Case study of a challenge: Prevention education and implementation in Zambia, Africa
The author participated in 10-day mission trip to Zambia.
By Amy Tedford
Abstract
In Zambia, Africa, many infectious and chronic diseases are causing years of life lost (YLLs) due to premature mortality in the population. Oral health-related quality of life is equally as important in developing countries with limited access to good oral health care systems. Prevention is key, and with education and efficient implementation, the oral health and overall health of Zambians could vastly improve.
The utilization of established organizations, such as International Caring Hands, Caring Hands Worldwide, Mercy Ships, and more to educate the population about prevention and distribute as many toothbrushes as possible would aid in the improvement of oral health and overall health. In Zambia, these organizations could also create a demand for toothbrushes in the rural markets and test for HIV/AIDS with oral fluid tests while addressing an array of dental problems. It is key that the importance of oral health preventative strategies not be degraded. Existing structures, churches and schools, urban dental and medical clinics, and rural clinics can be used in the promotion of preventative oral health and market systems for the access of preventative instruments (i.e. toothbrushes and toothpaste).
If the proposed implementation occurred, conducting a large study on prevalence of self-reported hygiene and knowledge of oral hygiene would be indicative of progress. But ultimately, spending time in Zambia, being immersed in the culture, and being observant of changes in oral health habits and behaviors would be most indicative. The successful implementation would be a multi-year process; it would not happen overnight. Therefore, it would not be plausible to conduct a large study until five or more years after implementation.
Introduction
Poor oral health can be attributed to many factors, all of which will be addressed in this paper. They include inadequate health care systems, limited access, little to no oral health prevention education, degrading of importance of preventative oral health care, and lack of funding, providers, and modern equipment. The purpose of this paper is to propose realistic methods to attain improvement in oral health habits and behaviors in group and individual levels through the utilization of existing structures and organizations.
The proposed implementation is not an overnight fix because there is not enough funding or resources. It is a gradual process, as any sought after change in behaviors and habits tend to be. Effective prevention of oral health conditions common to Zambia could lessen the overall burden of oral health-related impacts on daily life. If the proposed implementation were successful, it could be modeled in other countries with similar limitations to achieving good oral health. It is important to remember that oral health care is just as important in third world countries as it is in developed countries.
Background
Zambia, Africa is slightly larger than Texas, at 752,618 sq km. It is landlocked by seven surrounding countries and has a population of 15,510,711, 40.9% of which is urban (2015). Zambia is very linguistically diverse with allegedly over 70 languages, many of which are considered dialects. Zambians have more children per household, with a birth rate of 41.8 births/1,000 population (fourth highest of all countries). The 2016 estimate for Zambia’s GDP was $65.17 billion, of which the health expenditure accounts for 5%.(1)
Urban versus Rural. A phone interview with Brandy O’Connor, a registered nurse and missionary with Overland Missions, made it apparent that city life vastly differs from life in the rural villages. O’Connor has spent seven to nine months each year in a rural village near Livingstone, Zambia, for the past six years. O’Connor and her husband are there with Overland Missions, a Christian organization, and she is, therefore, very familiar with life in the rural villages as well as in the city.
Livingstone is very close to Victoria Falls, the largest waterfall in the world, which makes the city a beacon for tourism. Citizens of Livingstone are typically either members of the upper or lower class; there is no middle class.(2)
O’Connor stated that villagers live in mud huts with grass roofs and use a long-drop system for their bathroom needs. A long-drop system is a deep hole in the ground that once full, is covered with dirt and a new hole is dug. The village O’Connor lives in has a well for water, but not all do.(2) According to the CIA World Factbook, 48.7% of the rural population has an unimproved drinking water source.(1) Other water sources include a nearby river or pools of water that have collected during the rainy season. The water is boiled before consumption and is used for bathing as well. There are no additives in the village drinking water.
Zambians eat corn with every meal. Their staple dish, nsima, is mashed corn that takes on an almost mashed potato appearance and consistency. Nsima is often served a with a relish, which may be beans, collard greens, cabbage, or on rare occasions, rehydrated fish or goat. They typically do not eat cow because cattle are their currency; the exception being when cattle die from old age.
In the village, everyone is basically at the same level of poverty. The villagers typically do not have any means of transportation besides walking. They may have an ox-cart, but it is rare. Village health clinics are two to three hours away by means of walking. Therefore, they only seek medical attention if seriously ill (i.e. malaria or infected cut) or for maternal services, since maternal care is heavily pushed by the Zambian government.(2)
Villagers will often seek out witchdoctors for health problems, family problems, etc. Witchdoctors are in every village and very well known among the villagers. They will give charms, potions, or perform animal sacrifices. For generations, witch doctors have been sought after because they were easily accessible, and they are sought after for the same reason today.(2)
The city has a hospital and many clinics, in addition to the well-known “traditional doctors”/witch doctors While walking in the city, flyers are often handed out advertising “traditional doctors” as well as large billboards.(2)
Problem Context
According to O’Connor, visually, rural children seem to have good oral health because they have a diet that consists of less of the sugary foods and beverages often consumed in developed countries, while adults often have decayed teeth and/or missing teeth.(2) The expected lifespan at birth for residents of Zambia is 52.5 years of age.(1) Their diet is predominantly a soft diet, but people do report not being able to enjoy foods they would like to.
The accessibility of preventative instruments, such as toothbrushes, toothpastes, and floss, is almost nonexistent for rural Zambians. O’Connor stated that she has seen few villagers with toothbrush and toothpaste because they are not easily attainable. She went on to say, “It’s not a common thing for every person in the village have a toothbrush or toothpaste. If you are a villager who has a toothbrush, you probably don’t have toothpaste. But to get those things, yes, they would have to go to the city and purchase those.”(2)
Markets are common in the city. They sell items indigenous to the area as well as necessities for tourists (sunscreen, lotion, etc.). City vendors love to trade tourists for items such as lotion, toothpaste, and hair ties because they are in high demand among other tourists and fellow citizens.
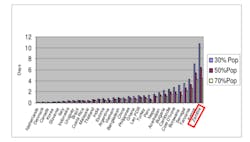
For citizens, these items are often too expensive for them to purchase on their own because of high demand among tourists. “[City vendors] will trade anything with you pretty much…The cost of toothpaste for the average worker in the market is expensive. I don’t know the equivalent it would be to us, but it would be more a luxurious item. So if they can trade it for a bracelet, they are going to,” O’Connor said.(2) Figure 3 shows the days of household expenditures to pay for toothpaste needed by one person for one year at the lowest price of toothpaste; 39 countries were involved in the study, and of all the countries, toothpaste in relation to household expenditure is most costly for Zambians.(3)
The short report Self-reported poor oral hygiene among in-school adolescents in Zambia (2011) suggests oral hygiene is poor among adolescents, but does not confirm causation due biases, misreporting, missing data, limited sampling population, and that fact that no “clinical parameters or indices of plague or gingival status were collected.”(4) The researchers used the 2004 Zambia Global School-Based Health Survey (GSHS) to attempt to determine the oral hygiene habits among adolescents, most of which were 13-15 years of age. They did not state whether the schools involved in the survey were urban or rural, but the assumption that they were urban can be drawn from the following statement: “each school’s chance of being selected was proportional to its enrollment size.”(4)
The 2004 GSHS had a response rate of 75%, with 2,257 respondents; 53.9% of which were male, 42.2% drank alcohol, 37.2% smoked cannabis, and 82.5% went hungry. In addition, 30.9% of the respondents were females aged 13 years or younger.(4)
The researchers focused on the question “During the past 30 days, how many times per day did you usually clean or brush your teeth?” The responses included “I did not clean or brush my teeth during the past 30 days; 1 time per day; 2 times per day; 3 times per day; 4 or more times per day.”
Poor oral hygiene was only associated with the response, “I did not clean or brush my teeth during the past 30 days.” They concluded that overall 10% of the respondents had self-reported poor oral hygiene. Age was not consistently associated with self-reported poor oral hygiene, but alcohol drinking, cannabis smoking, and going hungry were positively associated. They recognized the limitations to their study, such as those previously stated and that it solely included school children, not drop outs.(4) With agriculture being the main occupation, it is plausible to conclude that a lot of students may drop out to help the family with farming and raising cattle.
Oral Health and Overall Health
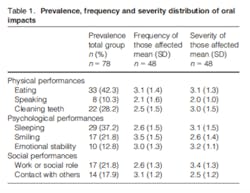
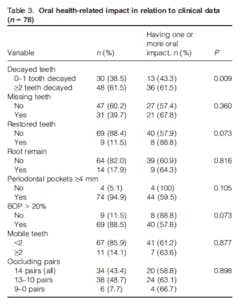
The article, The impact of oral health on daily performances and its association with clinic variables in a population in Zambia (2014), discusses a study conducted at a dental clinic in Livingstone, Zambia. The study involved 78 subjects, ranging 15 to 48 years of age that were “consecutively recruited in connection with a dental care visit.” Oral health affected one or more daily performances during the last six months for 61.5% of the subjects.
The oral impacts included in the study were physical performances, psychological performances, and social performances, which were then broken down into subcategories (see Figure 4). “Difficulty of eating and enjoying food” was the performance reported most frequently affected (42.3%). Figure 5 shows the variety of dental conditions experienced by the patients who actively sought dental care. The majority had periodontal pockets greater than or equal to 4 mm (94.9%) (mean 4.3+2.6), while 88.5% had gingival bleeding on probing >20%.(5)
The researchers concluded that there was a significant association between decayed teeth and oral impacts on daily performances. They attributed the array of dental conditions to more modern standard of living in cities, which has brought about increased sugar consumption.(5) An emerging problem is that sugar is available in rural markets, while toothbrushes and toothpastes are not.(2) The dental conditions can also be attributed to an increase in smoking in low- and middle- income countries, lack of utilization of health systems due to cost and transportation, and lack of health professionals and equipment, which often limits dental care to pain relief and emergency care exclusively.
The researchers of this study came to an agreeable conclusion. “In third world countries where agriculture is the main occupation, illiteracy remains, and people neglect their oral health because of lack of knowledge. With more knowledge about the importance of good oral health and its relation to daily life, people would hopefully improve their oral habits.”(5)
Implication of Problem/Proposed Implementation
Theutilization of established organizations, such as International Caring Hands, Caring Hands Worldwide, Mercy Ships, and more, as well as established structures, such as churches and schools to educate the population on the group and individual level about prevention and distribute as many toothbrushes as feasibly possible could aid in the improvement of oral health. In Zambia, these organizations may be able to create a demand for toothbrushes in the rural markets and test for HIV/AIDS with oral fluid tests while addressing an array of dental problems. Currently, oral fluid tests for HIV/AIDS are rather expensive but have many advantages in comparison to blood-based antibody tests for both the patient and provider.(6)
Caring Hands Worldwide is a Christian-based organization currently providing dental care in Chuuk, Micronesia. Chuuk has one of the worst ratios of dental providers to citizens in the world, and no private dentist to serve a population of approximately 50,000 people. Caring Hands Worldwide utilizes shipping containers with operatories and dental equipment. They utilize volunteer dentists, dental hygienists, and dental assistants for a minimum of two weeks. The volunteers stay in housing provided by the organization, but are required to pay for their air fare. Caring Hands Worldwide has the goal to eventually modernize emergency service in the Chuuk hospital and later “retrofit one of their buildings for a five-operatory dental clinic,” which is very ambitious.(7)
Rachel Hymes, DMD, went on a dental mission in Zambia in June 2014 through the Christian-based organization, International Caring Hands (ICH). ICH has fully-stocked mobile dental units in several countries in South Africa and around the world. Hymes spent her mission in Kafue, Zambia, a town in the Lusaka Province (see Figure 1). Hymes was responsible for purchasing air fare and any excursions, while ICH took care of Hymes’ transportation, food, and lodging while serving the community.
The mobile unit had two functional dental chairs, an overhead light, attachments for handpieces, an autoclave and ultrasonic, suction, personal protective equipment, cleaning supplies, and materials for restorations. The unit had a generator, air compressor, and air conditioner. Hymes said, “Anything I could think to use was there.”(8)
Prior to Hymes arrival, she requested that a local assistant aid in the operation of the clinic. ICH set her up with a local assistant, Lucas, from Lusaka who was instrumental in gaining the trust of the patients. Advertising occurred in surrounding villages that dental procedures would be available on a first come, first serve basis before Hymes’ arrival. On the first morning, patients were lined up before Hymes had the clinic ready. The majority walked from the surrounding villages, but few were lucky enough to receive a ride from the few cars or trucks on their way to the city.
The clinic was open from 8:30 a.m. to 5:30 p.m., with the exception of a 30-minute lunch break. Hymes saw 30 to 50 patients per day, who ranged from 4 to 84 years of age and had a “variety of concerns.”(8). Hymes stated, “Originally, our plan was to do extractions as well as fillings, but because of the demand for extractions, we were never able to place any restorations or do any cleanings.”
Hymes did astounding work in Zambia, but it is important that the importance of oral health preventative strategies not be forgotten or degraded. She describe her last day performing dental care in Zambia:
Our final day was definitely the most difficult. When it came time to close the clinic, a number of the people who had been waiting all day in hopes of receiving a number and being seen continued to stay. We worked well into the night, but no matter how hard we tried, we were not able to see all those who stayed. It was heartbreaking to hear them ask, "When will you be back?" Lucas said this might be the only opportunity for them to ever get any dental work done.(8)
Mercy Ships is an organization that uses hospital ships to provide medical and dental care internationally. The hospital ships dock on the coastline of a country and while doctors and other medical professionals provide care on the ship, dentists, dental hygienists, and dental assistants travel into the nearby villages to provide dental care.(9)
All three of the organizations mentioned have limitations, such as lack of providers, lack of funding, and therefore, lack of resources able to be provided. Mercy Ships only work well for countries located along the coastlines.Therefore, the utilization of existing structures are necessary. Schools and churches can promote good oral health on group and individual levels and even be instrumental in HIV/AIDS epidemic. Zambia is predominantly Christian, with a religious demographic of 75.3% Protestant, 20.2%, Roman Catholic, 2.7% other (includes Muslim, Buddhist, Hindu, and Baha’i), 1.8% none (2010 est.).(1) Therefore, churches can be instrumental in prevention education.
The article “Health Promotion through existing community structures: a case of churches’ role in promoting rotavirus vaccination in rural Zambia” discusses the use of community health workers (CHWs) through churches to promote preventative health behaviors, specifically the rotavirus vaccine. Promotion took place over 13 months with four key messages. Nineteen churches participated in the study, within which CHWs delivered health messages to 890 women’s groups meetings. The overall reach of the intervention was to 37.0% of church-attending women, and the efficacy was 67.7% [10]. They concluded the following:
Implementing community health programs is often expensive and unsustainable, but the reach and efficacy levels achieved through existing structures like churches are encouraging in resource-constrained countries. Churches can be effective channels for delivering health prevention strategies to often difficult-to-reach rural populations.(10)
Schools can educate children on the importance of good oral health and preventative strategies early on. Studies have shown that behaviors and habits adopted by young children typically remain throughout their entire life. Therefore, intervening when in the young population may cause change in behaviors and habits for generations—that is, of course, if they are given access to the preventative instruments, i.e. toothbrushes and toothpaste, in addition to education. According to O’Connor, lotion is highly sought after in Zambia, and is available in urban and rural markets.(2) If a demand were created for toothbrushes and toothpaste, it is plausible to assume that they too would become available.
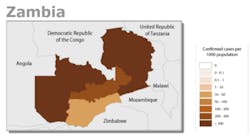
HIV/AIDS and malaria are prevalent in both urban and rural populations, and most often cause premature death when treatment is not sought after. The CIA World Factbook estimates that the HIV/AIDS prevalence is 12.91% (2015 est.), making it the seventh highest of all countries.(1) There are 4,184,661 malaria reported confirmed cases in Zambia (see Figure 2).(11) Screening for HIV/AIDS and malaria is available in rural clinics, but, as stated earlier, villagers are likely to only seek medical care in dire situations.
Government funding is likely to be spent on infectious diseases such as malaria and HIV/AIDS. Life expectancy is low in part due to these diseases, and the YLL are high. Oral health care may eventually be higher on the list of importance, but for now, utilizing existing systems seems to be the most realistic way to promote oral health prevention and importance.
The proposed implementation has not previously been done. Therefore, evidence cannot be provided for this proposed implementation. If it was implemented, conducting a large study on prevalence of self-reported hygiene and the knowledge of oral hygiene may be indicative of progress. But ultimately, spending time in Zambia, being immersed in the culture, and being observant of changes in oral health habits and behaviors would be most indicative. The successful implementation would be a multi-year process; it would not happen overnight. Therefore, it would not be plausible to conduct a large study until five or more years after implementation.
References
- CIA World Factbook. Zambia, Africa. https://www.cia.gov/library/publications/the-world-factbook/geos/za.html
- O’Connor, Brandy. RN and missionary, Overland Missions. Phone Interview. 19 April 2017 1:48 p.m. Duration: 29 minutes.
- Holmgren CJ, Yee R, Goldman AS, Benzian H. (2008). Global affordability of fluoride toothpaste. Globalization And Health, 4(1), 7. doi:10.1186/1744-8603-4-7.
- Siziya S, Muula AS, & Rudatsikira E. (2011). Self-reported poor oral hygiene among in-school adolescents in Zambia. BMC Research Notes, 4, 255. doi:10.1186/1756-0500-4-255.
- Andersson P, Kavakure J, & Lingström P. (2015). The impact of oral health on daily performances and its association with clinical variables in a population in Zambia. International Journal Of Dental Hygiene, 2015 Aug 18. doi:10.1111/idh.12171.
- Zachary D, Mwenge L, Muyoyeta M, Shanaube K, Schaap A, Bond V, Kosloff B, de Haas P, Ayles H. Field comparison of OraQuick ADVANCE Rapid HIV-1/2 antibody test and two blood-based rapid HIV antibody tests in Zambia. BMC Infect Dis. 2012 Aug 8;12:183. doi: 10.1186/1471-2334-12-183. PubMed PMID: 22871032; PubMed Central PMCID: PMC3475053.
- Caring Hands Worldwide. http://caringhandsworldwide.org/about-us/.
- Dental Mission in Zambia. Rachel Hymes, DMD. 22 December 2014. http://www.dentaleconomics.com/articles/print/volume-104/issue-12/features/dental-mission-in-zambia.html.
- Mercy Ships https://www.mercyships.org/who-we-are/
- Wesevich A, Chipungu J, Mwale M, Bosomprah S, Chilengi R. Health Promotion Through Existing Community Structures: A Case of Churches' Roles in Promoting Rotavirus Vaccination in Rural Zambia. J Prim Care Community Health. 2016 Apr;7(2):81-7. doi: 10.1177/2150131915622379. PubMed PMID: 26792908.
- Malaria Profile. WHO. http://www.who.int/malaria/publications/country-profiles/profile_zmb_en.pdf?ua=1.
- Map of Zambia, Africa. https://giving.colostate.edu/zambia-story/.