AO JOMI News: Implant-abutment interface configuration effects on dental implant therapy
Canine study finds implant-abutment interface configuration may influence crestal bone changes
This study was published in the September/October issue of The International Journal of Oral and Maxillofacial Implants (JOMI), the official journal of the Academy of Osseointegration (AO).
Background: Current implant protocols require not only osseointegration, but also high levels of soft-tissue stability and esthetics. Crestal bone changes and their impact on soft-tissue architecture are the most unpredictable and undesirable consequences of implant therapy, especially in the anterior maxilla. Hypotheses about the etiology of crestal bone remodeling around dental implants can be categorized into three main proposals: (1) mechanical factor that will disturb the surrounding tissues when occlusal forces are transmitted through the prosthetic component to the implant; (2) peri-implant inflammatory cell infiltrate caused by bacteria located at the implant/abutment microgap that will trigger crestal bone changes; and (3) adaptive response of the biologic width to the local condition not related to stress factors or inflammatory factors.
ADDITIONAL READING | AO, JOMI News: Accuracy of impression techniques, edentulous patients
Author: Dr. Santiago J. Caram, Department of Prosthodontics, Dental School, National University of Cuyo, Mendoza, Argentina, and Colleagues
Purpose: Scientists aimed to evaluate the peri-implant tissue response around different implant-abutment interface configurations when compared side by side. Two different soft-tissue adaptation variables and three different microgap interface variables were analyzed.
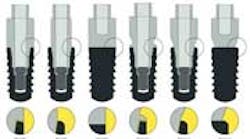
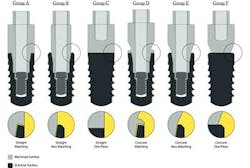
Materials and methods: Six different experimental implant abutment design groups — A to F — were evaluated in six mixed-breed dogs: (A) straight/matching; (B) straight/nonmatching; (C) straight/one-piece; (D) concave/matching; (E) concave/nonmatching; and (F) concave one-piece. At month 0, implant placement was performed and baseline standardized radiographs were taken. After three months of healing, standardized radiographs were taken and preformed titanium crowns were screw-retained to the top part of the abutments. Radiographs were taken every month for a period of six months. Dogs were fed a soft diet and implants were cleaned once each week with chemical and mechanical plaque control.
Results: All implants (72) integrated successfully and remained stable during the entire study period. When comparing radiographs of groups with straight profiles, crestal bone remodeling in Group C (one-piece design), was significantly less than in Group A (matching diameters) and Group B (nonmatching diameter). Implant Group C (one-piece design) showed the least crestal bone remodeling of all groups. When comparing radiographs of groups with a concave profile but different microgap configurations, all three designs demonstrated bone loss with no significant differences among the three groups.
ADDITIONAL READING | Implant dentistry news: Special preview of the Academy of Osseointegration 2015 Annual Meeting program
More information: To join AO and begin receiving JOMI (bi-monthly) or obtain online access to JOMI, visit: http://www.osseo.org/NEWmembershipApply.html.
About The International Journal of Oral & Maxillofacial Implants —
This highly regarded, frequently cited journal integrates clinical and scientific data to improve methods and results of oral and maxillofacial implant therapy. It presents pioneering research, seminal studies, emerging technology, position papers, and consensus reports, as well as the many clinical and therapeutic innovations that ensue as a result of these efforts. The editorial board is composed of recognized opinion leaders in their respective areas of expertise and reflects the international reach of the journal. Under their leadership, JOMI maintains its strong scientific integrity while expanding its scientific influence within the field of dentistry. It is published by Quintessence Publishing and is the official journal of the Academy of Osseointegration.
About the Academy of Osseointegration —
With 6,000 members in 70 countries around the world, the Academy of Osseointegration (AO) is recognized as the premier international association for professionals interested in implant dentistry. AO serves as a nexus where specialists and generalists can come together to evaluate emerging research, technology and techniques, share best practices, and coordinate optimal patient care using timely, evidence-based information. Follow AO on Facebook and Twitter.