Pinhole Surgical Technique: Impressive clinical results and greater patient acceptance in tissue grafting cases
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.
A few years ago I met a patient with advanced gingival recession, inadequate attached gingiva, and severe mucogingival defects in all four quadrants, for which I recommended four rounds of connective tissue grafting spanning a minimum of one year. Once I explained that, due to the need for connective tissue grafting on all four first molars and canines, he would require a minimum of four independent surgical procedures to correct the problem, he was understandably less than enthused. When he asked why it would take so long, I explained that because the defects were separated by a premolar in each quadrant and it was not possible to obtain a single palatal graft that could span this distance, he would need two palatal grafts for each quadrant to be treated (particularly because he was also missing his maxillary bicuspids, limiting the space he had available from which to harvest tissue). Furthermore, the palate would require a minimum of three months to regenerate the harvested tissue so that it could be harvested again. Like many patients, he said he would “think about it,” which I think we all know probably means thanks but no thanks, andreturned to his general dentist for maintenance.
It wasn’t until last fall that I heard from him again. I had just become certified to perform the Pinhole Surgical Technique and sent a letter to all of my referring doctors to notify them of this new service I was offering for my patients. I admit I did not recognize his name on the schedule when I saw him again for a consultation. Apparently his dentist was concerned about his recession after watching it progress little by little, year after year, and suggested he talk to me to see if he was a candidate.
ADDITIONAL READING |Periodontally accelerated osteogenic orthodontics reduces treatment times in comprehensive orthodontic cases
I reviewed his medical history and performed a comprehensive examination to make sure he did not have any contraindications to treatment such as uncontrolled diabetes, active periodontal disease, or extensive bone loss. Luckily, my only findings included recession and inadequate attached tissue resulting in mucogingival defects, occlusal trauma from bruxism, and recurrent decay on some of his failing Class V restorations. He was a perfect candidate for the Pinhole technique!
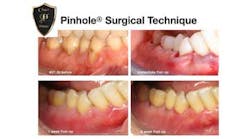
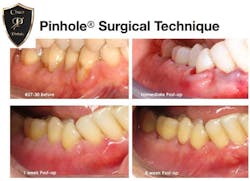
Still hesitant due to his fear of “surgery,” he opted to proceed with the treatment of only one quadrant. His existing Class V restorations were removed, decay eliminated, and gingiva coronally advanced using the Pinhole procedure. During his postoperative visit 48 hours later, he was pleasantly surprised at the absence of pain and immediate results. Thankfully he remained compliant with our instructions not to brush or floss the area during the healing period. And he is so happy with the results that he has already scheduled treatment for both the upper and lower left quadrants later this year, despite having no remaining insurance benefits.
ADDITIONAL READING | Nonsurgical periodontal disease treatment: The periodontist's point of view
This story is just one of many patients who have refrained from proceeding with connective tissue grafting—no matter how severe their periodontal condition—due to their fear of “surgery,” palatal harvesting, and stitches (evidently sutures are a very real fear of many people even if the sutures are dissolvable!). This case demonstrates some of the major patient-perceived benefits of the PinholeSurgical Technique: minimally invasive, suture free, graft free, and scalpel free. Of course not all patients are candidates. Like conventional therapies, they must be free of active disease, have no extensive bone loss, and be healthy enough for treatment, to name a few limitations. However, unlike traditional connective tissue grafting, there is no limitation to how many areas can be treated at the same time, and there is much higher patient acceptance due to some of the reasons stated previously. As the clinician, of course, I am pleased with the ease of the procedure and decreased chairtime to perform it, but most importantly the improved patient acceptance and impressive results I have seen in both my own patients as well as my respected colleagues nationwide who have been performing this procedure for a couple of years.
Adding the PinholeSurgical Technique to my clinical repertoire has allowed me to help more patients than ever before who would rather let their teeth fall out than proceed with alternative treatments. You think it’s difficult to convince a patient to do a crown or root canal because it “doesn’t hurt”?! Try explaining to someone why they should get surgery to correct a problem they think they’ve had since conception!
How is the Pinhole Surgical Technique performed?
A small pinhole is created by piercing the mucosa apical to the mucogingival junction in the area of recession, and specialized instruments are inserted through that hole to elevate a full thickness “flap” in an apico-coronal direction. Once the periosteum is elevated from the underlying bone and tooth, it can be easily pushed coronally. In lieu of stitches and soft-tissue grafts, collagen strips are inserted through the pinhole, under the gingiva, and into the interproximal spaces and facial surfaces of the previously exposed roots. Violà! The tissue is supported at the new position with the collagen assisting in tissue stabilization during healing to ensure root coverage.
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.