Overcoming allergy roadblocks
Too often, dental professionals live with allergic reactions that can be treated
By Curtis P. Hamann, MD, Pamela Rodgers, PhD, and Kim Sullivan
Rubber has been utilized in protective devices since at least 1600 B.C. when native Mesoamericans used it for waterproofing. After modern vulcanization processes were developed in the late 1800s, rubber was incorporated into wide range of products, including gloves. Rubber surgical gloves gained popularity around the turn of the century after their adoption by surgeons at Johns Hopkins Medical School. By the late 1920s, however, the first medical articles had appeared describing workers with allergies to their rubber gloves.
There are two types of allergies associated with exposure to rubber products — type IV (or delayed) allergy or type I (or immediate) allergy. A type IV allergy is a localized immune reaction of the skin to residual processing chemicals in natural and synthetic rubber products. These processing chemicals are a necessary addition during rubber manufacture and improve product elasticity, resiliency, and durability. Today, thiurams and carbamates are commonly used in rubber glove manufacture, whereas mercaptobenzothiazoles are rarely found.
Type IV allergic reactions also can occur to dental chemicals other than the residual processing chemicals in rubber gloves. The more common allergenic compounds include methacrylates (bonding agents) and glutaraldehyde (surface disinfectants). Symptoms of these type IV allergies to various dental chemicals include diffuse or patchy eczema, itching, redness and vesicles, thickened dry skin, fissures, and sores. These symptoms begin to develop within hours, but can last for several weeks.
A type I NRL allergy is a whole-body immune reaction to the plant-based proteins found in natural rubber latex (NRL). These immune reactions result from circulating anti-NRL antibodies that recognize NRL proteins absorbed through the skin, blood, or lungs. Once recognized, a rapid cascade of events begins much like in a pollen or food allergy. Generally, type I symptoms such as sneezing, itchy eyes, and hives develop and subside quickly. This type of allergy also can progress to life-threatening anaphylactic shock, requiring urgent medical care.
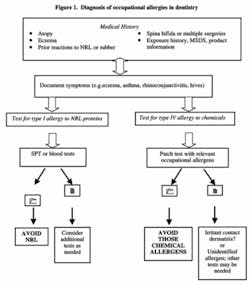
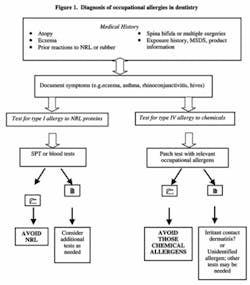
Determining which type of allergy plagues a dental worker is a multi-step diagnostic process (fig. 1). First, a comprehensive health history is taken. This can identify important risk factors such as existing allergies or allergic reactions, regular exposure to rubber products, previous reactions to rubber, and multiple childhood surgeries or spina bifida. Relevant symptoms also are documented along with information on their frequency and duration, and sources of potential chemical exposure.
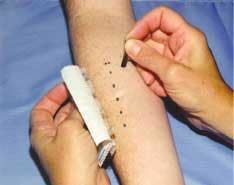
Individuals suspected to be allergic should be tested for type I NRL protein allergy, type IV allergy to rubber chemicals, or both. Patch testing (fig. 2) measures localized skin responses (type IV chemical allergy) to different chemical allergens, including rubber-processing chemicals. Skin-prick testing (fig. 3) and blood testing measure circulating antibodies to NRL proteins; either method can diagnose a type I NRL allergy. Most methods are not new, but have been used successfully to assess rubber-based allergies for several decades.
Unfortunately, practical evidence-based health care is not always employed. Despite the availability of diagnostic tests and solutions, health-care workers suffer with occupational skin disease for three years on average before obtaining treatment. The resulting chronic skin disease can lead to serious disease transmission, lost productivity and may precipitate career changes.
Worker and physician misconceptions may limit the pursuit of solutions to occupational allergies. In a recent case, a dental worker with severe chronic skin disease was convinced that she had a "latex" allergy that could be resolved with the "right glove." Unremitting redness and itching as well as cracked and bleeding fingertips threatened her livelihood. The worker was misinformed and had been poorly diagnosed. Finally, after appropriate testing, counseling, and training, this dental professional was able to work without the symptoms that had been so debilitating for more than a decade.
This scenario is not unusual. Dental professionals often erroneously assume their skin problems are due to a "latex" allergy. However, nearly three-quarters of these workers test negative for a latex allergy (type I NRL protein allergy). Moreover, the prevalence of latex allergy appears to be decreasing, perhaps due to the changes in glove standards for powder and NRL protein, as well as the increased use of low-allergen latex, powder-free latex, and synthetic rubber gloves.
If the skin on your fingertips cracks and bleeds, is it an allergy, or are your hands irritated by frequent hand washing or harsh weather? Unfortunately, dental workers and physicians poorly identify these conditions. More than 20 percent of dental professionals report symptoms of dermatitis. Far fewer actually test positive to allergens commonly found in dentistry. Allergists are more likely than dermatologists to conduct appropriate diagnostics, but not all perform the full battery of skin prick, serologic, and patch tests needed to correctly identify the source of occupational allergies. In the case described above, the dental worker with chronic skin disease was never tested for type I or type IV allergy and, despite unsuccessful treatment by different physicians, the initial assumption of a "latex allergy" was not revisited.
To complicate matters, the number of workers testing positive for type IV allergies to dental chemicals appears to be increasing. Current studies indicate that 10 to 22 percent of patch-tested dental workers are allergic to methacrylates (dental bonding agents), which may reflect the increased use of these materials throughout dentistry. Also corresponding to its increased use in the rubber glove industry, 7 to 14 percent of patch-tested dental workers are allergic to thiurams. In addition, 4 to 10 percent of patch-tested dental workers are allergic to disinfectants and preservatives, such as glutaraldehyde, thimerosal, benzoic acid, formaldehyde, and glyoxal.
Dental professionals and their physicians are frequently unaware of chemical hazards in the operatory and at home. Not surprisingly, few dental workers report having chemical safety training or guidance on effective barrier methods. Dental workers must learn to read ingredient labels, product inserts, and MSDS information, and become familiar with common chemical names (including brand names and synonyms). With the help of their physicians, they can chronicle potential chemical exposure and personal protective equipment as well as any corresponding patterns of symptom frequency and duration. This information can be invaluable in deciphering a complex mix of occupational allergies. In the above case study, the worker's skin reactions to bonding agents (dental and artificial fingernails), natural and synthetic rubber gloves (all containing thiurams), and disinfectants were highly consistent with her chemical exposure patterns at work and at home.
In addition to the roadblocks described above, dental workers can be reticent to change current habits. In the current case example, until retrained, this worker continued to be exposed to chemical allergens and be symptomatic. Ultimately, patient education is key to long-term successful management of occupational allergies. Physicians or professional organizations must provide guidance and training. The impact of personal preferences, work styles, work environments, and coworker attitudes also should be considered. Enlisting the assistance and support of family, friends, and coworkers is more likely to guarantee abatement of allergy symptoms long-term.
In summary, dental professionals are at risk for the development of occupational skin disease because of their frequent exposure to the chemicals in bonding agents, rubber gloves, disinfectants, adhesives, soaps, and preservatives. To prevent serious consequences, dental workers must receive appropriate diagnostics and correct information about chemical allergens. They must be trained to recognize and avoid these substances — at work and at home. As innovators and leaders in their fields, professional dental and medical organizations and educational institutions should provide resources and foster increased awareness of the importance of recognizing occupational allergies. When these roadblocks are overcome, the management of occupational allergies in dental professionals will be successful.
Editor's Note: References available upon request.