Achieving Stable Occlusion Prior to Esthetic Restoration... an Orthodontic Approach
Introduction ~
Many times, orthodontically moving the teeth prior to restorative care will result in a more stable, functional occlusion and decrease the amount of restorative dentistry needed to reach that goal. Achieving a stable occlusion prior to esthetic restoration improves the predictability of the restoration by optimizing its function and longevity. Dr. Harry Aronowitz states that the goal of orthodontics should be the same as restorative dentistry, which is to establish a functional occlusion.1 Orthodontics makes it possible to move the teeth into functional occlusion instead of placing multiple restorations to achieve the same goal. Two complex cases are presented here utilizing orthodontics prior to restoration. In both cases, a stable occlusion was attained orthodontically with the aid of equilibration post-treatment. Fewer restorations were required to give an esthetic result after moving the teeth.
Case One
(Figures 1 through 7)
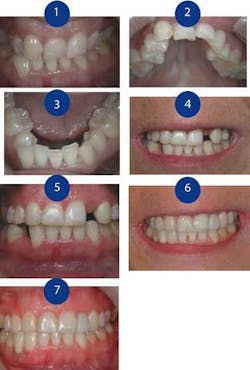
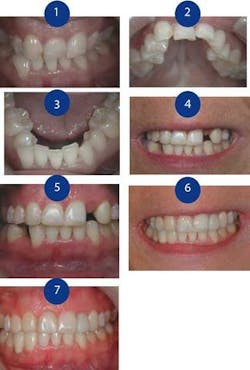
Figure 1: Anterior view prior to treatment
Figure 2: Maxillary occlusal view
Figure 3: Mandibular occlusal view
Figure 4: Prerestorative anterior view after orthodontics
Figure 5: Retracted prerestorative anterior view after orthodontics
Figure 6: After restoration, six months prior to final ceramic restoration of No. 27
Figure 7: Retracted restoration, six months prior to final ceramic restoration of No. 27
Patient history - A 34-year-old female expressed a desire to improve her smile. As a child, she had had cleft palate surgery and orthodontic treatment. A comprehensive oral health evaluation revealed the following conditions: She had Class II dental and skeletal malocclusion. Her midline was shifted to her left 6 mm. A total of eight teeth were congenitally missing (Nos. 1, 7, 10, 12, 16, 21, 27, and 29). Her incisors and left cuspid were moderately worn. She had a limited opening of 22 mm. Because of the appearance of her teeth, she was reluctant to smile. She had learned how to posture her lips to hide her teeth when she spoke.
Treatment options - The patient clearly stated that she did not want orthognathic surgery. Having had multiple palatal surgeries in childhood, she felt she had had “enough.” Therefore, combined orthodontics and orthognathic surgery was not an appropriate option for her. Other, more acceptable treatment options included splint therapy, orthodontic treatment to open space for missing Nos. 10 and 27, and implant-retained crowns for missing Nos. 10 and 27.
Treatment sequence - The first phase of treatment consisted of removal of No. 17, then occlusal splint therapy to make the patient more comfortable and improve joint health and function. Treatment called for the patient to wear a Tanner mandibular occlusal appliance2 24 hours a day except while eating. A cuspid-protected, anterior-guided occlusion was established on the appliance.3 A maxillary removable Schwartz appliance was used to begin palatal expansion. The patient was seen every two weeks to adjust the mandibular appliance. The patient reported being comfortable when wearing the appliances and was extremely compliant in order to maintain that comfort. This initial phase of treatment lasted three months. Because this was going to be a challenging orthodontic case, patient compliance would be a key part of successful treatment.
The next phase was orthodontic treatment. Because three of the eight bicuspids were missing, No. 5 was positioned in the area of No. 6. No. 6 was reshaped and its mesial surface bonded to mimic No. 7. The space for No. 10 was opened using a palatal expander bonded to the posterior teeth to expand the arch and coil springs to open the space. The space for No. 27 was opened using coil springs. Orthodontic treatment time was 16 months. Hawley appliances with temporary prostheses were used to retain the created spaces.
After orthodontic treatment, the patient’s teeth were whitened at home using bleaching trays. Restorative treatment was begun approximately five months after the removal of the patient’s braces. Equilibration was performed using the guidelines set by Pankey-Mann-Schuyler:4,5
• When both condyles are seated in the fossa, you have simultaneous, equal pressure on all the teeth.
• When you squeeze hard, there is no deviation of the mandible or any tooth.
• When you move the mandible in any excursion, no back tooth hits before, harder than, or after a front tooth.
Because No. 27 was going to be restored with an implant, lateral guidance went from No. 28 first, then to cuspid, then to central in the cross-over position.
Due to the root proximity of Nos. 9 and 11, an implant could not be placed for No. 10. A fiber-reinforced, bonded bridge with a porcelain veneer was used in place of an implant. An implant was successfully placed in the area of No. 27. Orthodontic treatment prior to restorative treatment positioned teeth for functional occlusion and regained space for congenitally missing Teeth Nos. 10 and 27. Future treatment will consist of veneering No. 5 (in the position of No. 6) and Nos. 7 through 9 to create more esthetic contours. Due to the complexity of the case, orthodontic treatment lasted 14 months for the maxillary arch and 16 months for the mandibular arch.
Case Two
(Figures 8 through 13)
Figure 8: Anterior view prior to treatment
Figure 9: Retracted anterior view prior to treatment
Figure 10: Prerestorative view of Nos. 7 through 10 after nine months of orthodontics
Figure 11: Retracted prerestorative view of Nos. 7 through 10
Figure 12: Smile after restoration, 22 months after orthodontic treatment
Figure 13: Retracted anterior view with veneers, 22 months after orthodontic treatment
Patient history - A 50-year-old female was bothered by the unnatural appearance of her mouth due to congenitally missing maxillary laterals that had been replaced by rotated cuspids. She had been referred to Dr. Kevin Murphy, a perio-prosthodontist, for a smile makeover and wanted to know if her goals could be met by placing veneers on the front of her teeth. The perio-prosthodontist referred her to me for an orthodontic evaluation preliminary to restoration.
She had had no prior history of orthodontic care. Due to the need for connective tissue grafts and the patient’s request for the shortest time of treatment, the perio-prosthodontist suggested we work together and perform orthodontic care combined with “Wilckodontics,” also known as Accelerated Osteogenic Orthodontics (AOO). Upon performing a comprehensive oral health evaluation, the following additional findings came to light: She suffered from Class II malocclusion. Heavy clenching had resulted in moderate to severe abfractions on the cuspids through first molars. She suffered from minimal gingival attachment and moderate to severe recession.
Treatment options - The patient was presented with three orthodontic options. The first plan called for opening the lateral space and repositioning the cuspids into Class I occlusion, then placing implants in the areas of the missing lateral incisors. The estimated time for orthodontic treatment for this plan was 24 to 28 months. Total time for periodontal grafts, orthodontic treatment, and restorative treatment was 30 to 36 months.
The second plan called for orthodontically moving and rotating the teeth, leaving the cuspid in the lateral space. This would create a close-to-ideal Class I occlusion, and the cuspids could be veneered to look like lateral incisors. The estimated treatment time for this plan was 22 to 24 months.
The third option was to combine the patient’s need for orthodontics and connective tissue grafts using Wilckodontics or AOO surgery.5 We could combine bone grafts, connective tissue grafts, and orthodontics to achieve the result we wanted in eight to 10 months. We would keep the cuspids in the lateral position and veneer them during post-orthodontic treatment. The teeth would be moved to Class I occlusion after which we would perform a post-orthodontic, full-mouth equilibration. The teeth would be whitened and restored with veneers on Nos. 6 and 11 in place of Nos. 7 and 10. We would recontour Nos. 5 and 12 to resemble Nos. 6 and 11. Class V composite would be used to restore areas of abfractions.
The patient elected the AOO surgery option. She did not want to reposition the cuspids and open the space for the laterals due to the additional time involved and the cost of the implants, abutments, and crowns needed to replace Nos. 7 and 10. Because she needed connective tissue grafts prior to the orthodontics, it made sense to have the AOO surgery performed at the same time.
Treatment sequence - Because porcelain brackets would be less noticeable on lighter teeth, treatment began with the patient whitening her teeth at home using bleaching trays. Bands were placed on four second molars. The perio-prosthodontist performed the AOO surgery and added connective tissue grafts in the areas of Nos. 4 through 6 and 11 through 13. Ten days after surgery, porcelain brackets were bonded to her teeth and orthodontic movement began.
Once Wilckodontics is underway, it is imperative that the patient be seen every two weeks during orthodontic treatment. A 16 x 22 NITI wire was placed after four weeks of movement and used in both arches during the majority of treatment.6 The accelerated movement happens over the first four to five months. After this time, traditional orthodontic movement occurs. The patient’s orthodontic treatment was completed in nine months. Three months into this treatment, the cuspids were reshaped and the mesial aspects of the teeth were bonded to look like lateral incisors.
After the orthodontic bands and brackets were removed, the patient was instructed to use an Essex retainer during the day and a Hawley appliance during the night. Class V composite was applied in all areas of abfractions. The patient’s teeth were then rewhitened at home. Five months into the retention phase, a full-mouth equilibration was performed and the perio-prosthodontist placed veneers on the cuspids to make them look like lateral incisors.
Photographs with veneers were taken 22 months after orthodontic treatment. The occlusion was functional and stable, and the attachment levels were greatly increased by the placement of connective tissue grafts at the time of the AOO surgery. The surgical technique combining selective partial decortication of the cortical plate, concomitant bone grafting/augmentation, connective tissue grafts, and primary flap closure allowed for rapid orthodontic tooth movement. The total orthodontic treatment time was nine months.
Summary
Many times, orthodontically moving the teeth prior to restorative care will result in a more stable occlusion and decrease the amount of restorative dentistry needed to establish both a functional occlusion and the desired esthetic results. The previous two case studies have illustrated this point. In Case 1, occlusion was stabilized and the esthetic objectives were achieved without orthognathic surgery. In Case 2, the patient’s occlusion was significantly improved and stabilized, and the esthetic objectives were achieved without orthognathic surgery or implants. Veneers were kept to a minimum in Case 2.
References
1 Aronowitz H. Orthodontics and occlusion: a historical perspective. J Calif Dent Assoc. Oct. 1996; 24(10):16-18.
2 Tanner HM. The Tanner mandibular appliance. J Colo Dent Assoc 1996; 75(2):14-18.
3 Williamson EH, Ludquist DO. Anterior guidance: Its effect on EMG activity on the temporal and masseter muscles. J Prosthet Dent 1983; 49:816-822.
4 Schuyler CH. Correction of occlusal disharmony of natural teeth. NY Dent J 1947; 13:445.
5 Mann AW, Pankey LD. The PM oral rehabilitation. J Prosthet Dent 1960; 10:135-162.
6 Wilcko T, Bouquot JE, Ferguson DJ, Wilcko UM. Rapid orthodontics with alveolar reshaping: Two case reports of decrowding. Internat J Perio & Restor Dent 2001; 21(1):9-19.
Nancy A. Ward, DDS, MAGD
Dr. Ward practices with her husband in Baltimore, Md. She is a visiting faculty member and a board member of The Pankey Institute. She is a past president of both the Baltimore and Maryland Academy of General Dentistry. Contact Dr. Ward at wardbyrne@ aol.com.