Life after laminectomy: Dental hygienist receives surgical option for debilitating occupational pain
By Theresa McCarter, RDH, BSDH
Asking a dental hygienist if he or she has any musculoskeletal pain is a ridiculous question. Working in this profession is considered as one of the most damaging careers to your body. Sitting for long periods, bending and holding your neck in a precarious position, and using our arms and shoulders in unnatural positions can be detrimental to our bodies.
Very few people are excluded from experiencing pain at some point in their lives resulting from this career. While there are many different ergonomic modalities that have been introduced over the years, many of us will experience severe pain, which may not be relieved without surgical intervention.
I entered this career at a later age than most individuals. I turned 40 at the time of my graduation from dental hygiene school. I knew that I had to be especially vigilant in keeping my body healthy from the repetitive stress. I invested in Orascoptic loupes with a light, an ergonomic chair with armrests, lightweight handles on my instruments, sharp instruments, and many ultrasonic tips.
I exercised and kept my weight down, ate healthy foods, and read many books and journal articles that were available on body mechanics. I attended numerous continuing education courses on ergonomics. I stretched before I started my day and in between patients, and I cut my work schedule down to two to three days a week.
Unfortunately, I could not escape degenerative disc disease and arthritis, which resulted in chronic headaches and excruciating neck pain.
Exposure to pain
The pain began 5 years ago when I was 52, with mild to moderate neck pain, muscle weakness in the upper arms, and occasional headaches. I went to see an orthopedic surgeon who ordered an MRI and it showed two mild herniations on C-5/6 and C6/7. My range of motion was very good, and he believed that, with core building exercises, I could relieve my pain. He prescribed 60 Vicodin. The physician stated that this was a very normal MRI for a woman my age and my pain was likely caused from arthritis. I took this advice and began Tai chi and Pilates, but I did not take any pain relievers other than ibuprofen. My pain continued.
Over the next five years, I saw three other orthopedic surgeons, two pain management anesthesiologists, a chiropractor, massage therapists, physical therapists, an acupuncturist, an osteopath, and this was all in addition to my primary care physician.
The general consensus of all of the professionals was to try any treatment other than surgery to relieve my pain. The procedures included cortisone injections and radiofrequency ablation, which offered no relief whatsoever. The medications included Flexeril, Soma, Robaxin, Vicodin, Mobic, Celebrex, Cymbalta, and tramadol—as well as holistic approaches and essential oils. I was happy for many of my colleagues who found relief with some of these therapies, but none of them relieved my symptoms.
My frustration grew, but I continued to work and suffer with the pain. I believe that I hid my pain from others in my workplace, and the only person who truly understood my pain was my husband who saw me suffering at night. The only medication that I took at this time was 800mg of ibuprofen, which barely touched the severe pain.
The breaking point
December 2016 was my breaking point. The pain and headaches were debilitating. I realized that I could not remember what it felt like to not have a headache. I could not fathom that neck pain was going to be a permanent part of my life, and I thought that I would not make it to the age of 60, let alone continue with a career in dental hygiene.
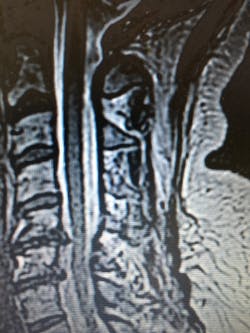
I encouraged my primary care doctor to order another MRI, which would be the third in five years. The results were shocking because the herniations of C5-7 were very large and the disc desiccations and osteophytes were right there in black and white.
A friend who was an anesthesiologist referred me to the Tucson Orthopedic Institute. We made an appointment with Dr. Jeffrey Baron, an orthopedic surgeon. Dr. Baron was a no-nonsense individual and blatantly stated that cervical spine surgeries statistically do not have favorable outcomes. He was not optimistic that I would be rid of my headaches or neck pain. He did not want to hear what any other physician had said about my condition and did an initial exam and x-rays.
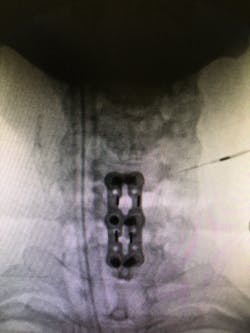
After viewing the films, he agreed that an anterior discectomy/laminectomy and fusion of Cervical 5-7 with a bone graft was the best surgical procedure. He outlined in detail what the procedure included from beginning to end, and he expressed his confidence in actually performing the procedure. He left the decision up to me, and I quickly made the choice to schedule the surgery and try what may be my last resort.
I am three weeks post-surgery, and I have no headache or neck pain, nor am I taking any medication. It will be six months to fully identify if the surgery is a complete success. At this point, I am hopeful.
The burning question—and I believe I know the answer—is that I will most likely never be able to return to clinical hygiene in the same capacity as before the surgery. I believe that I knew a few years ago that I would not be able to perform dental hygiene duties into my sixties due to my skeletal problems. I began to prepare for different work that was related to hygiene and education. I am fortunate to have my BS degree in dental hygiene and began to teach one day a week at a dental hygiene program near my home.
I also became a substitute elementary school teacher for the school district in my city. Most recently, I created a continuing education company called Hygienewize, LLC that offers CE courses approved through the Dental Board of California. I also became a CPR/AED/BLS provider for the American Red Cross, and I offer trainings to dental offices and the general public.
While none of these will ever replace working directly with my patients and the staff at my office, I am hopeful that I will continue to make a difference in the oral health-care community. I hope to help other dental professionals by providing research information on new products, existing and new therapies, employment opportunities and changes that are happening in the dental hygiene career.
To other dental hygienists who are suffering with chronic pain, I want to encourage you to plan for your future in the event that clinical hygiene becomes impossible. Seek higher education, network with other dental professionals, research other employment opportunities, and create your own destiny. We entered this career because we loved helping others and being involved in an important part of overall health for individuals and we must find opportunities that can keep us involved in the career that we loved but can longer perform in the ame capacity.
Reference
1. O’Neill, MD, MS, Kevin. ACDF: Anterior Cervical Discectomy and Fusion. Available at: https://www.spine-health.com/treatment/spinal-fusion/acdf-anterior-cervical-discectomy-and-fusion (2016). Accessed February 4, 2018.