Respiratory PPE, dry mouth, and COVID-19: Why you need to know your own CAMBRA score
Epidemiologists study health risks and are experts in determining disease patterns in populations. These scientists study both infectious and non-infectious diseases from an historical perspective and then apply what they have learned to project future disease outbreaks.
So why even bring this up? Certainly, dental professionals are quite adept at recognizing oral disease risks, but in today’s convoluted COVID 19-world, how many dental professionals are focused on what is happening their own mouth?
Dry mouth is increasing among health-care providers
While no one will argue the importance of increased personal protective equipment (PPE) requirements, there are simply unexpected consequences that should not be ignored. Based on several recent studies, 53% of health-care professionals report dry mouth and 66% are reporting a sense of dehydration.1
What does all of this mean to those of us in the trenches? We’re providing oral care to others, while our risk for caries, erosion, and fungal infections has risen exponentially since March 2020.2-5 The substantial risk of dry mouth syndrome is now a documented condition resulting from multiple side effects of using respiratory PPE for protracted periods of time.1
Evaluating personal risk
When is the last time you looked at your personal risk for oral disease? If you don’t think you have the time, it is really easy to get preliminary baseline data. Armed with good data, it is easy to make a plan that will lesson your risk for spending time off from work as a patient in the dental chair and help keep your smile intact. The CAMBRA risk assessment protocol, an acronym for caries management by risk assessment, was first introduced into the academic community over a decade ago. Over time CAMBRA protocols have worked their way into clinical practice, and it is now the standard cariology assessment tool.6
There are two data points that come in handy in assessing personal risk. The first is getting a reliable salivary pH score. Salivary pH values below 6 are heading into a risky range, especially if one has exposed root structure. The second data point evaluates buffering capacity or the ability to neutralize an acidic environment. These two data points are not the same, but together provide a much more robust look at relative risk. It is entirely possible to have a neutral oral pH, but simply lack buffering capacity, which can be a reflection of either the quality or also the quantity of saliva.2,3,7
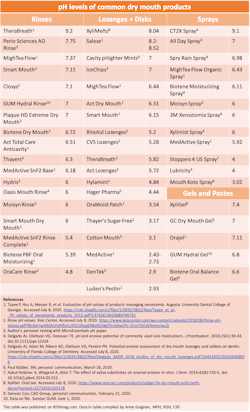
Micro Essential Laboratories is a reliable, established resource for all types of pH paper and testing supplies. Cavity pHighter test strips (CAO Group) are a new, innovative product that tests not only pH but buffering capacity. The testing is simple. Either place the strip in the mouth until fully moistened or coat the test strip reagent pads with a salivary sample. Immediately match the color change to the value grid on the product container.
In less than one minute, you now have data that you can use to create a solid action plan. The challenge then becomes a question of what next? Salivary stimulation, pH balancing, oral comfort, saliva composition support, or remineralization?8 Everyone has to determine their own personal strategy and figure out what product or protocol will work best in their lives. This is not a cookie-cutter solution.
Potentially dangerous consequences
The challenge of improving oral moisture or increasing hydration is complicated. Picking a safe strategy is a balancing act. Quite simply, a number of oral moisturizing rinses, gels, or lozenges are acidic, which adds fuel to the fire.9-11 While acidic preparations will stimulate saliva, if the oral cavity is dry, buffering is either compromised or nonexistent.2,3,7
There are many products that claim hydration properties. These come fully prepared or in powders or drops that are added water or other fluids.12-13 Most of these preparations are acidic in nature as well, and there are several ways to reverse the impact. Either drink the beverages quickly to reduce contact time, or consume them while eating protein, which has the potential to bind acids. Another strategy is to super-saturate a drink a fruit smoothie with a spoon or two of yogurt.14 This beneficial strategy counteracts the erosive potential due to the high level of calcium now available for remineralization.
Moving forward
In today’s world we simply need to recognize our personal disease risk, and figure out a way to implement strategies that help ward off health threats.
Receiving an academic dental degree, professional license, or becoming registered or certified to provide patient care is exciting. But quite simply, these achievements do not confer immunity to disease.
It is unlikely that any dental professional wants to be a statistic about the increased risk for oral disease created from wearing respiratory PPE while we care for other’s health needs.
- Guignon A. Impact of current PPE usage – healthcare professionals. June 2020.
- Leo M. Sreebny; Arjan Vissink Author. Dry mouth - The malevolent symptom: A Clinical Guide. Wiley, Balckwell. May 2010.
- Birgnajje WS, Taylor GW, Anderson PF, Shannon C. Dry mouth (Xerostomia): Diagnosis, causes, complications and treatment. Oral and general health-Exploring the connection. Research Review 2011.https:// / https://www.nedelta.com/SiteMedia/SiteResources/downloads/Forms%20for%20All/Dry_Mouth_Research.pdfDryMouthDentalProfessionals.pdf Accessed 7/8/2020.
- Lussi A, Schlueter N, Rakhmatullina E, Ganss C. Dental erosion--an overview with emphasis on chemical and histopathological aspects. Caries Res. 2011;45.
- Hara AT, Zero DT. The caries environment: saliva, pellicle, diet, and hard tissue ultrastructure. Dent Clin North Am. 2010 Jul;54(3):455-67.
- Fontana M, Zero DT. Assessing patients' caries risk. J Am Dent Assoc. 2006;137(9):1231-1239. doi:10.14219/jada.archive.2006.0380
- Buzalaf MA, Hannas AR, Kato MT. Saliva and dental erosion. J Appl Oral Sci. 2012;20(5):493-502. doi:10.1590/s1678-77572012000500001
- Guignon A. Treating dry mouth. What’s the point? RDH. 2018. https://www.rdhmag.com/patient-care/article/16408127/treating-dry-mouth-whats-the-point. Accessed July 8, 2020
- Delgado AJ, Olafsson VG, Donovan TE. pH and erosive potential of commonly used oral moisturizers. J Prosthodont. 2016 Jan;25(1):39-43.
- Delgado AJ, Olafsson VG. Acidic oral moisturizers with pH below 6.7 may be harmful to teeth depending on formulation: a short report. Clin Cosmet Investig Dent. 2017;9:81‐83. Published 2017 Aug 3. doi:10.2147/CCIDE.S140254
- Tayee P, Hsu A, Messer R, De Rossi S, Ciarrocca K, DeStefano J, Rueggeberg F. Evaluation fo pH valies of products managing xerostomia. Dept. Oral Biology, Augusta University, Augusta, GA. 2015. https://cdn.shopify.com/s/files/1/0035/3832/files/Tayee_et_al-_Ph_values_of_xerostomia_products_2015.pdf?13742613603684799761. Accessed July 8, 2020.
- West NX, Hughes JA, Addy M. The effect of pH on the erosion of dentine and enamel by dietary acids in vitro. J Oral Rehabil. 2001;28(9):860-864. doi:10.1046/j.1365-2842.2001.00778.x
- Nguyen Ngoc C, Ghuman T, Ahmed SN, Donovan TE. The erosive potential of additive artificial flavoring in bottled water. Gen Dent. 2018 Sep-Oct;66(5):46-51.
- Blacker SM, Chadwick RG. An in vitro investigation of the erosive potential of smoothies. Br Dent J. 2013 Feb;214(4):E9.
ANNE NUGENT GUIGNON, MPH, RDH, CSP, a visionary thinker, has received numerous accolades over four decades for mentoring, research, and guiding her profession. As an international speaker and prolific author, Anne focuses is on the oral microbiome, erosion, hypersensitivity, salivary dysfunction, ergonomics, and employee law issues. She may be contacted at [email protected].
About the Author

Anne Nugent Guignon, MPH, RDH, CSP
ANNE NUGENT GUIGNON, MPH, RDH, CSP, a visionary thinker, has received numerous accolades over four decades for mentoring, research, and guiding her profession. As an international speaker and prolific author, Anne focuses is on the oral microbiome, erosion, hypersensitivity, salivary dysfunction, ergonomics, and employee law issues. She may be contacted at [email protected].
Updated June 26, 2020