Endodontic case study: back to the basics
All too often, many dentists in private practice lose sight of their basic sciences training and begin to base the rationale for their clinical procedures on old ideas, recommendations from dental sales representatives, or simple misunderstandings. Some treatment modalities are performed without thought, but rather are based on some continuing education course taken, whose main intention is to demonstrate a procedure purported to be “faster, cheaper, easier” and to increase production (and therefore income). This is particularly true in the specialty of endodontics where scientific concepts quickly fall victim to the “latest and greatest” craze that is usually unfounded in the scientific literature.
ALSO BY DR. ANTHONY BORGIA | The perio-endo overlap
Almost all dental disease is microbiological in origin, from caries to periodontal disease to endodontic involvement, with the notable exceptions being physical in nature (trauma, occlusal, etc.). Nevertheless, we have been conditioned to believe that to be successful in treating endodontic disease, we must “seal the apex” and “fill lateral canals,” ignoring the presence and ramifications of the true infection that is present within the root canal system. Without question, knowing and understanding microbiology is paramount to achieving endodontic success to a far greater extent than learning any obturation technique.
ADDITIONAL READING |We can't save them all: the missing endodontic diagnosis
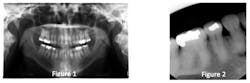
The case presented involves a mandibular canine that not only had a devitalized pulp, but also demonstrated a canal that had calcified for unknown reasons (Figs. 1 and 2). In addition to an asymptomatic periapical lesion, the patient presented with an extraoral fistula.
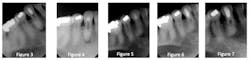
Several attempts at negotiating the canal were unsuccessful (Figs. 3 and 4), but after each visit, a thick mix of calcium hydroxide was densely packed into the preparation (Fig. 5). After approximately nine months, the lesion was seen to have resolved solely through the chemical reduction in the “bio load” present in the root canal system. The artificially created canal was then sealed with glass ionomer, followed by composite (Fig. 6). Of note, there is no sealer and no gutta percha anywhere in this tooth! One-year radiographic follow-up shows complete healing of the apical lesion (Fig. 7).
While this is obviously not a typical endodontic case, it clearly demonstrates that disinfection is paramount and of far greater importance than any system of obturation. An obturated, infected canal is or will be a clinical failure, whereas a sterilized canal that is protected from the reintroduction of microorganisms will be a clinical success.