Is the fear of bone grafting procedures keeping many GPs from placing dental implants?
By Alfred L. “Duke” Heller, DDS, MS, and Robert L. Heller, DDSObviously most general practitioners would agree that financially they would like to increase their office income by doing simple implant placement and restoration, thus keeping the fees for those services in their own cash flow. They also realize that implant dental treatment is a prosthetic discipline with a surgical component! Simple implant surgery starts with mounted models and pre-surgical diagnosis and treatment planning. The result of proper planning will produce a surgical template to help the doctor place the implant where it can be restored. Many times the implant placement comes back from a referring office with the implant out of alignment, and then it becomes compromised at the point of trying to make the prosthetics adapt to a misaligned implant.Considering that the average implant fee is $1,500 to $2,000 per implant and the abutment and fixed crown fee is approximately another $1,500, that is roughly $3,000 to $3,500 that could stay in the general practitioner’s own cash flow to help in this trying economic time. General practitioners can become as skilled as specialists in placing dental implants and should consider placing simple implants for their patients. Patients prefer to have their own dentist treat their dental implant needs rather than go to a different office for treatment.So why do so few general dentists place implants?It can be speculated that many don’t do implants because they don’t like surgery. Some dentists say they don’t feel adequately trained to watch a slide presentation at an implant course and then place implants in their patients. Some say they would like to place their first few implants with someone looking over their shoulder. Others feel that if they need to graft bone at the time of implant placement or before implant placement, they don’t know what materials to use. Bone grafting materials are becoming increasingly abundant in the marketplace. Doctors should seek training where the presenters are not paid to speak about certain bone grafting materials or a certain implant system. They should also seek to find a mentor or individual they can call on the telephone with surgical or prosthetic questions.Case reportA 22-year-old female presents with tooth No. 11 missing. History of patient is that the tooth was lost four years ago due to trauma. Patient would like for the general dentist to place the implant so she can get rid of her present flipper. The initial photo shows that the ridge appears to be sufficiently wide to accept an implant in the maxillary left cuspid area (Fig. 1). Upon tissue reflection, the underlying bone presents with a labial and lingual defect (Fig. 2). Options include a block bone graft or particulate graft with a barrier. A decision was made to use irradiated bone (80%), tricalcium phosphate (20%) mixture, together with Platelet Rich Plasma (PRP) mixture after decortications were done with a 700 XXL bur (Fig. 3). The barrier selected was the Inion GTR Barrier (Reimser Inc., Durham, N.C.) using small tacks (Salvin Dental, Charlotte, N.C.) to maintain the ridge (Fig. 4a). A plasticizer is used, which hardens the membrane to allow maturity of the bone graft without pressure necroses from food or removable appliance. Fig. 4b shows a side view showing the bone mixture under the Inion barrier. PRP (Clinseal centrifuge from Salvin Dental, Charlotte, N.C.) was used in the bone grafting mixture as well as in the completed sutured tissue to enhance bone and tissue growth. PRP was injected under the tissue flap to aid in bone growth at the end of procedure. Six months later, the ridge exposure measured 10 mm buccal-lingually (Fig. 5). As is evident in the photo showing buccal and lingual bone growth, which would not have been obtainable with a block graft, it would have only produced bone on the buccal thin ridge.A 3.7 mm implant was placed easily into the grafted site, leaving adequate buccal and lingual supporting bone for the implant (Fig. 6). Fig. 7 shows tissue closure with 43-0 vicryl sutures (Ethicon by Johnson and Johnson, Langehorne, Pa.). A periapical X-ray shows implant placement in grafted bone (Fig. 8).
Fig. 1 shows the preoperative photo of maxillary cuspid.
Fig. 2 shows the buccal and lingual bone thickness present after reflection of tissue. (Bone thickness next to lateral measured 2.8 mm. Bone thickness next to bicuspid measured 4.5 mm.)
Fig. 3 shows decortication of remaining bone with a 700 XXL bur, allowing for penetration of the labial cortical bone into the medullary bone to produce bleeding and blood supply for the future grafting procedure.
Fig. 4a shows the occlusal view of the Inion barrier tucked into the lingual tissue and tacked on the distal-buccal apical aspect of the bone defect.
Fig. 4b shows the amount of bone grafting mixture under the Inion barrier. The barrier is secured on the mesial-buccal apical to minimize movement of graft material.
Fig. 5 shows the thickness of the bone grown on buccal and lingual aspects of the previous bony ridge in area.
Fig. 6 shows placement of a 3.7 mm Zimmer implant in the 10 mm wide new bony receptor site.
Fig. 7 shows suture closure of the maxillary cuspid area.
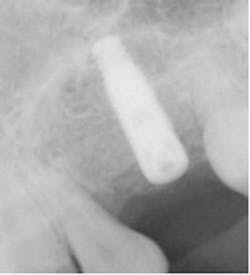
Fig. 8 shows an X-ray of 3.7 mm implant placement.
Drs. Alfred L. and Robert Heller do not have any financial interest in the products or companies mentioned in this article. They have directed the Midwest Implant Institute in Columbus, Ohio, since 1980, a teaching facility for specialists and generalists wanting to learn the art of dental implant surgery and implant prosthetics. Training facilities allow for training doctors to obtain an out-of-state Ohio dental license to perform surgery on their own patients during training. Visit www.midwestimplantinstitute.org to learn about available training. Both doctors may be reached at (614) 885-1215 with questions.
Drs. Alfred L. and Robert Heller do not have any financial interest in the products or companies mentioned in this article. They have directed the Midwest Implant Institute in Columbus, Ohio, since 1980, a teaching facility for specialists and generalists wanting to learn the art of dental implant surgery and implant prosthetics. Training facilities allow for training doctors to obtain an out-of-state Ohio dental license to perform surgery on their own patients during training. Visit www.midwestimplantinstitute.org to learn about available training. Both doctors may be reached at (614) 885-1215 with questions.
Dr. Alfred “Duke” Heller, founder and director of the Midwest Implant Institute, limits his practice to the placement of dental implants, and has placed more than 20,000 implants since 1969. He received both his DDS (1962) and MS (1974) from the Ohio State University College of Dentistry. He is a fellow of the American Academy of Implant Dentistry, board certified in oral implantology, and a past president of the American Board of Oral Implantology. Dr. Heller has taught in eight dental schools teaching hands-on surgical courses where doctors place implants under his supervision.
Dr. Robert Heller is a graduate of Ohio Wesleyan University and the Ohio State University College of Dentistry (1988). He completed a prosthetic residency at Medical College of Virginia (1990) and a hospital implant residency at Loma Linda Dental School (1997). He served as president of the Ohio Section of the American College of Prosthodontics and chairman for the Ohio Dental Association’s Sub-council on Young Dentists. Dr. “Rob” has been a teaching faculty member of the Midwest Implant Institute since 1995 and director of the prosthetic arm of Midwest Implant Institute.