Osteoporosis: Risk factors, diagnostic tools, and effects on oral health
As a clinical dental hygienist my goal has been helping to preserve and maintain bone. So, when I was diagnosed with osteoporosis, I couldn’t help but do a deep-dive into the research and prevention for this destructive, debilitating disease to learn more about it. What I found both shocked and motivated me to advocate for early detection.
What you may not know about osteoporosis
The Centers for Disease Control and Prevention states: “Osteoporosis is the most common bone disease and is characterized by weakening of bone tissue, bone structure, and strength, and may lead to increased risk of fractures. Low bone mass increases the risk of developing osteoporosis.”1 Osteoporosis is the most chronic metabolic bone disease and correlates with other chronic inflammatory diseases such as lupus, diabetes, irritable bowel syndrome, celiac disease, and rheumatoid arthritis, to name a few.2 Osteoporosis also has links to genetics, lifestyle choices, and environmental pollutants that may make a person more at risk for developing the disease.2
Osteoporosis is being called the “silent killer.” This statement is especially true for women. The disease is four times more likely to be found in women than men and is more common in Asian or Non-Hispanic White women.3 Women experience a faster rate of bone loss, and they can develop osteoporosis at a younger age.3 Some studies have linked this to a reduction in estrogen levels, which is common in postmenopausal and even some perimenopausal women.3 Hormones play a critical role in bone health. Lowered sex hormones (in both males and females) can lead to bone degeneration and eventually to bone loss.3
More about osteoporosis … Medical History Mysteries: Osteoporosis and dental treatment—bisphosphonates
Osteoporosis isn’t age-dependent
Unfortunately, osteoporosis has been characterized as a disease of the aging population. However, there are speculations that even more people have early signs of this silent disease but are unaware. They simply are not being screened for osteoporosis early enough. If someone does not fit the guidelines for screening, sadly they may receive an osteoporosis diagnosis only after a life-altering bone fracture.
For years, the guidelines for osteoporosis screening were aimed at 65-year-olds or older postmenopausal women—with no recommendation for men due to their lower risk for the disease.4 The good news is that the US Preventive Services Task Force has come out with new recommendations for the screening and diagnosis of osteoporosis. Their recommendation includes screening younger patients who are at an increased risk for osteoporosis, determined by a risk assessment tool.4 Learn more about FRAX, a fracture risk assessment tool.
These newer screening guidelines will hopefully help reduce the current staggering statistics:
- About 50% of women over age 50 will have a fracture of the spine, hip, or wrist in their lifetime.5
- The most common area for these fractures is the spine.5
- This means that one in every two women will need help with early detection to enable early intervention and treatments.
Risk factors for osteoporosis
Knowing the common risk factors for osteoporosis can help with early detection. Risk factors include:
- Smoking
- Family history of osteoporosis
- Low estrogen levels (women) and low testosterone levels (men)
- Small frame or thin bones
- Menopause
- Sedentary lifestyle
- Lack of protein, vitamin D, and calcium in the diet
- Long-term steroid use
- Heavy alcohol consumption
- Advancing age
- Side effects of some medications3
How osteoporosis affects oral health
In dentistry, we see many of these same risk factors playing a part in our patients’ oral health and healing. It comes as no surprise that studies are reporting a link between osteoporosis and periodontal disease showing horizontal alveolar bone loss.6 With shared risk factors and inflammation, patients with osteoporosis may have more periodontal disease.6 Consequently, dental professionals have a vested interest in early detection to fight osteoporosis and help preserve bone health throughout the entire body.
So, how can dental professionals help with early detection? It could be as easy as looking under your patient’s nose at their jaw.
You may also be interested in … Inflammation: A major link between oral and systemic diseases
Diagnostic methods for dental professionals
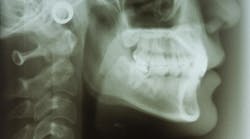
I have been a clinical hygienist for 30 years. A few years after graduating from hygiene school, an article was published stating that panoramic x-rays could be helpful screening tools for strokes and osteoporosis. In hindsight, this was groundbreaking news. Unfortunately, since 1996, using panoramic radiographs as screening tools for osteoporosis has not been widely used.
More recent research shows panoramic radiographs—along with current technology—can provide more precise screening of jaw degeneration and possible evidence of osteoporosis. A general radiologist, Oksana Bandura, MD, wrote an informative article for DentistryIQ called, “How new dental imaging can save the lives of your patients.” This article is a great reference to help dental professionals understand how to use panoramic and computer-aided diagnosis (CAD) as screening tools.7 More recent content discusses how cone-beam computed tomography (CBCT) could play a pivotal role in screening for osteoporosis.8 This is especially important for implant placement and the long-term success of implants.
Panoramic radiographs are inexpensive (covered by most insurances), safe (emitting low radiation), and accessible to the general public. A high percentage of patients may have panoramic x-ray images in their patient files already. Unfortunately, panoramic radiographs are underutilized as screening tools for systemic bone loss. Early detection is critical for patient referrals to a primary care physician for further assessment, diagnosis, and early treatment.
Patient education is key
I love educating dental professionals on current preventive health strategies to help improve the lives of patients. Dental professionals can help by seeking more education and knowledge on using dental radiographs as screening tools for systemic health conditions. We can utilize current technology, such as artificial intelligence and CBCT, to better serve our patients. Identifying patients at higher risk for osteoporosis allows us to make referrals to their PCP for further screening. By doing these things, dental professionals can assist patients in assessing their risk, getting an early diagnosis, and ultimately improving their future health outcomes.
Editor’s note: This article first appeared in Through the Loupes newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles and subscribe to Through the Loupes.
References
- Sarafrazi N, Wambogo EA, Shepherd JA. Osteoporosis or low bone mass in older adults: United States, 2017–2018. NCHS Data Brief, No. 405. Centers for Disease Control and Prevention. National Center for Health Statistics. Updated March 31, 2021. https://www.cdc.gov/nchs/products/databriefs/db405.htm
- Adami G, Fassio A, Gatti D, et al. Osteoporosis in 10 years time: a glimpse into the future of osteoporosis. Ther Adv Musculoskelet Dis. 2022;14:1759720X221083541. doi:10.1177/1759720X221083541
- Bailey A. Osteoporosis facts and statistics: what you need to know. Verywell Health. October 11, 2022. Accessed September 2023. https://www.verywellhealth.com/osteoporosis-facts-5323575
- US Preventive Services Task Force; Curry SJ, Krist AH, Owens DK, et al. Screening for osteoporosis to prevent fractures: US Preventive Services Task Force Recommendation Statement. JAMA. 2018;319(24):2521-2531. doi:10.1001/jama.2018.7498
- Osteoporosis. MedlinePlus. Updated January 25, 2023. Accessed September 2023. https://medlineplus.gov/ency/article/000360.htm
- Yeung AWK, Mozos I. The innovative and sustainable use of dental panoramic radiographs for the detection of osteoporosis. Int J Environ Res Public Health. 2020;17(7):2449. doi:10.3390/ijerph17072449
- Bandura O. How new dental imaging can save the lives of your patients. DentistryIQ. October 3, 2017. Accessed September 2023. https://www.dentistryiq.com/dentistry/article/16366176/how-new-dental-imaging-can-save-the-lives-of-your-patients
- de Castro JGK, Carvalho BF, de Melo NS, et al. A new cone-beam computed tomography-driven index for osteoporosis prediction. Clin Oral Investig. 2020;24(9):3193-3202. doi:10.1007/s00784-019-03193-4
Kristin Evans, BS, RDH, has been a clinical dental hygienist for more than 30 years. Her work as a professional educator, national speaker, and writer has elevated her love for helping both dental professionals and patients succeed. Kristin’s goal is to change lives with simple strategies and powerful education by bridging the gap between mental, physical, and oral health. Contact her at [email protected] or follow her on social media @kristinevansrdh.
About the Author

Kristin Evans, BS, RDH
Kristin Evans, BS, RDH, is a dental hygienist and educator with 30-plus years of experience. She became a national speaker in 2022 with a focus on hormones, bone health, nutrition, and the oral-systemic connection. Known as “The pH RDH,” she is a published author with a mission to inspire and empower dental professionals with practical strategies and knowledge bridging the gap between oral, mental, and physical health. Contact her for speaking inquiries at [email protected] or follow her on Instagram @ThepHRDH.