Guidelines for peri-implantitis and antibiotic premedication
Guidelines for treating peri-implantitis
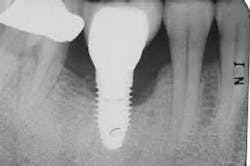
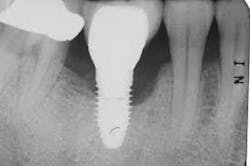
Peri-implantitis, including peri-implant mucositis and peri-implantitis, is a common cause for the failure of dental implants. Failure can be initiated by inappropriate treatment planning, surgical or mechanical failure, or poor maintenance.(1) Risk factors are many, and include poor biofilm plaque control and/or the inability of a person to cleanse the area adequately. There are many different treatments for managing peri-implantitis.
Searches were conducted in PubMed, Embase and the Cochrane Central Register of Controlled Trials (CENTRAL) databases. This was supplemented by searches in relevant dental journals. Peri-implantitis was defined as the presence of inflammation of the mucosa and loss of supporting bone around an implant in function. The primary outcomes were clinical attachment level gain (CAL) and the reduction in probing depth (PD). A meta-analysis for the efficacy of Er:YAG laser did not reveal statistically significant evidence for treatment effects in reducing PD and CAL levels in comparison to controls. The authors concluded, based on the information to date, that no advantage of laser treatment in comparison to conventional treatment of peri-implantitis could be identified.(2)
A Cochrane Systematic Review aimed to identify the most effective interventions for treating peri-implantitis.(3) They concluded that there is no consistent evidence that any one treatment modality is superior to another, however, that does not mean that any of the treatments are ineffective. Another 2014 Systematic Review did not offer any specific recommendations; they did report some successful outcomes.(4) Problems with recommendations include a variety of definitions being used in the studies, varying disease severity, different lengths of time for follow-up, and differing inclusion/exclusion criteria.
The guideline also includes a shared decision-making tool to facilitate cooperative decision-making between patient and clinician, and to supplement but not replace informed consent procedures. There is a guest commentary on the report that stresses the use of the science, the clinician, and the patient’s wishes. It also suggests collaboration between the medical and dental disciplines.(6) For information on all antibiotic premedication, visit the ADA website.(7)
Maria Perno Goldie, RDH, MS, is the editorial director of RDH eVillage FOCUS.
References
1. American Academy of Periodontology. Academy Report. Peri-Implant Mucositis and Peri-Implantitis: A Current Understanding of Their Diagnoses and Clinical Implications. Journal of Periodontology, Volume 84, Number 4, 436-443. http://www.joponline.org/doi/pdf/10.1902/jop.2013.134001.
2. Kotsakis GA, Konstantinidis I, Karoussis IK, Ma X, Chu H. A Systematic Review and Meta-Analysis of the Effect of Various Laser Wavelengths in the Treatment of Peri-Implantitis. J Periodontol. 2014 Jan 20. [Epub ahead of print] PubMed PMID: 24444398.
3. Esposito M, Grusovin MG, Worthington HV. Treatment of peri-implantitis: what interventions are effective? A Cochrane systematic review. Eur J Oral Implantol 2012; 5(Suppl): S21–S41.
4. Heitz-Mayfield LJA, Mombelli A. The Therapy of Peri-implantitis: A Systematic Review. The International Journal of Oral & Maxillofacial Implants, Volume 29, Supplement, p 325-345. 2014.
5. AAOS and ADA. Prevention Of Orthopaedic Implant Infection In Patients Undergoing Dental Procedures Evidence-Based Guideline And Evidence Report. December 7, 2012. http://www.aaos.org/Research/guidelines/PUDP/PUDP_guideline.pdf.
6. Jevsevar DS, Abt E. Guest Commentary. The New AAOS-ADA Clinical Practice Guideline on Prevention of Orthopaedic Implant Infection in Patients Undergoing Dental Procedures. J Am Acad Orthop Surg 2013; 21:195-197.
7. http://www.ada.org/en/member-center/oral-health-topics/antibiotic-prophylaxis#endocarditis.