Saving teeth through surgical endodontics
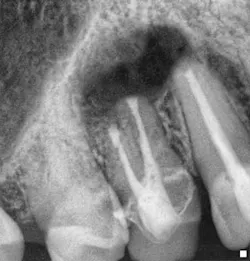
By Manish Garala, BDS, MSEndodontic surgery: an outdated clinical procedure?Endodontic surgery has developed the perception in some areas of dentistry as being an unpredictable and unnecessary procedure, especially with the advent of modern day implants. This opinion has been based on endodontic surgery being performed using outdated concepts and techniques that compromised the potential for clinical success, often resulting in the persistence of patient symptoms, periapical pathology, and, ultimately, extraction of the treated tooth (Fig. 1).
Fig. 1: Radiograph of a failing surgically treated endodontic case.The establishment of new surgical principles based on the use of enhanced magnification and illumination from the surgical operating microscope have addressed the technical and biological deficiencies that were previous barriers to successful, predictable surgical treatment.1The term microsurgical endodontics has now become synonymous with improved clinical success rates for endodontic surgical procedures, and scientific research has confirmed the merit of this procedure as more than just a last-ditch heroic attempt at tooth retention. Success rates of 90% and above have been reported from prospective case series and randomized controlled trials performed with contemporary techniques and protocols.2,3 The emphasis on using magnification for the identification of apical canal anatomy (Fig. 2), including additional canals, isthmuses, canal fins, and lateral canals (Fig. 3), apical disinfection of the root canal system, and the establishment of an impervious apical seal using biologically acceptable root filling materials such as MTA (Mineral Trioxide Aggregate, Dentsply Tulsa, OK) has enabled the routine achievement of these significantly improved success rates (Figs. 4 and 5).
Fig. 2: Microscopic image at 12x magnification of the MB, MB2, and DB roots of a maxillary molar that have been treated using a contemporary microsurgical technique.
Fig. 3: Endodontic surgery performed due to the development of a buccal sinus tract. A large lateral canal was identified microscopically at the site of the osseous defect located on the lateral root surface. Apical and lateral root preparation was performed using ultrasonics and the preparations sealed using MTA. The sinus tract healed and the tooth has remained stable in function for the last four years.
Fig. 4: Endodontic surgery performed without adhering to contemporary microsurgical principles. An apical seal is not evident and apical pathology has developed radiographically with associated swelling and symptoms.
Fig. 5: Microsurgical endodontics performed to correct the deficiencies in existing surgical treatment that took place less than six months ago. Apical repreparation performed using ultrasonics and MTA to create an ideal apical seal. A bone graft and resorbable membrane were used to maximize osseous and soft tissue healing. Microsurgical endodontics should be presented with confidence to patients as a potential treatment option for the management of clinical cases where there are ...
- Significant obstacles to the maximal intracanal disinfection of the canal space by nonsurgical endodontic retreatment. (Case 1)
- Unfavorable healing following conventional nonsurgical endodontic treatment, which results in persistence of symptoms or pathology. (Case 2)
- The management of apical pathology, which may not be of endodontic origin, and surgical biopsies may be necessary. (Case 3)
Fig. 6: Surgical preop radiograph.Endodontic treatment was necessary due to the presence of periapical pathology and acute symptoms, despite the radiographic appearance of the existing endodontic treatment being technically satisfactory. The presence of a long post, which is possibly serrated in nature and potentially actively engaging the root structure, is likely to compromise the potential for post removal and increase the risk of root fracture initiation, which would jeopardize the long-term survival of the tooth.
Fig. 7: Surgical postop radiograph.Surgical endodontic treatment was performed and the apical 3 mm to 4 mm of the root was reprepared using ultrasonics and sealed with MTA. A bone graft and resorbable membrane were placed to maximize the potential for osseous and soft tissue healing, especially with the proximity of the maxillary sinus to the surgical site. Case 2
Fig. 8: Retreatment preop radiograph.Note the less-than-ideal technical status of the existing RCT with an incomplete coronal seal.
Fig. 9: Sinus tract tracing with GP.Endodontic treatment was necessary due to the persistence of a buccal sinus tract that can be traced to the radiographic apex of tooth No. 10, despite recent endodontic treatment. Retreatment was performed and the sinus tract persisted, despite the adherence to strict protocols for intracanal disinfection and establishment of a technically satisfactory intracanal seal.
Fig. 10: Retreatment postop radiograph.
Fig. 11: Surgical postop radiograph.Surgical endodontic treatment was performed and the site of the periapical pathology debrided. No internal or external root fractures were detected, and a surgical seal was prepared at the apex of tooth No. 10 using MTA after ultrasonic preparation to ensure there was no potential for further recontamination of the apical tissues. A bone graft and resorbable membrane were placed to maximize the prognosis for osseous and soft tissue healing. The six-month recall radiographs show graft stability radiographically. There has been no recurrence of the buccal sinus tract, the periodontal attachment is intact, and the patient remains symptom-free. Case 3 Endodontic treatment was performed due to the development of buccal swelling and nonvitality on testing by an endodontic colleague. The sinus tract and buccal swelling persisted despite the ideal radiographic technical status of the treatment performed. Surgical treatment was indicated to manage the nonresolution of the presenting pathology.
Fig. 12: Postop RCT completion radiograph following intracanal placement of calcium hydroxide as an antimicrobial medicament for two weeks in an attempt to maximize intracanal disinfection.
Fig. 13: Six-week reevaluation appointment confirms nonhealing of buccal swelling or sinus tract, which was again traced to the osseous periapical breakdown site between the root apices of teeth Nos. 5 and 6.
Fig. 14: Immediate postoperative radiograph following microsurgical endodontics on buccal and lingual roots of Teeth Nos. 5 and 6.
Fig. 15: One-year postoperative radiograph demonstrating complete resolution of the periapical radiolucency and restoration of normal PDL (periodontal ligament) architecture radiographically.Microsurgery performed involved significant resection of the root apex of tooth No. 6 to enable complete osseous crypt curettage. Repreparation of the root apices of both teeth was performed using ultrasonics with no fractures visible on internal or external root surfaces that were exposed. Apical seals prepared using MTA. No bone graft or resorbable membrane was placed as this case was prior to its incorporation into surgical protocols. Biopsy results from the tissue located within the osseous defect revealed the presence of extraradicular periapical actinomycosis. This resulted in the need for antibiotic therapy for six weeks following microsurgical treatment completion. The patient has been recalled for the past eight years and remains symptom-free with no recurrence of the apical pathology. Tooth retention would not have been possible without complete crypt curettage that could not have been achieved without surgical intervention.ConclusionsThe above cases serve to highlight the numerous clinical situations in which surgical endodontics can be a predictable treatment option. There is no doubt that there is a high degree of clinical expertise required for the ideal technical standards to obtained in endodontic microsurgery, but this should not be used as an obstacle to the pursuit of this treatment option when indicated. This treatment modality will preserve the longevity of the tooth by its retention in function without symptoms or associated pathology. Ultimately, these are the factors by which our treatment should be assessed for clinical success and patient satisfaction.Author bioManish Garala, BDS, MS, received his dental degree in 1996 from Turner Dental School, University of Manchester, England. Between 1996 and 1999, he successfully completed his vocational and general dental practitioner degrees in private practice, Manchester, England. During this time, he developed a strong passion for endodontics, which led him to pursue a career as an endodontic specialist. He completed his postgraduate degree in endodontics at Nova Southeastern University, Ft. Lauderdale, Fla., in 2002, with a Master of Science in education, and became a diplomate of the American Board of Endodontics in 2007. Dr. Garala has been in specialist endodontic practice in Houston, Texas, since 2002, and is an adjunct assistant professor at Nova Southeastern University College of Dental Medicine. He is also adjunct faculty at UTMB Dental Branch of Houston. He has authored a number of scientific research papers focusing on root canal preparation using rotary nickel titanium instrumentation, and has also written a chapter in the comprehensive textbook by John McSpadden titled “Mastering Endodontic Instrumentation.” He has lectured extensively nationally and internationally. Contact him at [email protected].References1. Kim S, Kratchman S. Modern endodontic surgery concepts and practice. Journal of Endodontics, 2006; 32(7):601-623.2. Von Arx TJS, Hanni S. Clinical and radiographic assessment of various predictors for healing outcome one year after periapical surgery. Journal of Endodontics, 2007; 33:123-128.3. Taschieri S, et al. Endodontic surgery using two different magnification devices: Preliminary results of a randomized controlled study. J Oral & Maxillofacial Surg, 2006; 64:235-242.