WHEN do we become Perio Savvy?
When do dental practitioners become perio aware? I mean really aware. Yes, we all took periodontics courses in dental school and performed the obligatory scaling and root planing for our boards, but how many times do we consider periodontics before we look at restorative needs? According to “Oral Health in America: A Report of the Surgeon General,” 85 percent of adults older than 18 are affected by periodontal disease.1 We would like to think all practitioners consider the foundations prior to restoring the structures, but do we?
Let’s take a trip back to dental school. We had to take a series of coursework to prepare for patient care. Mannequins and dentecs became our friends (if not our mobile, uncompromised patients). We scaled on plastic root structure and sometimes on extracted teeth. We were meticulous - and slow - while we probed each other, only to find barely 3 millimeter sulcular depths. But, in addition to our diligent probing, we were also setting plastic teeth, carving wax, and learning about the biochemistry of gypsum crystals.
Progressing into the clinical program, we were assigned a group of patients with a list of requirements or tasks essential to graduate. Regardless of the methods of assessment and numbers of procedures necessary, all students went through the process of treating complete patients. Treatment planning and comprehensive care for all patients prepared us for the boards required to gain licensure in a state or region. Additionally, these skills are the basis for the standard of care when we leave our educational settings and enter our professional practices.
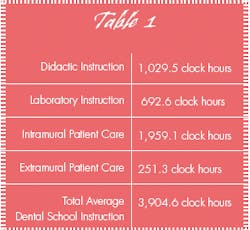
The American Dental Association Accreditation Standards for Dental Education programs do not detail how many specific courses, instructional hours, or clinical experiences a dental education program must present in periodontics.2 Although, according to the 2001-02 Survey of Predoctoral Dental Education, the mean number of didactic clock hours in periodontics is 65.4; laboratory instruction mean is 25.7 hours; and patient care is 239.2 hours, for a total mean clock hours of instruction in periodontics of 295.8.3* The entire dental school program consists of an average of 3,904.6 hours of total instruction, and perio-dontics is about 7 percent of the curriculum. It doesn’t diminish the importance of the treatment of this huge component of our professional practice, but does it predict future focus?
Now, after dental school came the beginning of our real dental lives. How much of that intricate probing are we still performing? Not even considering the cost of dental school education, a residency, or practice start-up, we face patients in our chairs who appear with bevies of dental issues - not only periodontal disease. Are the periodontal needs of our patients fully addressed, or do we allow some of the probe readings to slip away in lieu of restorative care? Again, don’t we need that solid foundation prior to building a house?
Sometimes in our busy practices, we treat a broken tooth or place a full-coverage restoration prior to considering the underlying support. No, this isn’t a correct treatment plan, but when we face patients in pain, esthetic concerns, or loss of tooth structure, the restoration may come before the treatment of burgeoning periodontal disease. We may also leave our periodontal patients to our hygienists, only giving cursory checks and quick hellos while running to the next treatment room to restore implants or place permanent fixed prostheses.
Periodontal disease is an infection that creates a full inflammatory response in reaction to the stages of the disease. I heard someone say that if a patient were bleeding from his or her ear, he or she would rush over to the emergency department of a hospital and probably disobey traffic signs, but when our patients’ gingival tissue is hemorrhagic, they don’t seem to care. Could it be because sometimes we do not center on the infection underlying the bleeding, but merely mention an increase in flossing or brushing to remove plaque? We need to adjust our priorities so we may concentrate on every patient’s periodontal needs.
Let’s refocus on the infection. We know that periodontal disease is caused by bacteria (primary etiology). Genetics determine the susceptibility and resistance of the host (gingiva). Genetics modify the host reaction to the bacterial attack.It affects people differently. A person with a strong set of genetics and excellent home care may have gingival issues from certain medications. Another person with horrible genetics (poor host resistance) may do everything correctly and still suffer from periodontal disease. So, genetics is really the ballpark where everything happens. Hormones (puberty, pregnancy), stress, medications, systemic diseases (diabetes specifically, but there are many others), and poor nutrition are the players in the ball field. They all influence how the body will react to the bacterial attack.
We know the plaque biofilm begins innocuously as nonpathogenic, normal intraoral bacteria that forms almost immediately after brushing, flossing, and dental prophylaxis. This is not a commercial for “Well, if it forms immediately, then aren’t we in a losing battle, so why bother?” Absolutely not. The matrix can be disrupted by home and professional care, so that is why we need to bother. We must reinforce to patients the need to perform daily home care. The later entrants in this biofilm collection are the anaerobic players that cause the destruction and inflammation. These anaerobes are nasty pathogens that cause the most damage inside the sulcus. Remember, they can’t go out to eat, so they survive in their own little world - the protected sulcus. Depending on the depth of the sulcus, they have unlimited party space and limitless ability to damage bone and supporting structures.
Research has shown a relationship between periodontal diseases and diabetes, cardiovascular disease, stroke, and adverse pregnancy outcomes such as preterm births and low-birth-weight babies. This relates to the inflammation component of periodontal disease. Periodontal disease is an infection that sets off an inflammatory response. The bacteria in the biofilm release several products such as lipids, proteins, and acids that stimulate osteoclastic activity. This causes the destruction of bone tissue and triggers an immune response in the body. As a component of the immunological cascade response, the liver triggers release of C-reactive protein. An elevated CRP causes an increase in cardiovascular incidents such as heart attacks and strokes.
With all of this information, why don’t we focus on every patient’s periodontal health? Every patient should receive probe readings as part of his or her initial comprehensive oral evaluation and routine preventive maintenance. We must be proactive and diligent in our oral-hygiene instructions to our patients. In most offices, this task is relegated to a hygienist, but as dentists, we must spend more than a few minutes during each periodic evaluation discussing the importance of home care and the connection between plaque and inflammation. The message is stronger when delivered by an entire team.
Several companies explain home care and why we must improve oral hygiene to improve oral conditions and systemic health. Johnson & Johnson has “Flossing Matters - Bringing Out the Flosser in Every Patient.” This unbranded dual set of materials (one for the patient and one for the professional to use chairside) educates patients on oral care based on their age groups and suggests to practitioners how to motivate patients to floss. OraPharma has a patient-centered brochure about asking for “numbers,” or periodontal probe readings. OraPharma’s new education materials make it easy for dental professionals to teach patients that periodontal disease is a chronic oral infection. This campaign increases patients’ knowledge of periodontal disease and makes diagnosing and treating the disease easier. The ADA has other unbranded materials available for the show-and-tell portion of patient education.
Considering treatment options for periodontal disease, we have several surgical and nonsurgical approaches available. Oftentimes, patients in need of scaling and root planing may go unscheduled. Because of time constraints, insurance issues, cost, or our feeling that patients won’t understand the need, we must discuss the ramifications of unchecked periodontal disease with patients and educate them toward proper treatment regimes. Pregnant women must know about the importance of effective home care. Numerous recent studies have shown women with periodontitis are seven to eight times more likely to have preterm or low-birth-weight babies.4 Cardiac patients, as well, need to know the risk of periodontal disease and increases in their circulating CRP levels.
In addition to mechanical scaling and root planing, adjunct therapies are also beneficial.Some practitioners use systemic antibiotics, singly or in combination, for a specific regimen. Antimicrobial mouth rinses such as Peridex or other chlorhexidine preparations are available.Finally, because scaling and root planing alone cannot reach the base of all pockets, newer locally applied antibiotics, or LAA, which offer precise placement of the drug directly into the sulcus, are also excellent therapies. Again, referencing the Surgeon General’s Report on Oral Health, “antimicrobial agents [are placed] directly into the pocket. Antimicrobials incorporated into either resorbable or nonresorbable interpocket-delivery systems have been studied in randomized, double-blind, controlled, clinical trials and are now FDA-approved and on the market (Goodson et al. 1991, Jeffcoat et al. 1998). When used as an adjunct to scaling and root planing, gains in clinical attachment level and decreases in probing depth and gingival bleeding were demonstrated.”1 Three effective products are Arestin, Atridox, and PerioChip. They may be placed by dentists or dental hygienists.
Now let’s get to the bottom line. According to Dr. Gordon Christensen at a recent lecture, we may be missing 10 percent of our periodontal treatments. It isn’t that we aren’t properly diagnosing, but another 10 percent of our patients might need active periodontal treatment that can be performed in our offices. If we are not treating this segment for whatever reason, then we are losing money. By increasing the necessary periodontal treatment, we will always increase the bottom line. It isn’t as though we’re looking for things to do; they are most likely available for us or our hygiene teams to treat.
Consider this: The most recent Dental Economics fee review stated that scaling and root planing (4341) would generate an average of $210 per quadrant, depending on the area of practice. Chemotherapeutic agent placement (4381) ranges from $40 to $50 per tooth. Adding a few patients per week in the hygiene schedule will produce revenues of a minimum of $3,000 per week. I wasn’t a math major, so extrapolate that out to a 40-week year (and most of us do work more than 40 weeks in our hygiene departments). This translates to more than $120,000 a year.
Being perio savvy may sound like a no-brainer. At least, we protect our patients from tooth loss and possible systemic diseases. At best, we protect ourselves from lawsuits. Are you savvy? The real question is, why not?
References:
1 Oral Health in America 2000: The Surgeon General’s Report on Oral Health http://www2.nidcr.nih.gov/sgr/sgrohweb/home.htm Accessed October 24, 2005.
2 Commission on Dental Education, Accreditation Standards for Dental Education Programs 1998.
3 From Figure 7a: Average Number of Clock Hours for Clinical Science Subjects by Didactic and Laboratory Instruction, 2001/02, ADA Survey of Predoctoral Dental Education, Volume 4, Curriculum, page 62. This was published in April 2003.
4 Jeffcoat MK, Hauth JC, et al., Periodontal disease and preterm birth: results of a Pilot Intervention Study, J Periodontol. August 2003; Vol 74 (8); 59-63.
The author wishes to thank Dr. Terry J. Annex and Jeff Gartman, ADA reference and online resource librarian, for their assistance.
*The schools reporting in excess of 400 total clock hours are: University of Connecticut, University of Colorado, Nova Southeastern University, Medical College of Georgia, University of Oklahoma, Oregon Health and Science University, University of Pennsylvania, Medical University of South Carolina, Virginia Commonwealth University, and Marquette University.