Positioning for success
Essential ergonomic guidelines for dental hygienists
by Bethany Valachi, PT, MS, CEAS
Twenty-five heads bowed reverently over their colleagues, diligently scaling the upper arch. From the back, one would assume that the students were not wearing loupes, but from the side, a different reality became apparent. The students were working on the upper arch with the occlusal plane angled slightly forward of vertical, causing excessive leaning and straining forward — even to see into the mirror. When the occlusal plane was tipped backward about 15 degrees, the postural transformation was amazing.
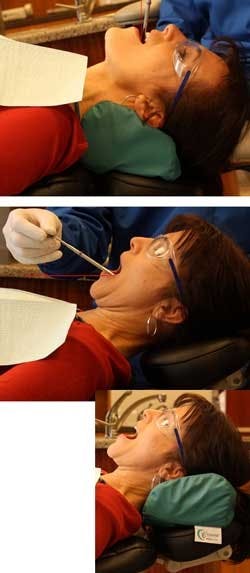
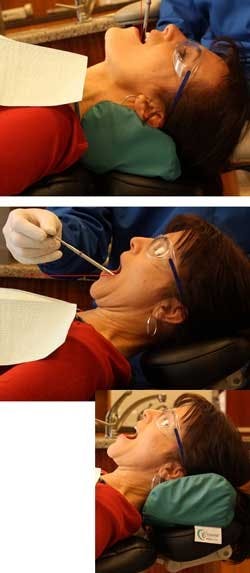
This is one of the most common ergonomic mistakes I observe (not only in the schools, but also amongFigure 1a, b: An ergonomic dental cushion (Crescent Products) will increase patient tolerance to being reclined when treating the upper arch, and facilitate proper positioning (top). Angle the headrest slightly forward when treating the lower arch (bottom), or reverse a contoured dental cushion (inset). (Photo ©2010 from “Positioning for Success” DVD)
Not feeling any pain ... yet? Is a tooth completely healthy unless your patient is experiencing pain? The progression to a musculoskeletal disorder (MSD) in dentistry is a slow, insidious process, and the proof is in the numbers:
- An average of two out of three dental professionals experience occupational pain.1-12
- Nearly a third of dentists who retire early are forced to do so because of a musculoskeletal disorder.13
- In 2004, approximately $131 million was lost in income due to MSDs in the dental profession.14
The causes of MSDs in dentistry are multifactorial, ranging from nonergonomic loupes to improper selection of delivery system, as well as to generic exercise that worsens muscle imbalances. However, proper patient positioning techniques can go a long way in preventing the progression toward chronic pain or potential injury in dentistry. In fact, it has been shown that dental hygienists who take the time to carefully position their patients to promote a direct view have significantly fewer headaches.15 Patient positioning techniques will vary slightly depending upon the quadrant being treated, the patient’s tolerance to reclining, and patient chair shape and width.
Operator posture
First, it is imperative that the hygienist is seated properly and the stool is correctly adjusted.16
From an ergonomic standpoint, the operator stool is the most important chair in the treatment room. Its adjustment can profoundly impact posture and musculoskeletal health. Positioning in the operatory should always begin with adjusting the operator stool first, then the patient. Ideally, the stool should be used by only one operator to prevent repeated adjustments. Keep in mind that a stool is only ergonomic if it adjusts to fit your body size and shape. When shopping for stools, it is wise to utilize unbiased product reviews.
The sequence for adjusting a traditional operator stool is as follows:
- Adjust the backrest height so the most convex portion (the lumbar support) nestles in your low-back curve. On most dental stools, there is no recognizable lumbar support. On these stools, adjust the backrest to a height where the shape fits most snugly against the curves of your back.
- Move the backrest away from your back, which enables you to sit all the way back on the seat pan.
- Check for appropriate size of the stool by placing three finger-widths behind your knee.
- If the closest finger touches the seat, the seat pan is too deep, and you should select a stool with a shorter seat.
- If your stool has a tilting mechanism, tilt the seat very slightly forward, only five to 15 degrees.
- Adjust the height with your feet flat on the floor until your thighs slope slightly downward. Your weight should be evenly distributed in a tripod pattern: through each foot on the floor and through your buttocks. If, at the highest adjustment, your thighs are still parallel to the floor, you may need to order a tall cylinder from the manufacturer.
- If the stool has armrests, adjust them one at a time to a height where the shoulder is not visibly elevated when compared with the opposite shoulder, yet the arm is fully supported.
If there is no tilting seat feature on the stool, an ergonomic wedge cushion may be used to retrofit the stool and attain proper posture.
Saddle stools are becoming increasing popular among dental hygienists, since they are very easy to move around the head of the patient, facilitate proper posture at the 9 o’clock position (see Figure 2), and are ideal for confined operatory spaces. Because of its shape, it places the pelvis in a neutral position, so the spinal curves can more easily balance and also minimizes the need for backrest support. Saddle stools are especially beneficial for shorter operators. By opening the hip angle, they allow lower positioning of the patient, and a more relaxed arm and shoulder posture. Saddle stool height should be adjusted so the thighs slope downward at about a 45-degree angle.
Patient positioning
Since the hygienist moves frequently around the head of the patient during treatment, they will ask the patient to rotate the head or tilt the chin during treatment to attain a line of sight that is perpendicular to the tooth surface.
Ideally, the patient should be positioned supine for treating the upper arch and semi-supine for the lower arch. However, in the real world, time constraints and practicality usually prevent the hygienist from such luxuries.
Therefore, it is recommended that the chair back be positioned so it is elevated 10 to 15 degrees from the floor (use the preset control of the patient chair to set this angle) and left in that position throughout the treatment. Proper orientation of the occlusal plane can then be achieved using a contoured dental neck cushion for treating the upper and lower arches. Ensure that the positioning aid is not too large, or it will be counterproductive, forcing the patient’s head forward. Many “dog-bone” pillows I have seen in operatories cause such positioning.
After reclining the chair, ask the patient to scoot to the end of the headrest. This is especially important if using a flat headrest — reaching or leaning over the “dead” headrest space can lead to a myriad of musculoskeletal dysfunctions.14 Often, this is not done in deference to the patient’s comfort — their spinal curves may not align properly with the patient chair support when scooted up all the way to the end of a headrest. This is easily resolved with dental ergonomic cushions that support the patient’s neck, low back, and knees.
When treating the upper arch, adjust the headrest so the occlusal plane of the upper jaw is about 15 to 20 degrees backward in relation to the vertical plane. You can check for proper positioning from the side, using an instrument handle to visualize the angle of the occlusal plane (see Figures 1a, b). This angle is most easily attained with double-articulating headrests — by angling the headrest upward into the patient’s occiput. On flat headrests, use a contoured dental pillow with the large end under the patient’s neck, to angle the head back and chin higher. Then, adjust the height of the patient chair so forearms are parallel to the floor or sloping 10 degrees upward.17 Whether using flat or double-articulating headrests, contoured memory foam cervical support cushions will make the patient much more tolerant to reclining.
In the 8 to 9 o’clock position, the hygienist can treat the upper posterior and anterior surfaces facing toward the hygienist, remembering to ask the patient to rotate their head to preserve their own best working posture. For example, ask the patient to turn their head slightly away when treating the upper right facial surfaces, and for the anterior facials, ask the patient to turn their head toward you. Sidesitting in the 8 to 9 o’clock position is one of the most damaging positions the hygienist can assume, and should be eliminated or minimized to avoid injury. This can lead to pain and musculoskeletal disorders in the hips, back, shoulders, neck, and arms. Always try to face the patient directly during treatment. A saddle stool can help greatly with gaining close proximity in the 8 to 9 o’clock position (see Figure 2).
A majority of the upper arch should be treated from the 11 to 1 o’clock positions, using direct or indirect vision. Mirrors should be used whenever direct viewing of the oral cavity requires leaving neutral posture. One study revealed that more pain-free dental professionals use a mirror than those who did not use a mirror.18 Frequent positioning at the 10 o’clock position without a mirror tends to encourage more arm abduction and neck/shoulder problems.19 The hygienist must remember to reposition the delivery system when moving around the head of the patient. Handpieces and instruments should be at about elbow level. Finger fulcrums are important to increase stability and to reduce compression in the carpal tunnel.
As the hygienist moves around the patient, the overhead light must be repositioned to prevent shadowing. The light should parallel the hygienist’s line of sight to within 15 degrees. Thus, the light will be placed slightly behind and to one side of their head. To avoid repeated upward reaching for the light, the hygienist should consider a lightweight head-mounted light, which will parallel even more closely with the operator’s line of sight to prevent shadowing20 (see Figure 3). Dr. Lance Rucker, professor and chairman of operative dentistry in the Department of Oral Health Sciences at the University of British Columbia has done valuable research in this area. For the upper arch, a mirror may be used to reflect light onto the surface.
When treating the lower arch, adjust the headrest so the occlusal plane of the lower arch is about 30 degrees elevated from the horizontal plane (see Figure 1b). On a double-articulating headrest, angle the headrest slightly forward, so the patient’s chin tilts downward. On flat headrests, reverse the position of a contoured dental cushion, so the large end is behind the head. It may be necessary to slightly lower the height of the patient chair so forearms are parallel to the floor or sloping 10 degrees upward.
Some hygienists may find that the chair does not adjust low enough to allow proper, relaxed arm posture. In this case, a saddle stool may be used to raise the hygienist to a higher seated position, since this places them between standing and sitting.
The hygienist should watch their wrists as they move to different quadrants to ensure a safe, neutral wrist posture. If the wrist is excessively flexed, a different clock position should be explored to enable a straight wrist posture.
With tight patient schedules, emergencies, and productivity goals to consider, it is easy to overlook proper patient positioning. However, taking the time to position the patient, hygienist, and equipment properly can not only have positive ramifications for the operator’s posture, comfort, and career longevity — it can also lead to better treatment and increased productivity.
Author’s note: This article is based on the educational DVD, “Positioning for Success in Dentistry.” Hygienists can earn 2 CEUs with the DVD, which also contains assistant, dentist, loupes, and wheelchair positioning techniques. The DVD, downloadable tests, as well as demo video clips are available on her website at www.posturedontics.com. Faculty and student discounts are available.
Bethany Valachi, PT, MS, CEAS, is a physical therapist, dental ergonomic consultant, and author of the book, “Practice Dentistry Pain-Free: Evidence-based Strategies to Prevent Pain and Extend Your Career.” Ms. Valachi is CEO of Posturedontics, a company that provides research-based dental ergonomic education, and clinical instructor of ergonomics at OHSU School of Dentistry in Portland, Ore. She is a member of the National Speakers Association, lectures internationally, and may be reached at [email protected]. She offers free articles, newsletters, videos, and continuing education on her website at www.posturedontics.com.
References
1. Akesson I, Schutz A, Horstmann V, Skerfving S, Moritz U. Musculoskeletal symptoms among dental personnel; - lack of association with mercury and selenium status, overweight and smoking Swed Dental J 2000;24:23-28.
2. Alexopoulos EC, Stathi I, Charizani F. Prevalence of musculoskeletal disorders in dentists. BMC Musculoskelet Disord 2004;5:16.
3. Auguston TE, Morken T. Musculoskeletal problems among dental health personnel. A survey of the public dental health services in Hordaland. Tdsskr Nor Laegeforen. 1996;116(23):2776-80.
4. Chowanadisai S, Kukiattrakoon B, Yapong B, Kedjarune U. Occupational health problems of dentists in southern Thailand. Int Dent J 2000;50:36-40.
5. Fish DR, Morris-Allen DM. Musculoskeletal disorders in dentists. N Y State Dent J 1998;64(4):44-48.
6. Finsen L, Christensen H, Bakke M. Musculoskeletal disorders among dentists and variation in dental work. Applied Ergonomics 1997;29(2):119-125.
7. Lehto TU, Helenius HY, Alaranta HT. Musculoskeletal symptoms of dentists assessed by a multidisciplinary approach. Community Dent Oral Epidemiol 1991;19:38-44.
8. Marshall ED, Duncombe LM, Robinson RQ, Kilbreath, SL. Musculoskeletal symptoms in New South Wales dentists. Aust Dent J 1997;42(4):240-6.
9. Ratzon NZ, Yaros T, Mizlik A, Kanner T. Musculoskeletal symptoms among dentists in relation to work posture. Work 2000; 15:153-8.
10. Rundcrantz B, Johnsson B, Moritz U. Cervical pain and discomfort among dentists. Epidemiological, clinical and therapeutic aspects. Swed Dent J 1990;14:71-80.
11. Rundcrantz B, Johnsson B, Moritz U. Occupational cervico-brachial disorders among dentists: Analysis of ergonomics and locomotor functions. Swed Dent J 1991;15:105-15.
12. Shugars DA Miller D, Williams D, Fishburne C, Strickland D. Musculoskeletal pain among general dentists. Gen Dent 1987;35:272-6.
13. Burke FJ, Main JR, Freeman R. The practice of dentistry: an assessment of reasons for premature retirement. Br Dent J 1997;182(7):250-4.
14. Valachi B. Practice Dentistry Pain-free: Evidence-based Strategies to Prevent Pain and Extend Your Career. Portland, Oregon: Posturedontics Press; 2008:5.
15. Rundcrantz B, Johnsson B, Moritz U. Cervical pain and discomfort among dentists. Epidemiological, clinical and therapeutic aspects. Swed Dent J 1990;14:71-80.
16. Valachi B. Operator Stools: How Selection and Adjustment Impact your Health. Dent Today. 2008 Sep;27(9):148, 150-1.
17. Chaffin D, Andersson G, Martin B. Occupational Biomechanics. 3rd ed. New York: John Wiley & Sons Inc; 1999:355-391.
18. Rundcrantz B, Johnsson B, Moritz U. Occupational cervico-brachial disorders among dentists: Analysis of ergonomics and locomotor functions. Swed Dent J 1991;15:105.
19. Proteau R. Prevention of work-related musculoskeletal disorders in dental clinics. Montreal, Quebec: Association pour la sante et la securite; 2003. Available at: http://www.asstsas.qc.ca/english/publication.asp. Accessed July 31, 2007.
20. Rucker LM, Sunell S. Ergonomic Risk Factors Associated with Clinical Dentistry. CDA J 2002;30(2):139-48.
Past RDH Issues