Orthodontic treatment: assessing patient readiness
Maintaining oral health during orthodontic treatment can be a challenge for both the patient and clinician. It is imperative that patients receive a comprehensive oral evaluation prior to the start of orthodontic care. This will allow for an assessment of the effectiveness of the patient’s current oral hygiene practices. The clinician can also make a determination of whether the patient is willing and able to implement practices that will lead to the maintenance of gingival and tooth health throughout the course of treatment. During this evaluation, indices that measure oral hygiene should be integrated into the visit, and treatment modalities leading to a shift from a diseased to a healthy oral environment recommended.
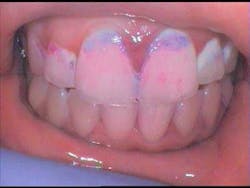
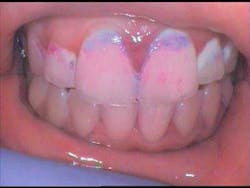
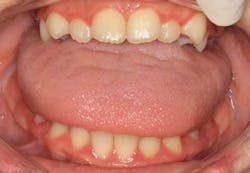
A plaque-free score can be used to determine the location, number, and percentage of biofilm-free surfaces.(1) This score can provide information regarding how effective a patient’s home-care techniques are. A plaque index will allow the clinician to assess the thickness of the biofilm at the gingival area. (1) Both of these exams can be performed by using a disclosing agent. Use of a disclosing agent provides a visual tool that allows the clinician to determine the areas being missed by the patient and also serves as an effective enhancement to the educational process. The GC Tri Plaque ID Gel is a useful product that can aid in identifying new, old, and extra-high caries risk plaque. The gel is smeared on the tooth surfaces and after application, the patient is asked to lightly rinse the mouth with water. A pink or red color on the tooth surface indicates new plaque. A blue or purple color indicates mature plaque that has been on the tooth surface for at least 48 hours, while a light blue color is indicative of mature and strong, acid-producing plaque.
Patients presenting with light plaque can be cleared for orthodontic care; however, those with poor oral hygiene practices should be placed on a preventive regimen that will aid in the control of biofilm formation. An adjunct supplement to brushing and flossing would be in the integration of products containing xylitol as the sole or principal sweetener. Streptococcus mutans is one of the early colonizers on the tooth surface and produces a sticky, extracellular polysaccharide that enables more fastidious organisms to attach to the tooth. Xylitol inhibits adhesion of these bacteria by decreasing the gtfB gene expression of S. mutans, which can negatively affect the synthesis of extracellular polysaccharides. (2) This inhibition contributes to a reduction in biofilm formation by weakening the adherence potential.
Xylitol can be easily implemented throughout the course of the day. Research shows the effects plateau between 6.4 grams and 10.3 grams per day, so patients should be placed on a regimen within this range. (3) Moreover, frequency of xylitol is just as important as prescribing a proper therapeutic dose. Dosing of less than three times a day has shown to have small, nonstatistical difference in S. mutans levels. (4) Because mouth pH drops after the intake of meals and snacks, it would benefit potential orthodontic patients to routinely use xylitol after every meal. This will help to balance oral pH and will contribute to a healthier oral environment. (5)
While brushing and flossing are instrumental to plaque removal, placing patients on a regimen of gums and candies containing xylitol can simplify this process by inhibiting the adherence of plaque. Furthermore, because xylitol comes in a variety of forms, it can lead to greater compliance. Adolescent patients will be more excited about implementing a regimen that includes chewing gum, flavorful candy, or water sweetened with xylitol. This compliance will lead to a shift in disease status and will ensure oral health throughout the course of orthodontic care.
ADDITIONAL READING ...
Why won't my patient ... Getting even your toughest patients to better oral health
The role of the dental hygienist in orthodontics
References
1. Wilkins, Esther M. Clinical Practice of the Dental Hygienist. Lippincott Williams & Wilkins, Philadelphia, PA. 2012.
2. Peldyak J, Makinen, Kauko K. Xylitol for Caries Prevention. Journal of Dental Hygiene, 2002; 76(4):276-285.
3. Milgrom P, Ly KA, Roberts MC, et al. Mutans streptococci dose response to xylitol chewing gum. Journal of Dental Research, 2006; 85:177-181.
4. Ly KA, Migrom P, Roberts MC, et al. Linear response of mutans streptococci to increasing frequency of xylitol chewing gum use: a randomized controlled trial [ISRCTN43479664]. BMC Oral Health, 2006; 6:6.
5. Topitsoglou V, Birkhed D, Larsson L, Frostell G. Effect of chewing gums containing xylitol, sorbitol or a mixture of xylitol and sorbitol on plaque formation, pH changes and acid production in human dental plaque. Caries Res, 1983; 17:369-378.