Electronic determination of working length: more accurate than radiographs?
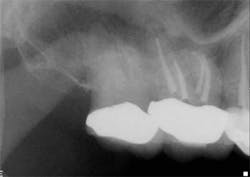
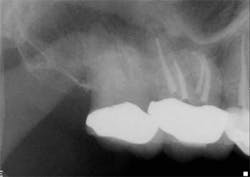
Removing bacteria and pulp tissue from the root canal system is necessary to achieve endodontic success. (1,2) The only way this can be accomplished is with an accurate determination of the working length. Historically, this has been done through the use of radiographs. However, the actual canal terminus (minor constriction) can vary from the radiographic apex by as much as three millimeters, and the apical foramen coincides with the radiographic apex in only 17% to 46% of cases. (3,4,5,6) When using radiographs to determine working length, an arbitrary measurement within the canal is chosen as the desired end point. For example, most clinicians choose to fill the root canal between 0.5 mm and 1.0 mm from the radiographic apex. The clinical significance of this arbitrary choice can have dire effects on clinical success. If the canal terminates more than 1.0 mm from the apex, an overfill will result. This may or may not be an issue depending on the cleanliness that was achieved during the instrumentation and irrigation phases of treatment. On the other hand, if the canal exits at the radiographic apex and the instrumentation and obturation are terminated 0.5 mm short of the canal terminus, bacteria will persist in the root canal system and may result in post-treatment disease.
ALSO BY DR. DAVID LANDWEHR | Endodontic case study: referred pain leads to diagnostic uncertainty
According to the endodontic literature, using an electronic apex locator (EAL) is more accurate than radiographs in determining the location of the apical constriction. (7,8) An in vivo study reported an EAL could measure the foramen to within +/- 0.5 mm in 96% of teeth. (9) Although it was a problem with first-generation apex locators that measured length via impedance or resistance, the presence of fluids or canal lubricant in the canal will not lead to inaccurate readings with modern apex locators. (10) Additionally, the accuracy of an EAL is not dependent on pulpal status, as there is no difference in the accuracy of an EAL if the pulp is vital or necrotic. (11,12) Many practitioners incorrectly consider file size to be an important determinant of accuracy for an EAL, and there was a historical, but unfounded concern about the safety of the EAL in patients with cardiac pacemakers. (13,14,15)
ALSO BY DR. DAVID LANDWEHR |Endodontic case study: an alternative method for the cleaning and shaping of a mid-mesial canal
There is a learning curve involved in the use of an EAL, and the use of a radiograph to confirm the accuracy of the EAL reading would be recommended until the clinician has complete confidence in this technique. The best time to initially determine working length with an EAL is following straight-line access, opening of the orifice, and establishment of an unobstructed glide path. This will provide the most consistently accurate readings, because the orifice will be centered over the canal. (16,17) Taking this initial reading following access, prior to final instrumentation of the apical portion of the root canal, and immediately in advance of obturation will provide the most accurate results. Taking several readings will take time, especially in multirooted teeth. However, increased accuracy will make the time well spent, and multiple EAL measurements can be taken in the time required to obtain one well angled and clinically useful working length radiograph.
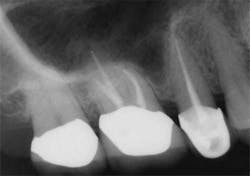
Clinicians rely on a variety of methods to determine working length including, but not limited to, the tactile sensation of feeling the file “pop” through the apex, bleeding on paper points, and radiographs. However, proper use of the EAL, in conjunction with a well-exposed and properly angled preoperative radiograph, will result in the most accurate and reproducible means of determining the true working length. Ideally, this will lead to more predictable and efficient treatment outcomes to maximize both patient comfort and root canal success.On routine six-month recall, the patient was asymptomatic and the access opening was restored. The apical and crestal bone was unremarkable. The follow-up radiograph was taken from different horizontal and vertical angles. Now the fill-in palatal root looks nearly flush with the radiographic apex. A case like this clearly illustrates the limitations of two-dimensional radiographs and the benefits of an EAL for the most accurate working length determination.
References
1. Kakehashi S, Stanley HR, Fitzgerald RJ. The effects of surgical exposures of dental pulps in germ-free and conventional laboratory rats. Oral Surg Oral Med Oral Pathol 1965;20:340-349.
2. Möller AJ, Fabricius L, Dahlén G, Ohman AE, Heyden G. Influence on periapical tissues of indigenous oral bacteria and necrotic pulp tissue in monkeys. Scand J Dent Res 1981;89:475– 484.
3. Burch JG, Hulen S. The relationship of the apical foramen to the anatomic apex of the tooth root. Oral Surg Oral Med Oral Pathol 1972;34(2):262.
4. Green D. Double canals in single roots. Oral Surg Oral Med Oral Pathol 1973;35:689.
5. Kuttler Y. Microscopic investigation of root apexes. J Am Dent Assoc 1955;50:544.
6. Pineda F, Kuttler Y. Mesiodistal and buccolingual roentgenographic investigation of 7275 root canals. Oral Surg Oral Med Oral Pathol 1972;33:101.
7. Pratten DH, McDonald NJ. Comparison of radiographic and electronic working lengths. J Endod 1996;22:173-176.
8. Ravanshad S, Adl A, Anvar J. Effect of working length measurement by electronic apex locator or radiography on the adequacy of final working length: a randomized clinical trial. J Endod 2010;36:1753-1756.
9. Shabahang S, Goon WWY, Gluskin AH. An in vivo evaluation of Root ZX electronic apex locator. J Endod 1996;22:616-618.
10. Jenkins JA, Walker WA III, Schindler WG, Flores CM. An in vitro evaluation of the accuracy of the Root ZX in the presence of various irrigants. J Endod 2001;27:209-211.
11. Goldberg F, De Silvio AC, Manfré S, Nastri N: In vitro measurement accuracy of an electronic apex locator in teeth with simulated apical root resorption. J Endod 2002;28:461.
12. Mayeda DL, Simon JH, Aimar DF, Finley K: In vivo measurement accuracy in vital and necrotic canals with the Endex apex locator. J Endod 1993;19:545.
13. Cianconi L, Angotti V, Felici R, Conte G, Mancini M. Accuracy of three electronic apex locators compared with digital radiography: an ex vivo study. J Endod 2010;36:2003-2007.
14. Garofalo RR, Ede EN, Dorn SO, Kuttler S. Effect of electronic apex locators on cardiac pacemaker function. J Endod 2002;28:831-833.
15. Wilson BL, Broberg C, Baumgartner JC, Harris C, Kron J. Safety of electronic apex locators and pulp testers in patients with implanted cardiac pacemakers or cardioverter/defibrillators. J Endod 2006;32:847–852.
16. de Camargo EJ, Zapata RO, Medeiros PL, Bramante CM, Bernardineli N, Garcia RB, de Moraes IG, Duarte MA. Influence of preflaring on the accuracy of length determination with four electronic apex locators. J Endod 2009;35:1300-1302.
17. Ibarrola JL, Chapman BL, Howard JH, Knowles KI, Ludlow MO. Effect of preflaring on Root ZX apex locators. J Endod 1999;25:625-626.