Protecting your hands
by Mary Govoni, CDA, RDA, RDH, MBA
As a dentist, your hands are your livelihood. Protecting them means protecting your ability to continue earning your living in dentistry, not to mention the personal benefits of comfort and health. There are many factors to consider in protecting your hands, but the two key factors are protecting them from exposure to infectious diseases and preventing injury from repetitive tasks or cumulative trauma that can cause a musculoskeletal injury.
First, let’s consider infectious diseases. Hand washing and personal protective equipment are critical elements of an infection-control program, both from a regulatory standpoint (OSHA) and to ensure your health and safety. According to the Centers for Disease Control, hand washing is one of the most important infection-control protocols. In dental settings, hand washing should occur before donning and after removing gloves. In some cases, dental professionals perceive gloves as substitutes for hand washing, which puts them at risk if gloves develop micro tears. In this case, saliva and blood can come in contact with fingers and hands, posing the risk of infection. While OSHA and the CDC recommend antimicrobial hand-washing products, they are not mandated. Antimicrobial soaps contain compounds such as triclosan or chlorhexidine that decrease the number of microbes on the skin, beyond the physical action of washing the hands. In addition, these antimicrobial agents provide persistent activity, which helps control the regrowth of microbes on the skin.
For a dentist with sensitive skin, however, antimicrobial agents can be drying and irritating. Intact skin is an excellent barrier against infection, so it is more important to find a hand-wash product that does not irritate the skin than it is to ensure the use of a product with antimicrobial properties. This is especially important during cold weather, when skin tends to be extra dry and easily cracks and chaps. The CDC recommends the use of soap and water or alcohol-containing, waterless hand-wash products in health care settings. Either is acceptable for dentistry, but your specific needs determine which product is most appropriate.
In addition to hand washing, examination gloves are the other key infection prevention tool required in dental-practice settings. Selecting the right gloves is a matter of personal preference, as well as patient needs. Many dentists prefer latex gloves because they provide superior elasticity and flexibility.
Some patients, however, are allergic to latex, making it necessary for dentists to have nonlatex gloves available. Nonlatex gloves have improved in quality and flexibility over the years and many good nonlatex alternatives are readily available from dental distributors.
The fit of gloves is important not only for infection prevention, but for the musculoskeletal health of the hands. Wearing a glove that is too large can result in less dexterity, possibly leading to a puncture injury. Wearing a glove that is too small can result in tearing from fingernails or jewelry and pose an infection risk. It is important to note that the CDC recommends that natural nails be short, so as not to puncture gloves, and that artificial nails (acrylic, gel, or tips) are not recommended in clinical settings.
Another important factor to consider is that constant donning and removing of gloves promotes wear on the prongs of rings. Have jewelry checked by a jeweler regularly to avoid losing valuable stones from rings. Because fungal infections can occur on fingers underneath rings, it may be a good idea not to wear rings at work.
An improperly fitting glove can also cause pain and numbness in the hand, particularly at the base of the thumb. Wearing a glove that is too small or wearing ambidextrous gloves can cause compression of the hand in this area, resulting in discomfort. Changing to a larger glove size may help, or wearing hand-specific gloves may be necessary to relieve symptoms.
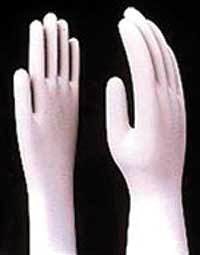
The top photo illustrates the difference between the hand forms that are used to manufacture ambidextrous and hand-specific gloves.
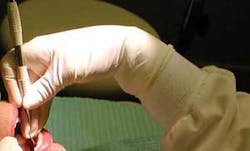
If glove size is not a factor in hand discomfort at work, several other factors should be considered. The first is hand position. Carpal tunnel syndrome is a common workplace injury, especially among women. It is a type of compression neuropathy that can result in numbness, tingling, weakness, and severe pain. At work, CTS can be caused by performing repetitive functions, especially those performed with the wrist in a bent position, compressing the median nerve in the hand, as shown in the photo.
Another contributor to hand discomfort is instrument selection and use. Instruments with small-diameter handles cause the user to use a tighter grip on the instruments. Tightly gripping an instrument causes muscle tension, pain, and stiffness. Using instruments with larger-diameter handles can decrease tension and loosen the grip. This applies to mirror handles as well. Holding a mirror in the nondominant hand with the wrist bent is a common practice for many clinicians. Instruments with soft silicone handles, grips, or both can also increase hand comfort. Lightweight, balanced handpieces are also critical to hand comfort.
These are a few important suggestions for protecting the health of your hands. Everything that you can do to prevent injury is a measure that helps safeguard your livelihood.