The glass ionomer crown: A case report
Our practices serve a diverse population. We have patients who accept ideal treatment without any concern for finances or treatment time. On the other hand, we also have patients who cannot afford ideal treatment and patients who have medical conditions that preclude them from sitting (or sitting still) through lengthy dental appointments.
Glass ionomer technology has been flooding the marketplace. Although physical properties limit the use of most glass ionomers, there is a glass-hybrid restorative material on the market that is indicated for load-bearing Class II restorations. EQUIA Forte (GC America) is indicated for Class I, load-bearing Class II, and Class V restorations. We have been using EQUIA Forte and its older formulations for years with exceptional clinical success.
The reasons to consider glass ionomers for long-term restorations are plentiful, including excellent bond strength to dentin, excellent marginal integrity, good wear resistance, fewer caries, resistance to wear in acidic environments, ease of use, easily repairable, and efficient placement.
Case report
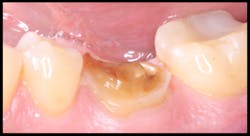
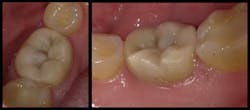
This is a case report of a tooth that was previously restored using a direct technique and a glass ionomer restoration. When the restoration failed, it completely debonded from the tooth surface, and minimal tooth structure remained (figures 1 and 2). When treatment options were discussed with the patient, he refused all traditional restorative therapies. In fact, he refused any preparation of his remaining tooth structure and requested that the tooth be restored with a direct glass ionomer restoration.
Figure 1: Lateral view at initial presentation
Figure 2: Occlusal view at initial presentation
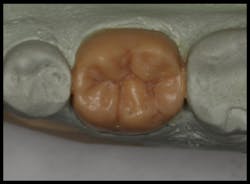
Given how difficult the handling properties of many glass ionomers can be, there are many challenges to restoring proper contour and function. We decided that another solution was necessary. A direct restoration using a glass hybrid restorative material in a guided matrix was used. A diagnostic wax-up was completed (figure 3).
Figure 3: A diagnostic wax-up was completed.
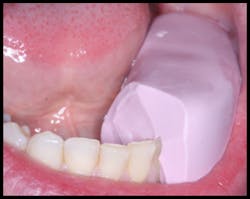
No local anesthetic was administered. Teflon tape was placed onto the adjacent teeth to separate the adjacent teeth and the restoration to create a restoration with interproximal contacts that could be flossed (figure 4).
Figure 4: Teflon tape was placed on the adjacent teeth to create interproximal contacts that could be flossed.
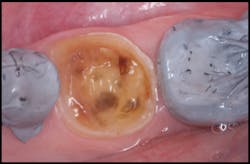
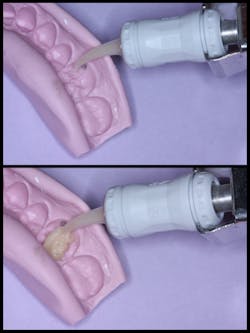
The tooth surface was conditioned with a polyacrylic acid conditioner (Cavity Conditioner, GC America). EQUIA (GC America) was triturated, per the manufacturer's recommendations, and placed into the silicone matrix (figure 5). The silicone matrix was placed intraorally (figure 6), and the material was allowed to set. The silicone matrix was removed (figure 7).
Figure 5: EQUIA was placed in the silicone matrix.
Figure 6: The silicone matrix was then seated onto the tooth.
Figure 7: The silicone matrix was removed immediately after polymerization.
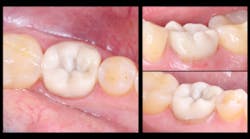
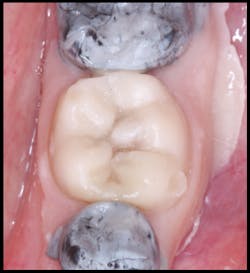
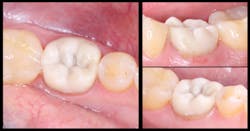
All excess material was removed, and occlusion was checked. The restoration was coated with EQUIA Coat and then light cured. The final result had ideal contours and occlusion (figure 8). At a 23-month recall visit, the tooth was still in occlusion, and minimal wear was noted (figures 9 and 10).
Figure 8: The final result
Figure 9: The final restoration at a 23-month recall visit
Figure 10: No. 19, still in occlusion at a 23-month recall visit
In cases when ideal treatment is not possible, or in instances when a patient requests glass hybrid restoratives for definitive treatment, this may be a viable treatment consideration. Should this restoration chip, fracture, or debond completely, glass hybrid restoratives can be easily repaired or replaced. Although this technique demonstrates use of the material beyond the recommendations of the manufacturer, we believe that this technique should be considered as a legitimate long-term treatment option.
Since this restoration was placed, a newer glass hybrid restorative with even greater physical properties, EQUIA Forte, became available. We are confident that this technique is an ideal technique when minimally invasive therapies are indicated.
Pamela Maragliano-Muniz, DMD, is an editorial director for Pearls for Your Practice: The Product Navigator, an e-newsletter from DentistryIQ and Dental Economics. She was a dental hygienist before earning her DMD from Tufts University School of Dental Medicine and her certificate in advanced prosthodontics from the UCLA School of Dentistry. She teaches, and she maintains a private practice in Salem, Massachusetts. In 2010 her practice was named the Adult Preventive Care Practice of the Year by the American Dental Association.
Brian Nový, DDS, is the director of practice improvement at the DentaQuest Institute and an adjunct associate professor in the division of general dentistry at Loma Linda University. He served on the ADA Council of Scientific Affairs from 2010–2014 and as chair of the CAMBRA Coalition from 2010–2015. In 2009 Dr. Nový's office was named the Adult Preventive Care Practice of the Year by the American Dental Association. He practices in Westborough, Massachusetts, at the DentaQuest Oral Health Center.