Trauma and horizontal root fractures of the anterior teeth: A review and case report
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.
Horizontal root fractures present an interesting diagnostic and treatment challenge for the endodontist. These types of fractures comprise only 3% of all dental injuries (1) and are at times difficult to diagnose. The diagnosis of horizontal root fractures rely heavily on radiographs, often times more than one, as the angulation of the X-ray beam needs to pass through the fracture line for them to be visible. It is also important to remember that these fractures often occur in an oblique fashion.
ALSO BY DR. JOSEPH PETRINO |Endodontic diagnosis: How lesions can cloud determination of root canal treatment
Surprisingly, the treatment of these injuries is relatively simple, as most often these teeth do not require endodontic treatment. Flexible splinting is required (or no splinting if the coronal segment is stable) for approximately two to four weeks and possibly longer if the fracture line is closer to the coronal third of the root (2,3,4). Following splinting, these teeth should be evaluated clinically and radiographically at three, six, and 12 months, and yearly after that for five years (4). Surprisingly, a vast majority of these cases do not require treatment. In fact, one study found that healing was noted in 84% of cases (5). In a classic study, Andreasen and Hjorting-Hansen noted four types of healing in 50 teeth that sustained horizontal root fractures, and only one was associated with pathology (6).
Case report
The following case depicts healing associated with an immature central incisor that sustained a horizontal root fracture.
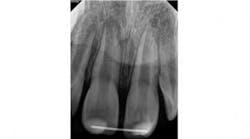
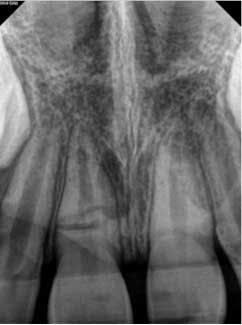
A 7-year-old male presented to my office following an accident that resulted in a horizontal root fracture of tooth No. 8. Upon examination, the general dentist had splinted the central incisors together using a rigid splint. Clinical testing on tooth No. 8 revealed that this tooth had a nonlingering response to cold and displayed slight tenderness to palpation. All other testing on teeth Nos. 7 and 9 was within normal limits (WNL). Radiographically, the apices of both central incisors were incompletely developed and a horizontal root fracture was noted at the junction of the coronal and middle third of the root on tooth No. 8 (figure 1). Due to the positive response to cold and lack of symptoms to percussion, bite, and palpation, I recommended retesting in three weeks and removal of the splint.
Approximately three weeks later, the patient returned and the splint was removed. Upon removal of the splint, slight mobility was noted on tooth No. 8. Vitality testing was again performed at this visit, which was equivalent to the initial visit.
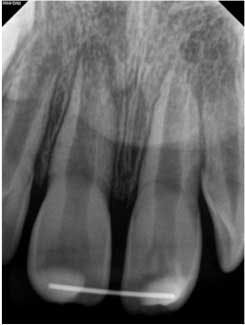
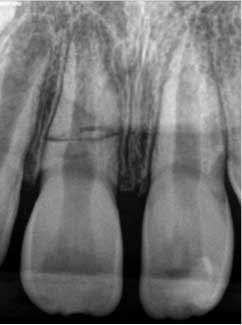
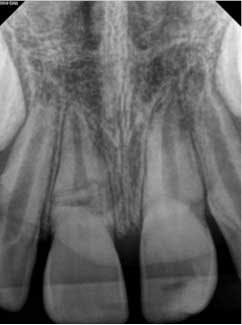
At three months, the clinical testing was equivalent and radiographs showed a fracture still present, but the periodontal ligament (PDL) and lamina dura (LD) were intact and uniform, especially near the fracture line (figure 2). At six months, there was no change in the response to vitality testing and radiographs continued to show no deleterious changes (figure 3).
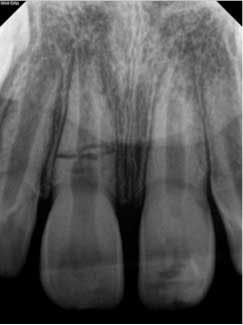
At approximately one year, the patient returned for follow-up. Clinical testing was equivalent to earlier recall visits. Radiographically, the tooth showed continued apical development with further development of a calcific barrier at the fracture line (figure 4). Furthermore, the medial aspect of the fractures showed repair.
At approximately two years, the patient returned for follow-up. Clinical testing was again equivalent to previous visits despite calcific metamorphosis of the coronal portion, which can occur following trauma (1). The mesial aspect of the fracture shows repair and continued apical development is noted on tooth No. 8 (figure 5). Even at each visit, I have informed the patient and his parents that treatment may be needed, but I am starting to feel more and more confident that this tooth will continue to repair itself without any intervention as the prognosis for this tooth is favorable.
There are a few factors that can impact the prognosis for teeth with horizontal fractures. Teeth with the fracture at the coronal crest have a poor prognosis and the coronal segment requires extraction. The more immature a tooth is, the prognosis is better; however, immature teeth rarely sustain these fractures (7). Complications of these injuries include development of necrosis in the coronal segment, which occurs in approximately 20% of cases and can be treated endodontically (1). The apical segment rarely undergoes pulpal necrosis. Development of radiolucencies along the fracture line is an indicator of pulpal necrosis. Lastly, the prognosis is better following good reduction of the fracture and semi-rigid splinting (8).
It is important to remember that not all teeth that sustain trauma will require treatment. Like any case, diagnostic testing is crucial to assess if there is a need for treatment. Additionally, remember that there are valuable resources to help decision making when it comes to trauma, including http://www.dentaltraumaguide.org and the trauma resources section on the AAE website.
As stated earlier, this case presented an interesting challenge as seeing a fractured tooth makes one feel that treatment is going to be needed or should be initiated. However, if testing indicates vital pulp tissue, minimal or no intervention can be the best course of action for the patient.
Acknowledgements
The author would like to thank Drs. Scott B. McClanahan, Jeff Wiswall, and Kendra Boda for their help in reviewing this manuscript.
This article first appeared in the newsletter, DE's Breakthrough Clinical with Stacey Simmons, DDS. Subscribe here.
ALSO BY DR. JOSEPH PETRINO |Regenerative endodontics
References
1. Zachrisson BU, Jacobsen I. Long -term prognosis of 66 permanent anterior teeth with root fracture. Scan J Dent Res. 1975;83:345‑354.
2. Andreasen JO, Ahrensburg SS, Tsilingaridis G. Root fractures: the influence of type of healing and location of fracture on tooth survival rates—an analysis of 492 cases. Dent Traumatol. 2012;28:404-409.
3. Cvek M, Tsilingaridis G, Andreasen JO. Survival of 534 incisors after intra-alveolar root fracture in patients aged 7-17 years. Dent Traumatol. 2008;24:379-387.
4. The Treatment of Dental Traumatic Injuries. Endodontics: Colleagues for Excellence. Summer 2014.
5. Cvek M, Mejare I, Andreasen JO. Healing and prognosis of teeth with intra-alveolar fractures involving the cervical part of the root. Dent Traumatol. 2002;18:57-65.
6. Andreasen JO, Hjorting-Hansen E. Intraalveolar root fractures: radiographic and histologic study of 50 cases. J Oral Surg. 1967;25:414-426.
7. Andreasen JO, Andreasen FM, Mejare I, Cvek M. Healing of 400 intra-alveolar root fractures. 1. Effect of pre-injury and injury factors such as sex, age, stage of root development, fracture type, location of fracture, and severity of dislocation. Dent Traumatol. 2004;20:192-202.
8. Andreasen JO, Andreasen FM, Mejare I, Cvek M. Healing of 400 intra-alveolar root fractures. 2. Effect of treatment factors such as treatment delay, repositioning, splinting type and period and antibiotics. Dent Traumatol. 2004;20:203-211.