The strange things you see in dental sleep medicine
DENTAL SLEEP MEDICINE (DSM), commonly referred to as oral appliance therapy for obstructive sleep apnea (OSA) and snoring, intersects medicine and dentistry, and the unique nature of every patient means that dentists who practice in this field need to be prepared for anything.
For example, one of my patients had a custom appliance that he had used for years. When it needed to be replaced, he decided to purchase an appliance from the internet and modify it. He then came to me and asked if I could make him something like what he had created.
The patient had added a baby bottle nipple to the online appliance as a tongue stabilizing device. Because the nipple had a hole in the tip, he superglued a pushpin in the end of the nipple with the sharp point of the pin stuck through the nipple next to his tongue (he said that it never poked him). He had also placed a rubber band at the back of the appliance to help keep his tongue forward. The rubber band was not attached to anything and could very easily fall off into the back of his throat and potentially be aspirated.
I told the patient that I could not create an appliance like this, but I would really like to take a picture of his “interesting handiwork.” He was very reluctant and said, “Well, I do not want you copying my design idea.” I reassured him that he did not need to be the least bit concerned about that!
He wasn’t the only patient whose decision-making processes may have been impacted by OSA. One of my colleagues, Trish Braga, DDS, had a patient whose oral appliance had exceeded its useful lifetime, and the patient came to her asking for a replacement. He reported poor compliance with his continuous positive airway pressure (CPAP) machine due to claustrophobia, and he described removing his CPAP mask unconsciously and consistently during the night over a six-month trial period.
His former DSM provider (a dentist) had made a device for him that allowed him to open his mouth while it was in place (probably due to his self-proclaimed claustrophobia). Paradoxically, the patient also explained that his device worked much better with his mouth closed, and so he routinely used his wife’s pantyhose, tied around his chin and the top of his head, to keep his mouth from dropping open at night!
Significant training and experience can prepare dentists to handle unusual cases such as these, but it can also help them solve common patient problems.
Thomas Schell, DMD, an experienced DSM practitioner who recently co-chaired an international consensus conference on side effects and helped author a how-to guide for the most common side effects and their resolution, uses his experience to close gaps between teeth.
“One of the side effects I have been able to correct is the opening of contacts between the lower first and second molars. This open contact leads to food impaction, and subsequently either tooth decay and/or periodontal disease (or both). This is a relatively common side effect and one that can be easily treated with the following technique.
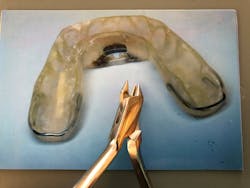
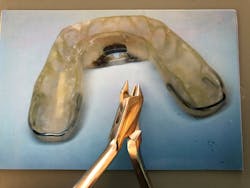
“With an impression of the lower arch, a wire cured into the plastic of the appliance, wrapping the back side (distal) of the tooth with the open contact, a small dimple can be bent into the wire with a three-prong plier (figure 1) in subsequent visits, moving the tooth gradually forward until the contact is closed. This wire will help to keep the contact from reopening and can also aid in added retention of the device.”
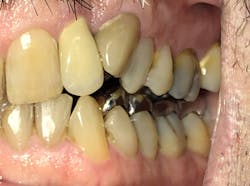
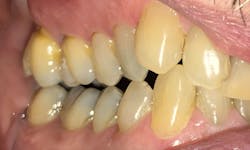
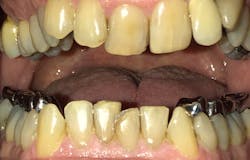
The understanding of how to treat obstructive sleep apnea has advanced rapidly in recent years. Michelle Cantwell, DMD, recently saw a patient with an oral appliance that needed replacement (figures 2–5).
“One of my colleagues used to make his own appliances using thermoplastic material and orthodontic components. He had a strong understanding of engineering and was working in uncharted territory at the time. The appliances were functional but could cause a significant amount of tooth movement (if patients failed to return for any follow-up).
“When one of his patients came to me recently, I braced myself for the discussion about how to correct the malocclusion, considering that bilaterally there was no posterior contact as well as an unesthetic anterior alignment.
“Instead, the patient said they were only there to have the removable cast-metal occlusal plate modified. The patient was the longest living person of their gender in their family, and the patient attributed that to having managed their obstructive sleep apnea.”
One way for dentists to learn the state-of the-art in DSM is to attend an intensive training program like the American Academy of Dental Sleep Medicine (AADSM) Mastery Program, which provides 65 hours of continuing education. Upon completion, dentists are eligible to sit for the American Board of Dental Sleep Medicine (ABDSM) exam. Passing the exam confers diplomate status, which enhances the dentist’s credibility among physicians, insurance companies, and patients. You can learn more about the AADSM Mastery Program at aadsm.org/mastery.
Read more clinical dentistry articles at this link.
Editor's note: This article originally appeared in Breakthrough Clinical, a clinical specialties newsletter from Dental Economics and DentistryIQ.
About the Author

Nancy L. Addy, DDS
Nancy L. Addy, DDS, is president of the American Academy of Dental Sleep Medicine. Since 1999, she has treated patients with obstructive sleep apnea while being an active AADSM member. She became a diplomate of the American Board of Dental Sleep Medicine in 2006 and served as the ABDSM president from 2014 through 2016. After concentrating her practice exclusively on dental sleep medicine in 2006, she earned AADSM facility accreditation in 2012. Dr. Addy regularly lectures on oral appliance therapy both locally and nationally, and she currently serves on the Peer Review Board of the Kansas Dental Association. She is a graduate of the University of Missouri-Kansas City School of Dentistry and a former assistant professor of general dentistry at UMKC.