Integrating equipment
By Jain Malkin
Today's equipment choices give practitioners a myriad of options for success
Smile! The future has arrived and it is wonderful! This is a great time to be a dentist — and an even better time to be a patient. For dentists, selling esthetic or cosmetic cases has never been easier. Restorative dentists enabled by new software, digital cameras, and photo-quality ink-jet printers, can easily show patients what can be accomplished. For patients, especially image-conscious Baby Boomers, the lure of a great smile and sparkling white teeth is irresistible. DVD-format educational programming — such as the Smile Channel® by CAESY — used in the waiting room can stimulate a desire for cosmetic procedures. Demand for dental implants and periodontal procedures also is rising among Baby Boomers who want to live to 100 without dentures.
Designing the patient's experience
Recent census data confirm that the Baby Boomer generation will soon be the dominant segment of the population. Empowered by the Internet and confident about making healthcare decisions, this group of consumers has been characterized as finicky and discriminating, and willing to spend the time to evaluate a variety of goods and services before making a commitment. Marketing consultants tell us that a strategy for reaching this group is to create a memorable experience that engages customers in a personal way. In The Experience Economy, Pine and Gilmore suggest that staged experiences create lasting and memorable impressions that can bond customers — in this case, patients — to a specific provider.
We're all familiar with how Starbucks took a basic commodity (a cup of coffee) and presented it in an environment that elevates the experience in such a way that customers will pay considerably more for the product than they would at the corner diner. In a similar manner, dental treatment experiences can be designed and scripted to help differentiate a dentist from competitors and to ensure a level of customer service that exceeds expectations.
Dr. Kurt Schneider, a general dentist in Mission Viejo, Calif., has mastered this concept. He promises his patients a "pampered pleasant experience." The aroma of freshly baked bread greets patients who arrive at midday. Other refreshments include non-fat frozen yogurt, coffee, sodas, and juices. Patients in treatment rooms can choose entertainment or escape — listen to the news, watch a video movie, use virtual reality glasses to view a 3D movie, or wear stereo headphones to listen to music. Creature comforts include a blanket or heated neck support pillow filled with fragrant herbs, and patients are handed a hot lemon-scented facecloth to freshen up before leaving.
New technology optimizes efficiency
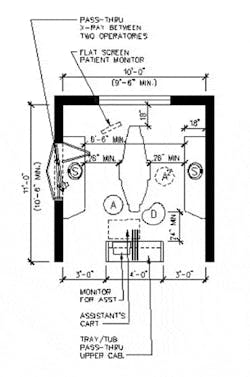
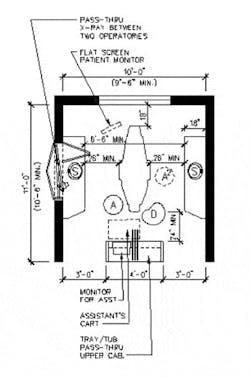
Recent advances in dental technology to enhance diagnostic capabilities and improve treatment are revolutionary compared to what was available only five years ago. It truly is a new world for dentists and, best of all, it's fun to use these new tools. Historically, dentistry has allowed for highly personalized practice methods, but this diversity will be minimized as technology is used to maximize efficiency and profitability. As a dental space planner, I have observed dentists cheerfully working in some of the most awkward spaces — Lilliputian operatories in which the dentist had to stand up to enable the assistant to leave the room. Some appear to be contortionists as they reach for or grab what they need. The willingness to adjust to an ergonomically unsuitable environment can take its toll in lost productivity, neck strain, and early retirement due to disability. Dentists who are starting out in practice or established dentists who are moving to a new location will have the best opportunities to accommodate new technology and to design — from scratch — a treatment room that optimizes efficiency (see left).
Plan the space before signing a lease
A common error, and one that can lead to 10 years of frustration, is leasing a space prior to engaging a space planner. While the dentist may know that he or she needs four treatment rooms in order to be functional, without a space plan it will be impossible to know how that space will lay out or if it will yield four treatment rooms of optimal size. A matter of inches can make a critical difference in an operatory. This is related to the shape of the space, the location of structural columns, as well as the overall dimensions of the area and perhaps the desire to have northern light in the treatment rooms. If the configuration of the space results in an awkward layout, undersized treatment rooms, and poor adjacencies with respect to critical functions such as sterilization and overall flow through the office, it may be desirable to find another location in that building or a different building.
As dentists know well, efficiency makes a tremendous difference, whether it is a convenient reaching distance while seated at the chair, the number of staff it takes to run the office, or the resulting stress that inefficiency places on the dentists and chairside assistants as they move through a busy schedule.
null
The regulatory climate heats up
Although there are variances among states, codes and regulations have been increasing dramatically for dentists. In terms of space planning, the Americans with Disabilities Act (ADA) means that dentists will no longer be able to pack a lot of stuff into small spaces. Tiny darkrooms, labs, or breakrooms with doors opening into the room, barely scraping the edge of the cabinet, are no longer possible. All rooms must be wheelchair-accessible and have an 18-inch wall area on the pull-side of the door. The ADA is interpreted differently by building departments even within the same region with respect to treatment rooms and task areas such as sterilization. Some require a 36-inch clearance on both the dentist's and the assistant's room entries, while others require the 36-inch opening only on the dentist's side.
Both OSHA and the Environmental Protection Agency (EPA) have regulations regarding the capture and certified disposal of film processing solutions or, at least, the fixer. Of course, the darkroom is quickly becoming extinct as digital imaging becomes widespread. The collection and disposal of amalgam and mercury is regulated at the state level.
Both OSHA and EPA have guidelines for hazardous waste and sharps, but there is a gap between what OSHA considers biohazardous (medical) waste within the working environment and what the EPA considers hazardous waste during disposal. It should be noted that national OSHA standards may be interpreted differently than state OSHA agencies. The OSHA/bloodborne pathogens standard mandates that universal precautions be taken with all patients.
An often overlooked design factor is the addition of a washer and dryer within the facility to launder barrier gowns. This also involves a storage area for clean gowns, which have either been laundered in the facility or sent out to a commercial laundry and subsequently delivered back to the dental office. A hamper is needed to collect soiled gowns until they can be laundered. The soiled clothing hamper or the washer and dryer cannot be placed in the staff lounge or any place food is prepared, or cosmetics or eye care products are used.
Dental equipment no longer uses city water because of possible contamination. Dental equipment is now designed to incorporate containers that can be filled with distilled water and mounted on the assistant's cart or on the dental console (see photos above). Other solutions include reverse-osmosis water or the use of an FDA-approved replacement solution that can be added to regular drinking water to kill microorganisms and prevent biofilm buildup in the water system.
Infection control
Clearly, sterilization techniques and infection-control procedures have changed dramatically in recent years. Instruments coming into contact with mucosal tissue during treatment must be processed, sterilized, and stored according to a higher standard of asepsis than has been common in the past. The Centers for Disease Control suggest that all dental instruments be wrapped or bagged prior to sterilization and remain sealed until used. Although the Dental Board in each state or the Board of Public Health regulate asepsis, the number of states where it is not mandatory that instruments be sterilized or packaged is dwindling as state regulators react to CDC guidelines by enacting legislation.
In addition, the ADA has endorsed the CDC regulations and made them the standard of care, which has led states to amend their practice acts accordingly. It is surprising how lax regulations have been with respect to sterilization of instruments and handpieces, and this is compounded by the fact that there is no agency inspecting dental offices in this regard.
The technology wave
The paperless office — In the paperless office, there is total connectivity among all aspects of practice-management and clinical care. Computers located at all workstations, including treatment rooms, enable a seamless transfer of information that starts with scheduling and ends with electronically processing insurance claims.
Intraoral video camera — This is a significant diagnostic tool that enhances the visibility of areas of the mouth that are difficult to see, and it also makes it much easier to educate patients about restorative treatment. This is the greatest visual tool for dentists since the mirror. Images are displayed on a monitor, ideally located where the doctor can see it by simply looking up, without twisting the head, and the patient also can see it. Whereas many dental equipment manufacturers have adapted their patient chairs and dental consoles to accommodate digital technology, the unit below is completely integrated without having to add separate items.
Extraoral cameras — These are used with imaging programs to show how the face will change after dental treatment. They are most commonly used in orthodontic practices and also in cosmetic or esthetic dentistry. These are also used by general dentists to provide an additional color-matching reference for a lab making a porcelain crown. The tooth-shade reference guide can be photographed against the patient's teeth and the image can be sent digitally to the lab to correct for differences in color reproduction on the monitor and/or printer receiving the image at the lab.
Digital radiography — This eliminates the need for a darkroom and the need to dispose of processor chemicals and lead film packs, and it exposes patients to far less radiation. One can see the digital image instantly and manipulate it in a variety of ways. With a click, it becomes part of the patient's record.
Operating microscopes — These are being built into many offices today thanks to the significant ergonomic advantage of being able to work while sitting up straight, looking forward at the microscope rather than bending over the patient. This enables all dental practitioners, including dental hygienists, to see better and to work at a high level of magnification (2x-21x).
Networked computer systems — Networked multiple treatment room computer systems integrate clinical software, digital X-ray, and practice-management software to effect seamless transfer of information.
Dual monitors — Monitors for patient and for clinical staff should be properly placed in each treatment room.
Air abrasion — This is an alternative to high-speed handpieces but is appropriate only for certain types of treatments. It is ideal for working on young children.
Cosmetic imaging — Inexpensive image-capture software, digital cameras, and photo-quality inkjet printers are helping dentists shift their practices from routine dentistry to more lucrative and rewarding esthetic dentistry.
Lasers — Lasers are used to treat periodontal disease and also can be used in cosmetic procedures to sculpt the gum line. In the future, it is expected they will be used in oral surgery and by endodontists for cleaning out root canals.
Chairside patient education/entertainment — Patient education has never been easier now that patients can view large images of their teeth taken by the intraoral video camera, look at digital X-rays, and watch DVD presentations on specific dental procedures chairside. CAESY® (Clinically Advanced Education System by Dentistry Online, Inc.) offers two- to three-minute video presentations enhanced by computer animation to explain problems and procedures. For entertainment, a monitor in the ceiling enables patients to watch TV, movies, or calming nature scenes during treatment.
CEREC (CEramic REConstruction) — The CEREC 3 by Sirona uses CAD/CAM technology to produce (chairside) fillings, veneers, onlays, and crowns. The computer creates the restoration using an electronic impression, and the entire process can be completed in one appointment. The patient leaves with the restoration.
Modular cabinetry — The new generation of modular casework accommodates the numerous pieces of equipment that are now part of a high-tech treatment room. Also built into these cabinets are dispensers for gloves, drinking cups, a tissue box, and sharps container. It is particularly efficient to have a through-the-wall cabinet for stocking and removal of trays and tubs without entering the room. It should be noted that using open-plan modular casework in lieu of fixed-wall partitions saves enough space to add one treatment room for every five fixed-wall rooms.
Ambidextrous treatment room — Today, flexibility is the key. New equipment is designed to facilitate ambidextrous use: the patient monitor is mounted on an arm that swings around the toe of the chair as in Figure 3, and the doctor's instruments are on a similar arm (or at the 12 o'clock position), and the assistant's cart is ordered with a swing-away bracket to transfer the hoses to the other side of the cart when assisting from the right side of chair.
Sterilization — With the increased emphasis on sterilization discussed earlier, a number of vendors have developed research-based engineered modular systems such as the Steri-Center by Triangle and one by the same name from Midmark.
Looking ahead
No doubt 10 years from now we'll look back on today's technology with some degree of good-natured amusement, but it's unlikely these changes will be as radically different from those in 2003 as today's changes are from the standards of practice in 1993.
Jain Malkin is president of Jain Malkin, Inc., a San Diego-based interior architecture firm specializing in healthcare facilities. She teaches at Harvard University in the Graduate School of Design, lectures widely on the design of healing environments, and is the author of "Medical and Dental.Space Planning, Third Edition." Illustrated with more than 580 photographs and drawings, the book is available from John Wiley & Sons, Inc., by calling (800) 225-5945 or online at www.amazon.com.