Evaluating causes for success and failure in endodontics
Root canals fail. As much as we don’t like to admit it, they do. It goes without saying that over the course of time, advancements in the field due to technology and understanding the microbiology involved with endodontic pathology have indeed increased the success of root canals. It is, therefore, important to consider the reasons for the successes and failures of root canal therapy (RCT) so we can better understand the process and how it plays a role in our own private practice.
ALSO BY DR. STACEY SIMMONS |Internal resorption: A brief review and case report
The rationale for endodontic treatment is to eradicate the infection, prevent microorganisms from infecting or reinfecting the root and/or periradicular tissues (3) by filling or obturating the cleaned and shaped systems, and prevent future recontamination of sealed root canals. (4) Consequently, failure to achieve these criteria results in RCT failure or continued presence of inflammation and infection. Therefore, the prognosis for RCT is based on several factors that can be divided into three categories: preoperative, operative, and postoperative causes.
ADDITIONAL READING |The top 5 endodontic articles from DentistryIQ in 2014
Preoperative causes that influence RCT outcome include misdiagnosis, errors in treatment planning, poor case selection, or treatment of a tooth with a poor prognosis. (1) Often, radiographic interpretation or lack of proper radiographs can interfere with the operator’s ability to predict the outcome, resulting in poor operative execution. Sjogren et al. indicated that one of the most important factors influencing the prognosis of endodontic treatment is the preoperative status of the tooth. (2) He furthermore referenced studies demonstrating that the success rate in endodontic therapy is significantly influenced by the presence or absence of a pretherapeutic radiographic lesion. (2) Teeth with an apical radiolucency may show up to a 20% lower success rate than teeth without such lesions. (2) Regardless of how the tooth presents, proper interpretation and subsequent treatment planning prior to initiating RCT will allow for better care and outcome.
Operative causes that influence the prognosis of RCT can be divided into two categories: mechanical and biological. Mechanical considerations include: cavity preparation/access, cleaning and shaping, instrument separation, perforation, missed canal(s), and obturation quality (under-/overfill). (1) Biological objectives involve removal or reduction of existing and potential irritants from the pulp space, sealing of the space, microbial control, and management of periapical inflammation. (1) Understanding the complex endodontic microbiology so that it can be most effectively eradicated during RCT can ensure that the biological objectives can be met clinically. (3) Interestingly enough, there are several microorganisms that are self-sustaining and resistant to antimicrobial treatment and can survive in the root canal after biomechanical preparation; i.e., prevotella, campylobacter, actinomyces, and eubacterium (a complete list can be found in the literature). (3) Knowing this, the presence of persistent infection following RCT can be attributed to the presence of the aforementioned microorganisms.
Postoperative causes that have an effect on RCT outcome occur when 1. there has been a delay in the restoration of a tooth following root canal treatment; 2. the coronal temporary filling, placed immediately following root canal treatment, is compromised; 3. the tooth is fractured and the canal system is exposed prior to final restoration; 4. the final restoration, regardless of type or design, lacks ideal marginal integrity or cannot withstand the forces of occlusal function, and deteriorates; or 5. recurrent decay is present at the restoration margin(s). (5) A combination of any of the aforementioned causes may ultimately dictate outcome.
Prognosis with RCT and variability of treatment will dictate that each case be assessed individually, taking into account all relevant factors. (1) Regular follow-up post-CT and subsequent restorative completion is furthermore recommended.
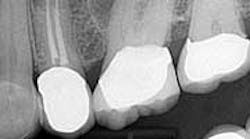
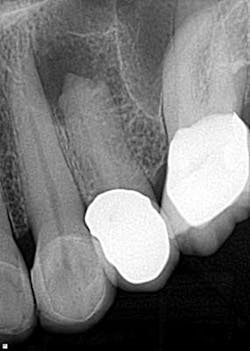
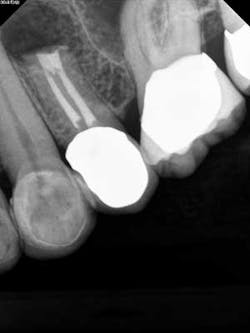
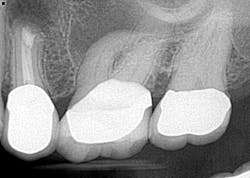
Case report A healthy 61-year-old female presents with a chief complaint of pain and discomfort in the upper left quadrant. A radiograph revealed a large radiolucency at the apex of tooth No. 12. An irregular root apex was also noted. Clinically No. 12 was sensitive to percussion and palpation in the buccal vestibular area. There was no response to cold. Diagnosis was necrotic tooth No. 12 with associated periapical abscess. RCT was recommended and the patient was referred to a specialist for completion. RCT was completed — no complications were noted and the prognosis was given as good. (Figs. 1 and 2) The patient was placed on recall by the endodontist for reevaluation of the lesion in 12 months.Fig 1. Fig. 2Eight months later, the patient presented back to the office stating that she felt pressure again in the upper left area. A radiograph of No. 12 showed an increased radiolucency around the apex of tooth No. 12. Furthermore, there was a draining fistula in the buccal vestibule. Diagnosis was persistent infection/disease, likely due to the initial presentation and presence of the cyst. (Fig. 3)
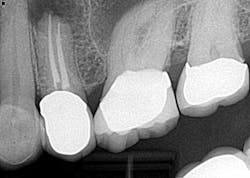
Fig. 3The patient did not want to lose her tooth and was referred back to the specialist for an evaluation and consideration of options. It was discussed and recommended that the patient have root end resection with a root end filling (apicoectomy). She agreed, and the treatment was completed. There was suspicion as to the nature of the pathology of the cyst-like lesion, so it was sent out for biopsy. Diagnosis was chronic, localized osteitis and actinomyces colony. Conclusively, the source of the infection was eradicated but the presence of the actinomyces microorganism was enough to sustain a chronic infection post-initial RCT. (Fig. 4)
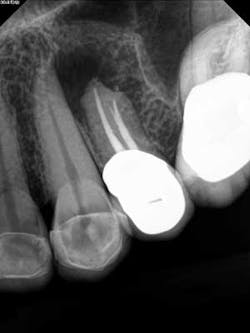
Fig. 4A two-month follow-up with the patient revealed a recovery of the area with loss of pressure and pain. A radiograph of the area showed initial stages of healing and bone recovery. She has been placed on a recall program for continuous assessment of the area. Prognosis is good. (Fig. 5)
Fig. 5
Success with RCT varies, and it can be said without much argument that a comprehensive approach to treatment is in the patient’s best interest. We can enjoy a higher success rate with RCT if we maximize available resources when diagnosing, treating, and rendering post-care follow-up.
References
1. Walton RE, Torabinejad M. Principles and practice of endodontics. 2nd Edition. WB Saunders Company. 1996;324-334.
2. Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. Journal of Endodontics. Oct. 1990;16(10).
3. Narayanan LL, Vaishnavi C. Endodontic microbiology. J Conserv Dent. Oct.-Dec. 2010;233-239.
4. Swanson K, Madison S. An evaluation of coronal microleakage in endodontically treated teeth. Part I: Time periods. Journal Endodont 1987;13:56.
5. Coronal leakage: Clinical and biological implications in endodontic success. American Association of Endodontics. Fall/Winter 2002 Publication.
About the Author
Stacey L. Simmons, DDS
Editorial Director of DE's Breakthrough Clinical e-newsletter
Dr. Stacey Simmons grew up in Hamilton, Montana. She did part of her undergraduate work at Purdue University and then received her bachelor’s degree in exercise physiology from the University of Utah. After applying to both medical and dental school, she decided that dentistry was her career of choice. She received her DDS degree from Marquette University School of Dentistry in Milwaukee, Wisconsin, in 2004. In private practice, she focuses her care on prosthodontics and cosmetic dentistry. She is a guest lecturer in the Anatomy and Physiology Department at the University of Montana. Outside the office, she trains for triathlons and spends time with her family. You may contact Dr. Simmons by email at [email protected].
In 2015, Dr. Simmons became the editorial director of DE's Breakthrough Clinical with Stacey Simmons, DDS, an e-newsletter focused on breaking through plateaus in clinical practice. Subscription information may be found here.
Updated May 4, 2016