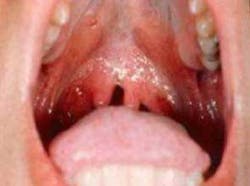
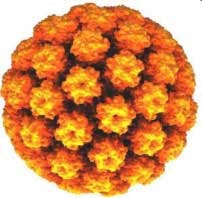
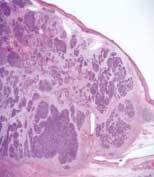
Oral cancer and the human papillomavirus: Part 1
High-risk genotypes of human papillomavirus (HPV) can be a contributing factor to oral carcinogenesis, especially in younger individuals without known risk factors such as tobacco and alcohol. Both the Centers for Disease Control and Prevention (CDC) and the American College of Pediatrics now recommend that both girls and boys be vaccinated against HPV. There is much debate about the HPV vaccination.
I will teach a class July 19, 2013, part of a Philips Sonicare Workshop at RDH Under One Roof, where we will discuss the risks that HPV brings and the link between HPV and cervical and oropharyngeal cancer; the pros and cons of the HPV vaccine; and oral cancer risks yesterday, today, and tomorrow. We will discuss how this was 100 years ago, and the potential of it morphing in the future to be something entirely different in another 100 years. This demonstrates how medicine and diagnosis, research and transmission are changing the world faster than ever before.
In 1990, John E. Watkins theorized about the next 100 years. "Photographs will be telegraphed from any distance.” "Americans will be taller by from one to two inches.” "Wireless telephone and telegraph circuits will span the world.” "Vegetables will be bathed in powerful electric light, serving, like sunlight, to hasten their growth.” Many of his predictions came true!(6) Years ago, aside from two known risk factors, tobacco use and drinking alcohol, health professionals were uncertain whether oral cancer was a viral or a genetic disease. Oral cancer remained a molecular black box that scientists could not open or explore. Most oral cancers were advanced by the time they were diagnosed, and mortality still remains high. Treatment options usually consisted of shrinking the tumor with radiation, followed by head and neck surgery to remove it. Today we know that oral cancers are the sixth most common cancers in the world, and the known risk factors for oral cancer are tobacco use and alcohol consumption. Recently, infection with certain types of human papillomavirus (HPV) has been linked to oropharyngeal cancer. Research studies funded by NIH in 2010 include “Genome-wide discovery of molecular alterations in head and neck cancer” and “Comprehensive analysis of genetic alterations in oral cancer.”(7)A 2011 study: “Conclusion: Increases in the population-level incidence and survival of oropharyngeal cancers in the United States since 1984 are caused by HPV infection.”(12) The good news: “HPV-positive patients have substantially better survival compared to HPV-negative patients.”(12)
There are two alarming concerns with HPV16 oropharygeal cancer patients: the age of the victims that contract the virus; and the method in which it is often transmitted. Oral cancer contracted via the ingestion of alcohol and tobacco is most often associated with individuals who are well into life, often over the age of forty. HPV 16 varies from this immensely as it most often found in people in their 20s with no traces of alcohol or tobacco consumption, although there is an additive link between consumption of these and HPV 16. The ease of which HPV 16 is unknowingly transmitted lies in the fact that it is mainly transmitted by sexual contact.
Read Part 2 for more on this course and this topic!
Thanks to Philips Sonicare for its educational grant for this course.