Current Anesthetics & Pain Management
By Wendy S. Hupp, DMD
SAFETY, RELIABILITY, AND TOLERABILITY ARE KEYS FOR SUCCESSFUL PAIN MANAGEMENT IN DAILY DENTISTRY.
Modern dentistry has a reputation of being preventive and nearly painless. With the advent of the high-speed, air-turbine handpiece and the laser, tooth preparation is much less traumatic. Both techniques reduce frictional heat damage to the pulp so that post-operative pain is decreased. The laser may even be used for preparing many cavities without anesthetic. Many patients remember how it used to be, and certain procedures require local anesthesia and post-op, prescription pain medication. Let’s address some new pharmacotherapies for anesthesia and analgesics.
Articaine
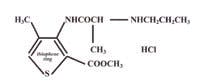
One of the newest anesthetics in the United States is articaine. Developed in the 1970s, it has been used in Europe and Canada for decades. In April 2000, the Food and Drug Association approved its use in a 4 percent hydrochloride solution with 1:100,000 epinephrine (Septocaine, Septodont USA). The drug is similar to other amide anesthetics such as lidocaine, except that it contains a thiophene ring instead of a benzene ring. The thiophene ring contains a sulfur atom instead of all carbons. The structure of articaine is otherwise similar to the amide prilocaine (see diagram below).1 Amide local anesthetics are now the drugs of choice because they do not show the relatively high incidence of allergic reactions seen with the ester anesthetics. Even with the sulfur atom, articaine has not been observed to cause problems with patients who are allergic to “sulfa” or sulfonamide drugs. The risk of causing an allergic reaction is similar between articaine and the other amide anesthetics and is most likely a reaction to the preservative sulfites included for the vasoconstrictor in the carpule.
Articaine can be used for infiltration or nerve-block anesthesia. The molecule is much smaller than the lidocaine molecule and is absorbed into nerves much faster than other amides. This results in an onset time of one to six minutes and pulpal anesthesia duration of 60 minutes. Well-controlled studies have shown that 4 percent articaine with 1:100,000 epinephrine and 2 percent lidocaine with 1:100,000 epinephrine performed similarly in onset of effect, depth of anesthesia, spread of anesthesia, and duration of effect.2
An advantage of using articaine is that 90 percent of the drug is metabolized by enzymes in the plasma. This leads to its short half-life of about 25 minutes compared to that of lidocaine at about 100 minutes. Patients with liver disease should be spared the stress on the hepatic microsomal enzyme system. There should be fewer drug interactions with articaine, and it is less likely there will be an accumulation of the drug with repeated injections over several hours.
Like lidocaine, articaine can cause systemic reactions. Toxic levels of either drug can lead to convulsions and subsequent cardiovascular and respiratory collapse. Any local anesthetic with epinephrine can lead to tachycardia, and the proper aspiration technique should be followed. Articaine is available as 4 percent solution and the carpules made by Septodont contain 1.7 milliliters. The maximum dose in milligrams of articaine is the same as lidocaine, however the maximum number of carpules is roughly half that of lidocaine.
Articaine has not been tested on children younger than 4. The recommended doses by volume are 0.5 to 2.5 milliliters for infiltration, 0.5 to 3.4 milliliters for nerve block, and 1 to 5.1 milliliters for oral surgery.1 Nerve paresthesia in regional anesthesia such as the inferior alveolar nerve block has been reported with 4 percent articaine. Malamed et al.3 concluded that the incidence of postinjection paresthesia with 4 percent articaine was not significantly different than 2 percent lidocaine, both with 1:100,000 epinephrine. It is postulated that a 4 percent solution of anesthetic may be neurotoxic because of the higher concentrations (articaine, prilocaine) and that these drugs should not be used when the needle may pierce the nerve.2 Personal communication with Septodont suggests that the small size of the articaine molecule may allow it to penetrate the neurons at a greater concentration than other anesthetics, leading to an extended healing time of up to one year for altered sensation to resolve [Orlando, March 2006].
Oraqix
The combination of lidocaine and prilocaine as a topical anesthetic has been used in a cream form for several decades (EMLA, AstraZeneca). It has been proven safe for children for needle procedures such as lumbar punctures, and also in newborns for circumcision.4 Oraqix (OraPharma, Inc., DENTSPLY Pharmaceutical) is formulated as a liquid at room temperature that turns into a gel at body temperature. The contents include 2.5 percent of each lidocaine and prilocaine. This preparation is not used for injection, but is applied with a device that delivers the liquid into the periodontal pocket before the tissue is manipulated. Dental hygienists can use this bendable needle applicator, achieving 10 to 20 minutes of soft-tissue anesthesia with a short, 30-second onset.
Oraqix was approved by the FDA in December 2003. The lidocaine and prilocaine are absorbed from local tissues, but the systemic levels are at least 20 times below those able to cause toxic levels in the central nervous system.2 Most patients are comfortable during oral hygiene procedures and have the added benefit of no postappointment numbness or injection-site soreness.5 My personal experience reveals that there may have been some dentinal absorption of the medication, further easing the pain of scaling and root-planing procedures. While some patients may object to the taste, the tongue is rapidly numbed as well, so the slightly bitter taste is masked.
In those states where hygienists can give anesthetic injeections, this product allows them to proceed without interrupting dentists’ schedules. The applicator is well-designed and easy-to-handle by a small hand. The anesthetic cartridge and blunt-end needle are packaged together and made to fit the Oraqix applicator only - no chance for the drug to be mistakenly used in a typical aspirating syringe.5,6
Combunox
Dentists should anticipate their patients’ discomfort after procedures and advise them to use analgesics that are appropriate for them and their specific procedures. A simplified protocol is presented below. Each of these medications should be used for short periods, no more than three to five days. Chronic pain is not common in dental practice; these regimens pertain to acute pain control.
Mild pain, such as the hyperemia of a pulp after an intracoronal restoration, can be treated with over-the-counter analgesic medications. Acetaminophen can be recommended, 650 milligrams every four to six hours, with no more that 4,000 milligrams in one day. Aspirin is another OTC analgesic that has some slight anti-inflammatory effect as well. The dosage of aspirin is similar to that of acetaminophen. Many patients complain of stomach upset with aspirin, and buffered or enteric-coated preparations are more tolerable. Also available over the counter is the 200 milligram ibuprofen tablet, recommended at 200 milligrams every four to six hours, with a limit of 1,200 milligrams per 24 hours.
Patients who may experience moderate pain, e.g., periodontal tissue manipulation, crown preparation, and extraction of a periodontally involved tooth, will benefit from the prescription of ibuprofen at 400 to 800 milligrams per dose. At this level, the analgesic property is joined by the anti-inflammatory effect of this medication. Many well-controlled studies of oral surgery patients have shown that ibuprofen can be just as good or better than opioid analgesics. A good rule is to prescribe this medication so that the patient takes the first dose before the local anesthetic wears off, and then be on the clock for at least the first 24 hours. Prescribe 400 milligrams every four hours, 600 milligrams every six hours, or 800 milligrams every eight hours, not to exceed 3,200 milligrams in one day. While the OTC 200 milligrams could be doubled, tripled, or quadrupled, the prescription doses are made to dissolve and absorb more quickly. It is likely that analgesia is equivalent, but the patient may experience less gastric distress with fewer pills. If the patient is also prescribed an antibiotic, make the ibuprofen dose parallel to improve compliance. A patient can get confused if he or she is supposed to take one prescription every four hours and another every six hours.
Severe pain is likely when periosteum and bone are manipulated. Extraction of bony-impacted teeth, periodontal recontouring, and endodontics beyond the apex are several examples of procedures that should have additional analgesic medications. I recommend the addition of a narcotic pain medication to the ibuprofen prescription for moderate pain. Many combination medications with opioids and acetaminophen or aspirin are available. These combinations help treat pain at the central nervous system (opioids) as well as the peripheral (acetaminophen or aspirin). Inflammation is not addressed with these combinations even though most dental treatments result in inflammation. Two examples of these combinations are Percocet (Endo Pharmaceuticals) and Tylox (Ortho-McNeil Pharmaceutical, Inc.). The first comes in different doses, such as 5 milligrams of oxycodone and 325 milligrams of acetaminophen. The second is 5 milligrams of oxycodone and 500 milligrams of acetaminophen. For each of these, the therapeutic dose of acetaminophen is not met with one pill, and taking two pills may lead to respiratory depression or somnolence as an effect of the higher dose of oxycodone. An alternative is to take one Percocet or Tylox and one OTC acetaminophen every four to six hours. Compliance decreases as the number of pills increases.
Combunox has recently become available (Forest Pharmaceuticals, Inc.). Each tablet contains 5 milligrams of oxycodone and 400 milligrams of ibuprofen. This combination provides the centrally active opioid and the anti-inflammatory and analgesic ibuprofen. The recommended frequency is one tablet every six hours, for a maximum of four tablets in 24 hours. For patients on antibiotics, this regimen is on the same clock, minimizing the number of pills needed. As with all opioids, the patient should be cautioned regarding side effects.
Conclusion
Pain management can be a simple yet important part of daily dental practice. Safety, reliability, and tolerability are keys for medications described here. Patient compliance and maintenance of health are achievable with these medications and are successful many times each day. Good reference tools are available to help determine the appropriate medications for our patients. 7,8,9
References
1 Septocaine package insert. Septodont USA, New Castle, DE. June, 2000.
2 Yagiela JA. Recent developments in local anesthesia and oral sedation. Compendium Contin Educ Dent 2004;25:697-708.
3 Malamed SF, Gagnon S, Leblanc D. Articaine hydrochloride: a study of the safety of a new amide local anesthetic. J Am Dent Assoc 2001;132:177-185.
4 Berde CB, Sethna NF. Drug therapy: analgesics for the treatment of pain in children. N Engl J Med 2002;347:1094-1103.
5 Clinical Research Associates. Non-injectable local anesthetic for periodontal administration. CRA Newsletter 2005;29(4):3.
6 Oraqix package insert. OraPharma, Inc., York, PA.
7 Lexi-comp, Inc. Lexi-comp Online software. Hudson, OH, 2006.
8 Gage TW, Pickett FA. Mosby’s Dental Drug Reference, 7th edition. Elsevier Mosby, St. Louis, Missouri, 2005.
9 Gold Standard Multimedia, Inc. Clinical Pharmacology software. Tampa, FL, 2006.
Wendy S. Hupp, DMD
Dr. Hupp is an assistant professor of oral medicine, College of Dental Medicine at Nova Southeastern University in Fort Lauderdale, Fla. She has been a member of AAWD since 1985 and is a founding member of the editorial board of WDJ. You may reach her at [email protected].