Women's Wellness Part II: Arthritis
Are you ready for an emergency?
by Risé Lyman, DDS, MBA
It seems like everyone knows to be prepared for terrorist attacks or natural disasters in our country. As dentists, we are normally prepared for emergencies in our office with drug kits and even defibrillators. We prepare our schedules daily for emergency patients and where they might fit best in our normal routines. But what about an emergency of the doctor, practice owner, or key producer?
Many times we take our bodies for granted. We continue to work even when it hurts. We harp at our patients to seek treatment before they hurt. A lot of diseases, such as rheumatoid arthritis, present without pain initially. Rheumatoid arthritis attacks the tissues or synovium and causes swelling. It covers the joints and destroys bone and cartilage. The exact cause is not known, but it affects about 1 percent of the population - women more often than men.
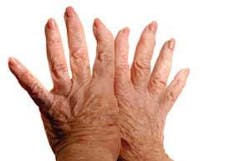
In the early stages of the disease, joint problems are the most common symptoms. A general sense of being tired or just not feeling right often happens before the slow start of joint pain and swelling. Morning stiffness is a frequent complaint. As the disease continues, symptoms often include swelling of joints in the hands, wrists, elbows, shoulders, hips, knees, and feet. The swelling usually takes place in the same joint on both sides of the body, known as symmetrical swelling. Rheumatoid arthritis may result in pain and deformity. Occasionally, the disease affects other organs of the body, such as the heart, eyes, and lungs.
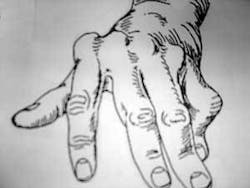
How does it affect our livelihood - our hands? The most common complaint is swelling of the hands at the knuckles, often in the wrists and large knuckles in the middle of the hand, which is what happened to me on my right hand, but only on the middle finger. The swollen tissue may destroy ligaments that hold the joints together and damage cartilage and bone resulting in deformities. The wrist may turn toward the thumb side of the hand causing “ulnar drift” of the fingers (see Figure 1). The swollen tissue may also produce damage and cause the tendons to rupture. Swelling may occur and cause pressure on nerves, called carpal tunnel syndrome, or lumps over various joints, called rheumatoid nodules.
Treatment may include nonsteroidal, anti-inflammatory, cortisone-like medications for pain; splinting to avoid damaging swollen joints; and aids for daily activities due to limited movement. Surgery may be considered when other treatment does not work. Surgical procedures may include removing swollen tissue surrounding joints and tendons, tendon repair, nodule removal to improve appearance, arthroplasty to replace knuckles, or total joint replacement.
After months of increasing pain from grasping motions and minimal relief with medications, I decided to have surgery. An Ascension MCP Implant (see Figure 2) was placed after tissue, bone, and nodule removal along the knuckle of the middle finger. After several months of physical therapy and splint appliances, a lag in the extensor tendon persisted. Adhesions seemed to prohibit full extension of the tendon. A second surgery was planned for tenalysis to free the tendons from adhesions. Three days postoperatively, the tendon ruptured as a result of postsurgical swelling, and a third surgery was planned to repair the tendon. The tendon was repaired, but because of more complications involving healing of skin covering the wound site, a fourth surgery was necessary to place a skin graft. The fourth surgery included joint replacement again, a tendon transfer from the palm, a radial artery transfer, a skin graft from the forearm, and a tummy tuck to obtain a graft for the forearm. I wish that was the end, but it is not. I now have no extension or flexion of the middle-finger tendons, and another surgery is planned to improve function.
I write about this experience because I am a healthy person. I take no medications besides a multiple vitamin, calcium, and an occasional Advil or Tylenol for pain. I have never had any surgical complications. I have since had extensive blood tests to rule out von Willebrand disease, leukemia, and other possible factors. Our bodies can react strangely when we least expect it. I had the best surgeons in my region of the United States. Would I have the first surgery again? Knowing what I know now, I would not.
What about the emergency status in my office? Well, I have not been able to fully work since the first surgery in September 2005. I work with my husband, who can pick up my slack. We never know from day to day my capability to treat patients.
Are you prepared for such an event? Do you have a good disability policy? Do you have dentists who would cover your office for you? Do you have retirement if you are unable to work? Are you ready for an emergency?
Risé Lyman, DDS, MBA
Upon graduating in 1985 from the University of Texas Health Science Center Dental School in San Antonio, Dr. Lyman started her own practice, which her husband joined in 1991. She is a past president of the AAWD and serves as president of the Smiles for Success Foundation. E-mail [email protected].