Pathology case: "My doctor said I have an infection on one of my top right teeth"
Editor's note: Originally published July 5, 2016. Updated March 2024.
Case presentation and clinical assessment
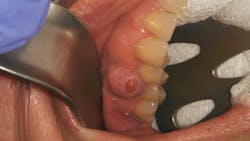
A 50-year-old female presented for a new-patient exam upon the recommendation of her general practitioner. Her chief complaint: “My doctor said that I have an infection on one of my top right teeth.” She pointed to a raised tissue mass between teeth nos. 4 and 5.
The patient was on a prescription of Keflex given by her MD for this “infection.” Other health considerations: penicillin allergy and a history of type 1 and 2 herpes.
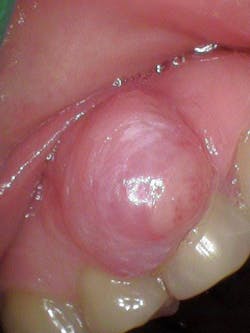
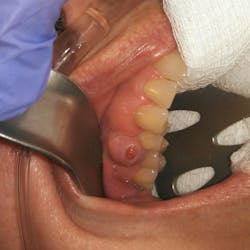
Clinical assessment revealed a 6 mm pink, raised, firm mass of osseous tissue measuring 12x12 mm. It was not tender to palpation and did not bleed easily when manipulated (figures 1 and 2). Radiographic assessment was within normal limits (figure 3).
Differentials
- Pyogenic granuloma
- Hormonal tumor
- Fibrous hyperplasia
- Osteosarcoma
- Chondrosarcoma
- Metastatic carcinoma
- Peripheral odontogenic fibroma
Final/definitive diagnosis: peripheral ossifying fibroma
Peripheral ossifying fibroma (POF) is considered to be part of the family of lesions that may be defined as “an increase in the size of an organ or tissue due to an increase in the number of its constituent cells, as a local response of tissue to an injury.”1 POF, a benign overgrowth of gingival tissue,1 is the most common form of odontogenic fibromas.2 It is thought to be derived from the overlying gingival epithelium. It frequently contains calcified deposits of cementum1 and, if significant enough, these calcifications may show up on radiographs with a slight radiopacity. Its location is most often found in the interdental papillae and often will separate adjacent teeth.
“Some 50% occur in patients between the ages of 5 and 25 years, predominantly female patients. Eighty percent occur anteriorly to the molars.”1 Since the lesions are raised, they typically have an erythematous surface due to chronic irritation. Treatment is excision with the attempt to remove underlying attachment to the bone. Recurrence is rare at 13%–16%.1
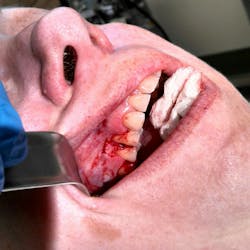
In this particular case, the patient was referred to an oral surgeon for an assessment and biopsy. The lesion was removed and sent to pathology with a definitive diagnosis of peripheral ossifying fibroma (figures 4–6). The gingival defect created by the removal of the fibroma was allowed to heal by secondary intention and will likely undergo a free gingival graft later to reconstruct the attached gingival margin. The patient managed well without complications.
References
- Wood NK, Goaz PW. Differential Diagnosis of Oral and Maxillofacial Lesions. 5th ed. Mosby; 1997:130-143.
- Sapp JP, Eversole LR, Wysocki GP. Contemporary Oral and Maxillofacial Pathology. Mosby; 1997:140-141.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].