Oral health-care professionals can assist patients during cancer treatment
By Maria Perno Goldie, RDH, MS
As October is Breast Cancer Awareness Month, I thought I would review some resources for oral care of the cancer patient. With more than 1.4 million new cases of cancer diagnosed each year and a shift to outpatient management, you will probably see some of these patients in your practice. Because cancer treatment can affect the oral tissues, it is important to know about potential oral side effects. Preexisting or untreated oral disease can also complicate cancer treatment. Your role in patient management can extend benefits beyond the oral cavity.(1)
As October is Breast Cancer Awareness Month, I thought I would review some resources for oral care of the cancer patient. With more than 1.4 million new cases of cancer diagnosed each year and a shift to outpatient management, you will probably see some of these patients in your practice. Because cancer treatment can affect the oral tissues, it is important to know about potential oral side effects. Preexisting or untreated oral disease can also complicate cancer treatment. Your role in patient management can extend benefits beyond the oral cavity.(1)
One resource is Oral Complications of Chemotherapy and Head/Neck Radiation by the National Cancer Institute (NCI) of the National Institutes of Health (NIH). There is a patient version, a professional version, and a Spanish version.(2)
It includes An Overview; Etiopathogenesis; Oral and Dental Management Before Cancer Therapy; Oral and Dental Management After Cancer Therapy; Oral Mucositis; Orofacial Pain in Cancer Patients; Infection; Hemorrhage; Neurotoxicity; Graft-versus-Host Disease; Posttransplantation Dental Treatment; Relapse and Second Malignancy; Dysgeusia; Oral Toxicities Not Related to Chemotherapy or Radiation Therapy; Head/Neck Radiation Patients; Late Complications of Head and Neck Radiation; Conditions Affected By Both Chemotherapy and Head/Neck Radiation; Psychosocial Issues; and Special Considerations in Pediatric Populations. It was last updated July 11, 2011. Free publications are available for downloading. They are listed according to A Type of Cancer, Cancer Topics, Audience (such as Professional), and Format.(3) One such publication is Chemotherapy and You.(4)
Aggressive treatment of malignant disease may produce unavoidable toxicities to normal cells. The mucosal lining of the gastrointestinal tract, including the oral mucosa, is a major target for treatment-related toxicity by virtue of its rapid rate of cell turnover. The oral cavity is highly susceptible to direct and indirect toxic effects of cancer chemotherapy and ionizing radiation.(5) This risk results from multiple factors, including high rates of cellular turnover for the lining mucosa, a diverse and complex microflora, and trauma to oral tissues during normal oral function.(6) A patient handout is available through the American Dental Association.(7) It is critical that a multidisciplinary approach be used to manage the oral effects of the cancer patient before, during, and after cancer treatment. A multidisciplinary approach is necessary because the medical complexity of these patients affects dental treatment planning, prioritization, and timing of dental care. Some cancer conditions, such as high-dose head-and-neck radiation, are often lifelong problems, and risks for serious complications such as osteoradionecrosis of the mandible must be managed. A multidisciplinary oncology team that includes oncologists, oncology nurses, and dental generalists and specialists as well as dental hygienists, social workers, dieticians, and related health professionals can often achieve highly effective preventive and therapeutic outcomes relative to oral complications in these patients.While treatment for cancer in terms of chemotherapy and radiation therapy have evolved significantly since their beginning, both of these cancer treatment modalities have the potential to result in painful and debilitating adverse effects. These effects can decrease quality of life and, potentially, increase mortality due to cancer. This is true especially if treatments are used in combination, such as with head and neck cancers. One study discusses the prevalence and etiology of three broad categories of oral complications found during the treatment of cancer patients: mucositis, dysgeusia, and infectious disease.(8) The authors present therapeutic options that may be helpful in ameliorating these uncomfortable and, sometimes, life-threatening oral complications. A conclusion of a Cochrane Review states that chemotherapy, in addition to radiotherapy and surgery, is associated with improved overall survival in patients with oral cavity and oropharyngeal cancers.(9) Induction chemotherapy may prolong survival by 8 to 20% and adjuvant concomitant chemoradiotherapy may prolong survival by up to 16%. In patients with unresectable tumors, concomitant or alternating chemoradiotherapy may prolong survival by 10 to 22%. There is insufficient evidence as to which agent or regimen is most effective and the additional toxicity associated with chemotherapy given in addition to radiotherapy and/or surgery cannot be quantified.(9)
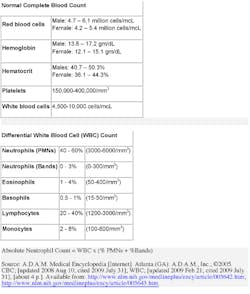
Oral cancer is usually detected earlier and treated with surgery and radiotherapy.(9) Oropharyngeal cancer is often advanced when detected and is treated with radiotherapy. Both treatments may be associated with disfigurement and decreased ability to eat, drink and talk. Treatment with chemotherapy (drugs which kill cancer cells), in addition to radiotherapy (and surgery where possible) offers prolonged survival. Chemotherapy given at the same time as radiotherapy is more effective than chemotherapy given before radiotherapy, and may reduce the need for surgery. The improvement in overall survival with the use of chemotherapy is estimated to be between 8% and 22%. The additional side effects of combined chemoradiotherapy (nausea, vomiting, diarrhea, hair loss, and infections) were not measured.(9) In summary, there are a multitude of resources at your disposal. Be sure to ask about levels of red and white blood cells, and platelets. If the patient is receiving chemotherapy, have the oncology team conduct blood work 24 hours before dental treatment to determine whether the patient’s platelet count, clotting factors, and absolute neutrophil count are sufficient to recommend oral treatment. Postpone oral surgery or other oral invasive procedures if: platelet count is less than 75,000/mm or abnormal clotting factors are present; or absolute neutrophil count is less than 1,000/mm, or consider prophylactic antibiotics.(10) Evaluate need for antibiotic prophylaxis. If the patient has a central venous catheter, consult the oncologist to determine if antibiotics are needed before any dental treatment to prevent endocarditis.(11)
Oral health care professionals can assist patients during treatment for cancer in maintaining oral, systemic and nutritional health, as well as in controlling oral symptoms. Recovery from the acute toxicities of therapy often requires diet modification, tube feeding or both to meet patients’ energy and nutrient demands.(12) The clinical implications are that effective management of oral complications of therapy for cancer is necessary to facilitate oral intake throughout treatment. Oral health care professionals should be part of the multidisciplinary team helping meet the needs of patients during treatment.References
1. Oral Complications of Cancer Treatment: What the Dental Team Can Do. NIH Publication No. 09-4372. www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOral.htm. This fact sheet is part of the series, Oral Health, Cancer Care, and You: Fitting the Pieces Together, focused on managing and preventing oral complications of cancer treatment. The series was developed by the National Institute of Dental and Craniofacial Research in partnership with the National Cancer Institute, the National Institute of Nursing Research, and the Centers for Disease Control and Prevention. 2. www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/HealthProfessional. 3. cissecure.nci.nih.gov/ncipubs/home.aspx.4. www.cancer.gov/cancertopics/coping/chemotherapy-and-you.pdf.5. Lalla RV, Brennan MT, Schubert MM: Oral complications of cancer therapy. In: Yagiela JA, Dowd FJ, Johnson BS, et al., eds.: Pharmacology and Therapeutics for Dentistry. 6th ed. St. Louis, Mo: Mosby Elsevier, 2011, pp 782-98.6. Keefe DM, Schubert MM, Elting LS, et al.: Updated clinical practice guidelines for the prevention and treatment of mucositis. Cancer 109 (5): 820-31, 2007. 7. www.ada.org/sections/scienceAndResearch/pdfs/patient_16.pdf.8. Mosel DD, Bauer RL, Lynch DP, and Hwang ST. Oral complications in the treatment of cancer patients. Oral Diseases, Volume 17, Issue 6, pages 550–559, September 2011. 9. Furness S, Glenny A, Worthington H V, Pavitt S, Oliver R, Clarkson J E, Macluskey M, Chan KW, and Conway D I. Interventions for the treatment of oral cavity and oropharyngeal cancer: chemotherapy. Cochrane Database of Systematic Reviews: Reviews 2011 Issue 4 John Wiley & Sons, Ltd Chichester, UK. 2011. DOI: 10.1002/14651858.CD006386.pub3. 10. National Cancer Institute. PDQ Cancer Information Summaries. Oral Complications of Chemotherapy and Head/Neck Radiation. Online at www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/healthprofessional (Accessed 10/17/2011) or from the Cancer Information Service at 1-800-4-CANCER.11. www.americanheart.org. 12. Epstein JB and Huhmann MB. Dietary and nutritional needs of patients undergoing therapy for head and neck cancer. JADA 2011;142;1163-1167. October 2011.Additional readings
Jellema AP, Slotman BJ, Doornaert P, et al. Impact of radiation-induced xerostomia on quality of life after primary radiotherapy among patients with head and neck cancer. Int J Radiat Oncol Biol Phys 2007; 69(3): 751-60.Keefe DM, Schubert MM, Elting LS, et al. Updated clinical practice guidelines for the prevention and treatment of mucositis. Cancer 2007 Mar 1; 109(5):820-31. Online at www.mascc.org/mc/page.do. National Cancer Institute. PDQ Cancer Information Summaries. Oral Complications of Chemotherapy and Head/Neck Radiation. Online at www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/healthprofessional (Accessed October 17, 2011) or from the Cancer Information Service at 1-800-4-CANCER.Schubert MM, Appelbaum FR, Peterson DE, Lloid ME. Oral complications. In: Blume KG, Forman SJ, eds.: Thomas’ Hematopoietic Cell Transplantation. 3rd ed. Malden, Mass: Blackwell Science Inc., 2004, pp 911-28.Shiboski CH, Hodgson TA, Ship JA, Schiødt M. Management of salivary hypofunction during and after radiotherapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007; 103(suppl 1):S66.e1-S66.e19.Sonis ST, Elting LS, Keefe D, et al. Perspectives on cancer therapy-induced mucosal injury: pathogenesis, measurement, epidemiology, and consequences for patients. Cancer 2004; 100(9 Suppl):1995-2025.Publications in the Oral Health, Cancer Care, and You series
For patients
Chemotherapy and Your Mouth
La quimioterapia y la boca
Head and Neck Radiation Treatment and Your Mouth
La boca y el tratamiento de radiación en la cabeza y el cuello
Three Good Reasons to See a Dentist BEFORE Cancer Treatment
Tres buenas razones para ver a un dentista ANTES de comenzar el tratamiento contra el cáncer
Three Good Reasons to See a Dentist Before Cancer Treatment (Illustrated booklet for adults with limited reading skills)For health professionals
Dental Provider's Oncology Pocket Guide www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/ReferenceGuideforOncologyPatients.htmOral Complications of Cancer Treatment: What the Dental Team Can Dowww.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOral.htmOncology Pocket Guide to Oral Healthwww.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OncologyReferenceGuide.htmOral Complications of Cancer Treatment: What the Oncology Team Can Do www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOncology.htmOral Health in Cancer Therapy: A Guide for Health Care Professionalswww.doep.org/images/OHCT_III_FINAL.pdf
1. Oral Complications of Cancer Treatment: What the Dental Team Can Do. NIH Publication No. 09-4372. www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOral.htm. This fact sheet is part of the series, Oral Health, Cancer Care, and You: Fitting the Pieces Together, focused on managing and preventing oral complications of cancer treatment. The series was developed by the National Institute of Dental and Craniofacial Research in partnership with the National Cancer Institute, the National Institute of Nursing Research, and the Centers for Disease Control and Prevention. 2. www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/HealthProfessional. 3. cissecure.nci.nih.gov/ncipubs/home.aspx.4. www.cancer.gov/cancertopics/coping/chemotherapy-and-you.pdf.5. Lalla RV, Brennan MT, Schubert MM: Oral complications of cancer therapy. In: Yagiela JA, Dowd FJ, Johnson BS, et al., eds.: Pharmacology and Therapeutics for Dentistry. 6th ed. St. Louis, Mo: Mosby Elsevier, 2011, pp 782-98.6. Keefe DM, Schubert MM, Elting LS, et al.: Updated clinical practice guidelines for the prevention and treatment of mucositis. Cancer 109 (5): 820-31, 2007. 7. www.ada.org/sections/scienceAndResearch/pdfs/patient_16.pdf.8. Mosel DD, Bauer RL, Lynch DP, and Hwang ST. Oral complications in the treatment of cancer patients. Oral Diseases, Volume 17, Issue 6, pages 550–559, September 2011. 9. Furness S, Glenny A, Worthington H V, Pavitt S, Oliver R, Clarkson J E, Macluskey M, Chan KW, and Conway D I. Interventions for the treatment of oral cavity and oropharyngeal cancer: chemotherapy. Cochrane Database of Systematic Reviews: Reviews 2011 Issue 4 John Wiley & Sons, Ltd Chichester, UK. 2011. DOI: 10.1002/14651858.CD006386.pub3. 10. National Cancer Institute. PDQ Cancer Information Summaries. Oral Complications of Chemotherapy and Head/Neck Radiation. Online at www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/healthprofessional (Accessed 10/17/2011) or from the Cancer Information Service at 1-800-4-CANCER.11. www.americanheart.org. 12. Epstein JB and Huhmann MB. Dietary and nutritional needs of patients undergoing therapy for head and neck cancer. JADA 2011;142;1163-1167. October 2011.Additional readings
Jellema AP, Slotman BJ, Doornaert P, et al. Impact of radiation-induced xerostomia on quality of life after primary radiotherapy among patients with head and neck cancer. Int J Radiat Oncol Biol Phys 2007; 69(3): 751-60.Keefe DM, Schubert MM, Elting LS, et al. Updated clinical practice guidelines for the prevention and treatment of mucositis. Cancer 2007 Mar 1; 109(5):820-31. Online at www.mascc.org/mc/page.do. National Cancer Institute. PDQ Cancer Information Summaries. Oral Complications of Chemotherapy and Head/Neck Radiation. Online at www.cancer.gov/cancertopics/pdq/supportivecare/oralcomplications/healthprofessional (Accessed October 17, 2011) or from the Cancer Information Service at 1-800-4-CANCER.Schubert MM, Appelbaum FR, Peterson DE, Lloid ME. Oral complications. In: Blume KG, Forman SJ, eds.: Thomas’ Hematopoietic Cell Transplantation. 3rd ed. Malden, Mass: Blackwell Science Inc., 2004, pp 911-28.Shiboski CH, Hodgson TA, Ship JA, Schiødt M. Management of salivary hypofunction during and after radiotherapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007; 103(suppl 1):S66.e1-S66.e19.Sonis ST, Elting LS, Keefe D, et al. Perspectives on cancer therapy-induced mucosal injury: pathogenesis, measurement, epidemiology, and consequences for patients. Cancer 2004; 100(9 Suppl):1995-2025.Publications in the Oral Health, Cancer Care, and You series
For patients
Chemotherapy and Your Mouth
La quimioterapia y la boca
Head and Neck Radiation Treatment and Your Mouth
La boca y el tratamiento de radiación en la cabeza y el cuello
Three Good Reasons to See a Dentist BEFORE Cancer Treatment
Tres buenas razones para ver a un dentista ANTES de comenzar el tratamiento contra el cáncer
Three Good Reasons to See a Dentist Before Cancer Treatment (Illustrated booklet for adults with limited reading skills)For health professionals
Dental Provider's Oncology Pocket Guide www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/ReferenceGuideforOncologyPatients.htmOral Complications of Cancer Treatment: What the Dental Team Can Dowww.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOral.htmOncology Pocket Guide to Oral Healthwww.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OncologyReferenceGuide.htmOral Complications of Cancer Treatment: What the Oncology Team Can Do www.nidcr.nih.gov/OralHealth/Topics/CancerTreatment/OralComplicationsCancerOncology.htmOral Health in Cancer Therapy: A Guide for Health Care Professionalswww.doep.org/images/OHCT_III_FINAL.pdf
Maria Perno Goldie, RDH, MS
To read previous articles in RDH eVillage FOCUS from 2011 written by Maria Perno Goldie, go to articles.