A new 'flossophy' exposes the myths surrounding the efficacy of flossing
"Cleaning between the teeth at the gum line is absolutely needed!On the other hand, there is not one published article that can be cited showing floss is superior to other interproximal aids, in spite of our beliefs. Why should flossing get a free pass when in other situations we always say, 'Show me the proof?'"
I want to discuss what you could say to patients who ask whether floss is useful for cleaning their teeth in light of the recent discussions and hope my experience can help you communicate differently.
Times have changed
In a way, it appears to be a no-win situation. Saying it is not proven to work when all the professional organizations say it does puts you at odds with your colleagues. On the other hand, if you agree that flossing is beneficial, you appear to be defending the status quo and patients still won't floss no matter what we say or do. Again, I'm in the camp that believes flossing really does not clean gum tissue biofilms as well as it does tooth biofilm. There are better alternatives that are much more effective and accepted by patients.
So, how will you and your team respond if you have promoted flossing to your patients for years or even decades as "gospel" and now media reports say it appears to be of little help? Patients want an honest, impartial discussion on this issue. So what is the best method of cleaning interproximally both tooth and surrounding gum tissue at the same time with equal pressure?
Times have changed. I was taught that amalgam is the best filling material, and it is still taught that way. Do you believe it is? I was taught stomach ulcers were the patient’s fault until we learned it is an infection to be treated with antibiotics. Every time our fundamental beliefs are challenged, our response is usually defensive rather than making a recommendation based on new evidence.
Similarly, we were all taught that floss was the best way to clean the teeth but gums were never mentioned. Do you know it is physically impossible to predictably clean gum biofilm with floss even though it does clean tooth biofilm well? Every patient you see is looking for alternatives to floss because few of them floss and those who do were coerced into doing it by us.
Cleaning between the teeth at the gum line is absolutely needed!On the other hand, there is not one published article that can be cited showing floss is superior to other interproximal aids, in spite of our beliefs. Why should flossing get a free pass when in other situations we always say, “Show me the proof?”
Why I don't routinely teach flossing
If that is the case, then we need to get to the head of the new parade. If you have not tried using Soft-Picks and Stim-U-Dents as the primary way to clean interproximal tooth and gum biofilm thoroughly, as well as as a diagnostic tool to detect and control most interproximal bleeding, then you are not offering your patients some of the best options available.
First of all, I teach flossing for a few occasions—if you have food stuck between the teeth, if you are cleaning dental implants or bridgework, and if nothing else will fit. What is the basis for this "flossophy" which puts my neck out there? Let's look at the science of flossing apart from the question of how good it is or isn't.
These are my three reasons why I don't routinely teach flossing aside from the fact patients won't do it.
- Published science says it doesn't clean effectively. In a meta review published in the Journal of Clinical Periodontology in April 2015, Chapple et al. state the obvious even if it goes against popular opinion: "Flossing cannot be recommended other than for sites of gingival and periodontal health, where interdental brushes (IDBs) will not pass through the interproximal area without trauma. Otherwise, IDBs are the device of choice for interproximal plaque removal. We support the almost universal recommendations that all people should brush their teeth twice a day for at least 2 min." (1) That is a strong statement published in a highly respected peer-reviewed periodontal magazine. But why doesn't flossing work?
- Physics is not on the side of flossing. You can't push string, and you can't you clean the inside of a bowl (the shape of the interproximal tissues) with floss. Flossing can’t fully disturb the interproximal tissue biofilm because it is physically impossible.
- The space between the tooth and gum, especially in loose swollen tissues, is wider than floss so it can't engage the tooth and gum at the same time. Biofilm composition is different on the gum tissue and the tooth. Both biofilms adhere tenaciously to the surfaces. Firm pressure is needed to disturb them. Flossing cannot do it as well as interproximal aids for tissue biofilms.
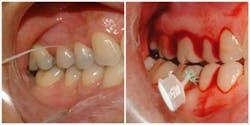
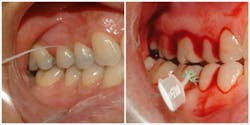
Prove it with patient examples! Look at this comparative photo showing no bleeding during flossing, but severe bleeding during interproximal cleaning.
For a very dramatic demonstration of this, watch the video below of a patient with periodontal disease having his interproximal areas cleaned with a Soft-Pick—the blood flows as if it is coming out of a faucet!
Appearance is a subjective observation whereas the Papillary Bleeding Score is objective and clearly shows health or disease visually and emotionally. As you have seen it is actually the most important test to do to detect active periodontal disease and to notify your patient of its existence.
How to guide your patients
So how do we respond to questions regarding the flossing debate? This is the perfect opportunity to discuss home care techniques and your practice "flossophy" when patients ask the question.
Try floss first. If there is no bleeding, congratulate them, but do another test before you commit to recommending flossing. It is the previously mentioned Papillary Bleeding Score. Use a Soft-Pickto rub the inside and outside of the lips and the labial tissues. Do you see any signs of bleeding? Ask the patient if it hurts or bleeds. If there are no signs of bleeding or pain, tell them you are going to rub it between the teeth firmly. Healthy tissues never hurt or bleed upon this type of probing. Have a mirror handy as you do this. Tell them if it bleeds or hurts that they have an infection and/or inflammation.
If they bleed after using interproximal devices but not floss, then you have your answer as to which method is superior. When they bleed, ask them if they believe they are "kissable"? This is an emotional moment! When they ask how to stop the bleeding, please don't say “Brush your teeth, floss, and have your teeth cleaned twice a year!” Believing means the presence of pathogenic bacteria that cause periodontal issues and bacteremia. It is serious. Does a physician watch bleeding and say, "Come back in six months to check if it has stopped?"
If there is a lot of bleeding, this is the chance to discuss perio charting, perio-modular care, biofilm, analysis, disclosing, irrigation, antibiotic rinses to kill the perio-pathogens, and a reevaluation appointment to see if the treatment was successful. By following these suggestions, everyone wins. Plus, patients get an individualized exam to help you accurately answer the question "Do I need to floss?" Keep in mind that there is a perception that interproximal brushes cause gingiva to traumatically recede. What actually happens is the tissue that we thought was healthy shrinks in three days; they change from "beer-belly" gums to "six-pack abs" gums. You will be surprised how quickly this happens, and bleeding and soreness stops on the third day, guaranteed! On top of this, patients will keep using the interproximal brushes on a daily basis with no coercion.
Remember the Australian physician who stated in 1982 that stomach ulcers were caused by infections? He was laughed at and it took 16 years before it was the accepted treatment; he got the Nobel Prize for Medicine in 2006. To some, this flossing debate appears to not be on the same level of medical importance as the discovery that stomach ulcers are caused by infections. But I believe it is.
If we teach a technique that doesn't work as well as others that are readily available and easier to use, aren't we contributing to the spread of the very disease we are trying to prevent? With the oral systemic link so much in the news, shouldn't we be promoting the best way of addressing this emerging issue to avoid potential legal liability, not to mention our responsibility to do our fiduciary duty to do no harm?
Despite our best efforts as dental professionals, 75% of our patients have periodontal disease. Why? Our traditional flossing recommendations are one of them. Another is we tell patients to brush their teeth but they also need to brush their gums, which is where the bacteria are located.
RELATED READING:Why the new model of periodontal disease matters
Disinfecting the mouth before therapy with antimicrobials as physicians do and post therapy with OTC rinses is needed in addition to interproximal cleaning. We also need to disclose every patient during every appointment. We need to put the brush in their hands and teach, demo, or coach them on how to brush instead of merely telling them how to do it. All of this will make a huge difference.
So I challenge every dentist and hygienist who recommends flossing as the primary method of cleaning interproximally to use a Soft-Pickor equivalent product on five hygiene or restorative patients in a row and see what happens. You will change your opinion when you see the bleeding in healthy-looking mouths. I hope you will have an open mind to what I have recommended.
Reference
1. Chapple IL, Van de Weijden F, Doerfer C, et al. Primary prevention of periodontitis: managing gingivitis. J Clin Periodontol. 2015;42 Suppl 16:s71-6. doi: 10.1111/jcpe.12366.
MORE READING:Dental profession reacts to Associated Press report about flossing evidence