The pathology with multiple manifestations
Editor's note: Originally published October 18, 2019. Formatting updated November 15, 2022.
Case presentation
A 75-year-old female presents to the office for a recare exam with a chief complaint of painful/burning lesions in her mouth that had been there for two weeks. She additionally reported that her body and arms had numerous “bumps” that manifested over the course of the last six weeks, and she was wondering if there was any relationship between the two.
Patient history
The patient had been seen recently by her primary care physician (PCP) for the lesions on her body and arms as well as for other symptoms that included fatigue, joint pain, and tenderness. Her PCP ordered blood tests to be taken over a six-week interval and then another office visit to discuss a definitive diagnosis.
In the interim, the patient was placed on methotrexate. She mentioned that her mouth had seemed drier over the last few weeks, but she didn’t think much of it until the oral lesions appeared about two weeks ago. She elaborated and said that initially, the gums/tissues in her mouth were all red and then eventually changed over to painful white patches.
Clinical exam
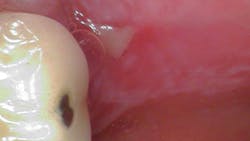
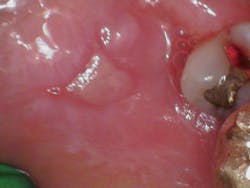
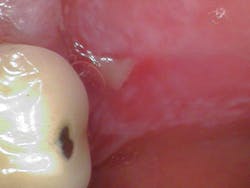
Clinical assessment revealed generalized ulcerated lesions intraorally, primarily focused on the buccal mucosa (figures 1 and 2). Furthermore, the tongue was coated with a white plaque-like layer.
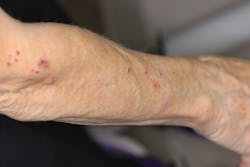
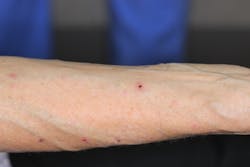
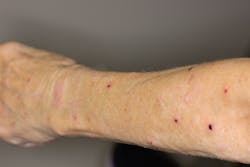
Presentation of the lesions on the patient’s arms showed numerous purplish flat-topped bumps, which had been scarred over somewhat as a result of her scratching them regularly. Overall, however, the lesions looked like they were on the mend (figures 3–5).
Once again, we are presented with ulcerlike and leukoplakic lesions intraorally. However, the added twist of the arm lesions in tandem can render the scenario somewhat challenging, if indeed a relationship between the two exists. The patient had already been to her PCP and a definitive diagnosis was pending, but the addition of methotrexate to her medicinal armamentarium and subsequent healing of the lesions allows the differentials to be narrowed down to some degree.
What do we know about methotrexate? It belongs to the antimetabolite class of drugs and is used primarily for cancer, severe psoriasis, and rheumatoid arthritis.1 This very strong medication is used to suppress the immune system and the progression of cancer cells.1
Differentials
- Lichen planus
- Aphthous ulcers
- Psoriatic osteoarthritis
- Leukemia
Definitive diagnosis: Lichen planus with psoriatic osteoarthritis
Treatment and discussion
Lichen planus lesions affect the skin and oral mucosa, with their etiology thought to be caused by genetics and/or autoimmune disorders.2 The lesions take on several different forms/patterns, including reticular (weblike), erosive, and eventually, ulcerative. They are found on the cheeks, tongue, and gums, and they can be quite painful when eating and drinking.2,3 There is no cure, but the condition can be managed with diet, topical medications, corticosteroids, etc.2
In this particular case, the lesions had taken on an ulcerative form and, at first assessment, appeared like canker sores or aphthous ulcers. As the patient’s care continued over time (as she was seen for follow-up appointments), the lesions converted to the nonpainful reticular form. The patient reports flare-ups now and then, which are dependent on stress levels and the overall state of her body.
With regard to the diagnosis of psoriatic osteoarthritis, it is an autoimmune disease that affects the joints as well as the tissues/skin of the body, as evidenced with our patient. Treatment is palliative and managed with injections of steroids, oral medications (methotrexate in severe forms), and alternative natural approaches.
Given the nature of the patient’s lesions with regard to location and timing, the relationship between the oral lesions and the arm lesions is indeed likely.
Subsequent treatment modalities for both types of lesions have rendered the patient stable under the care of her PCP. She has been weaned off the methotrexate and is now managing her symptoms with anti-inflammatories, diet, and steroid injections as needed.
References
- Methotrexate (anti-rheumatic) tablet. WebMD website. https://www.webmd.com/drugs/2/drug-3441/methotrexate-anti-rheumatic-oral/details. Accessed September 4, 2019.
- Burkhart N, American Academy of Oral Medicine Web Writing Group. Oral lichen planus. American Academy of Oral Medicine website. https://www.aaom.com/oral-lichen-planus. Updated September 2013. Accessed September 11, 2019.
- Wood NK, Goaz PW. Differential Diagnosis of Oral and Maxillofacial Lesions. 5th ed. St. Louis, MO: Mosby; 1997:75-77, 106-110.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].