The debate over occlusion
Equipment and materials for occlusion-oriented dentists
For reasons that are not entirely clear, the subject of occlusion has become one of the most controversial subjects in all of dentistry. In fact, most dentists would agree that there are few areas in dentistry that inspire so much heated debate and disagreement as occlusion. Probably not since the Civil War has any group of people been so divided in opinion. Over the past several decades, most dental schools shied away from teaching occlusion to the undergraduates, blaming the already-crowded curriculum. Most dentists leaving dental school do not have even the most basic understanding of the fundamental concepts of oral biomechanics and muscle physiology. As a result, many estimate there are less than 20 percent of dentists actively treating bite problems in one way or another, while most of the rest of the profession seems to be standing on the sidelines thinking that if the experts cannot agree on what to do, then this issue is too controversial to touch. In the end, the real losers are our patients who unknowingly suffer from a reduced standard of care.
It’s all just physics
Whether it is an airline pilot about to thunder down the runway in a 747, an engineer designing a shopping mall, a carpenter building a new deck on a house, a truck driver approaching a rickety country bridge (right), or a dentist treating a patient, we all need to understand that, unless we are aware of and can control the adverse forces we might encounter, there can be disastrous consequences.
As dentists, we have all had exposure to science and physics courses. We have all read stories of airplanes that attempted to take off without realizing that there were significant crosswinds. We have read stories of engineers who designed structures in New England without taking into account the consequences of the additional weight of accumulating snow. Finally, we have all heard of little country bridges collapsing under the excessive weight of tractor-trailers. Yet, we are often surprised when a tooth gets loose or a filling breaks.
In medicine and sports, we understand that overstressing muscles by overexertion or prolonged activity will often lead to pain and breakdown. Athletic coaches design training programs based on muscle physiology. The occasional weekend jogger who suddenly decides to run in a 10K race is not surprised when he can barely get out of bed on Monday morning.
When an orthopedic surgeon inserts a prosthesis for the hip or knee, we expect he or she will take into account the magnitude and direction of force that the prosthesis is likely to encounter in daily function. Doesn’t it make sense that the muscles and jaw joints would be subjected to the same kinds of forces as the legs and/or arches of the feet?
The oral structures serve several purposes and among the most important are eating, chewing and swallowing. These functions create forces that need to be managed; if the forces exceed the system’s capacity or are improperly directed, the system will break down.
Top photo: Force is provided off axis, Bottom photo: Equal force is provided on axis.
Fundamentals
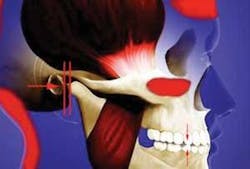
While the jaw joint is the most complicated joint in the human body and a major component of the “dental system,” most dentists have never studied and, therefore, do not appreciate its unique anatomy and physiology. It is interesting to note that when I was in dental school, we dissected the entire cadaver. However, we did not study the jaw joint, despite the fact that it is the foundation for everything we do in our entire career. There are three things that make the jaw joint unique:
* It is the only joint in the body where both the left and right sides have to move in coordination.
* It is the only joint in the body where the joint can move in three dimensions simultaneously. It can move forward and back, left and right, and can rotate open and closed.
* It is the only joint in the body that has an external articulating element - the teeth. In every other joint, the determinant of how the joint moves is in the muscles, ligaments, and bones of the joint itself. But with the jaw joint, since the teeth can only fit together in one way, in the final analysis, it is the teeth that determine the position of the jaw joints in the articular fossa.
Above: Teeth pull jaw joint off center.
Confusion or not, controversy or not, the fact of the matter is that the oral structures are affected by the same laws of physics as the rest of the universe. The human body, despite its ability to adapt and resist, is not capable of overcoming excessive force indefinitely.
You will probably never see a TV newsflash that says, “Mary Jones loses upper central incisor. While the details are as yet unclear, it appears that there were repeated collisions between teeth Nos. 8 and 25 and 26. The American Dental Association disaster recovery team has been on-site for several hours and has been investigating and interviewing witnesses. There are unsubstantiated rumors that Mary was doing some nighttime clenching. Her husband is reported to be in seclusion and was not available for comment, but there are as yet unconfirmed reports about some balancing side conflicts as well as a prior history of fremetice. Her dentist has not yet made a statement. We understand that the investigators have found the black box nighttime recorder and hope that, after they listen to it, that they will have more information. Please stand by as the story unfolds.” But you do probably see it nearly every day in your patient’s mouths.
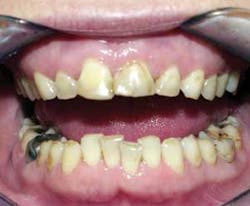
Above: Aftermath of an occlusal disaster.
Dentistry vs. internal medicine
Consider the field of cardiology. I am sure that at the American Association of Cardiology meeting there is considerable debate and disagreement as to the best methodologies to treat and prevent coronary artery disease. We know there are groups of doctors that feel that nutrition is a key factor, and some of them favor the low-fat approach, and others - as represented by the Atkins school - feel that carbohydrates are the killers and let their patients eat all the eggs and meat they want. We also know that there are doctors who believe that exercise is a key component, represented by people like Ken Cooper at the Cooper Clinic in Dallas. And there are schools of thought that believe that drugs are preeminent, such as those that lower cholesterol. Finally, there are those with a focus on early surgical intervention with the newest arthrography, stents, lasers, and laparoscopic robotic bypass procedures.
But at the end of the day, when the debates are over, they all walk out of the meeting rooms, face the public and regulatory authorities, and proclaim that despite their individual disagreements and preferences, they all agree that helping the heart to work best is what matters.
Unfortunately, in dentistry, it is not that way. We tend to focus much more on our areas of disagreement both internally (at meetings and conventions) as well as externally (to the public and regulatory authorities). This creates confusion in the eyes of both the public and the profession. There is no doubt that, in the long run, this is bad for everyone.
What am I going to do about it?
The key to improving the perception and practice of occlusion is simple - make it effective and predictable. In order to accomplish this, two things must be done. First, identify and highlight the fundamental occlusal concepts that experts of every major philosophy share. Where there are areas of significant disagreement, I will try to unemotionally show the options so that practitioners have the opportunity to see what works best in their hands and on their patients. Second, outline how to select and apply the plethora of materials and devices designed to improve, enhance, and simplify patient care.
In the area of occlusion, we have many types of equipment and materials at our disposal.
* Diagnostic imaging devices such as X-rays, CAT scans, and MRI scans.
* Listening devices such as stethoscopes, Doppler ultrasound, and Joint Vibration Analysis.
* Simulating devices such as articulators, face bows, and jaw tracking devices.
* Methodologies to assist us in determining how the teeth are hitting against each other, including marking ribbons, waxes, liquids, and the highly sophisticated T-Scan.
* Deprogrammers of all sorts of shapes and sizes that are prefabricated or custom-fabricated.
* Bite registration materials and techniques.
* Bite splints, hard and soft, anterior, posterior, and full coverage and many varieties of positioning devices.
* Patient education methodologies such as movies, flip charts, and models.
* Continuing-education programs.
And new things are coming on the market every month. The photo at the top of the next column shows some popular materials including a CAT-Scan, articulator (Panadent), facebow (Denar), full arch bite splint, anterior deprogrammer (Best-Bite), marking ribbon (Almore), bite registration media (Delar), sEMG system (BioResearch), and electronic occlusion contact and force measuring system (TekScan).
These devices, simple and complex, are not the ends in themselves; they are a means to an end. Most dentists are not super-interested in the chemistry of the newest bonding agents, but we are interested in using products that will give us good-looking, long-lasting, and sensitivity-free restorations. In the same way, we also want to create comfortable, long-lasting, and good-looking restorative cases as well. That is the purpose of the many devices and equipment we will explore in this column.
Tune in next issue for articulators
In the next column, we will examine articulators - big and small, complex and simple. What do they do? When do you use them? When may you not need them? What benefits can we derive from their use? What clinicians favor the different systems? Do you need one or several systems? How can you learn more about them? Where can you try them out and hold them in your hands, and see what might be best for your practice?
Summary
The purpose of this ongoing column is to create an environment of inclusion. Let’s see where we can agree and see what materials and equipment we can use to help our patients do better.
Author’s Note: I invite your questions, comments, and feedback via e-mail at [email protected] or call (212) 475-0393. I will personally respond to every e-mail as well as publish a response to the most frequent questions.
Dr. Jerry Simon has been an active dental practitioner in Stamford, Conn., for more than 30 years with a focus on bite dysfunctions. He is also the author of the book, “Stop Headaches Now: Take the Bite Out of Headaches,” more than 30 dental/medical journal articles, and inventor of the Best-Bite™ Discluder.