use of N95 respirators will be mandated, those choosing this higher level of masking have faced many adverse reactions with prolonged use. Having a good skin care strategy will minimize the negative impacts of wearing N95s. In order to do so, clinicians must first identify their skin type, understand sources of irritation, and adopt a good skin care regimen that reflects individual needs.
References
- Elston DM. Occupational skin disease among health care workers during the coronavirus (COVID-19) epidemic. J Amer Acad Dermatol. 2020;82(5):1085–1086. https://doi.org/10.1016/j.jaad.2020.03.012
- Henneberry B. How to make N95 masks. Thomasnet.com. https://www.thomasnet.com/articles/plant-facility-equipment/how-to-make-n95-masks/
- Institute of Medicine of the National Academies. Reusability of Facemasks During an Influenza Pandemic: Facing the Flu. The National Academies Press;2006. https://doi.org/10.17226/11637
- Eczema types: contact dermatitis overview. American Academy of Dermatology. https://www.aad.org/public/diseases/eczema/types/contact-dermatitis
- Upadhyay B. Suffering skin damage from face masks? Experts offer remedies. Outlookindia.com. April 5, 2020. https://www.outlookindia.com/newsscroll/suffering-skin-damage-from-face-masks-experts-offer-remedies/1791785
- Charkoudian N. Skin blood flow in adult human thermoregulation: How it works, when it does not, and why. Mayo Clinic Proceedings. 2003;78(5):605-612. https://www.mayoclinicproceedings.org/article/S0025-6196%2811%2961930-7/fulltext
- Romanovsky AA. Skin temperature: its role in thermoregulation. Acta Physiol. 2014;210(3):498–507. https://doi.org/10.1111/apha.12231
- Thermoregulation. Healthline. June 6, 2017. https://www.healthline.com/health/thermoregulation
- Cichowicz, K. (2020, June). Personal communication [interview].
- Fabian P, Brain J, Houseman EA, et al. Origin of exhaled breath particles from healthy and human rhinovirus-infected subjects. J Aerosol Med Pulm Drug Delivery. 2011;24(3):137–147. https://doi.org/10.1089/jamp.2010.0815
- Marie A. The exact skincare routine girls with dry skin should follow. The Zoe Report. 2019. https://www.thezoereport.com/beauty/skincare/dry-skin-skincare-routine
- How to control oily skin. American Academy of Dermatology. 2020. https://www.aad.org/public/everyday-care/skin-care-basics/dry/oily-skin
- Dougher K. How to properly wash your face when you have dry skin. Stylecaster. May 21, 2015. https://stylecaster.com/beauty/how-to-wash-dry-skin/
Susan L. Quan, MPH, MBA, RDH, has been a licensed dental hygienist for 31 years and is currently the clinical director of oral wellness in a large periodontal practice in Campbell, CA. Susan is committed to helping fellow clinicians achieve clinical excellence in dental hygiene practice through application-based continuing education.
About the Author
Susan L. Quan, MPH, MBA, RDH
Susan L. Quan, MPH, MBA, RDH, has been a licensed dental hygienist for 31 years and is currently the clinical director of oral wellness in a large periodontal practice in Campbell, California. Susan is committed to helping fellow clinicians achieve clinical excellence in dental hygiene practice through application-based continuing education.
Updated September 24, 2020