Minimal Intervention Dentistry
Incorporating Recaldent amorphous calcium phosphate products can help fight caries in high-risk patients.
In the new millennium, there is an ever-increasing range of products available to assist us with the management of oral diseases. We have all had those challenging patients in whom the use of fluoride alone has not controlled their dental caries. For these patients, the new group of amorphous calcium phosphate products are helpful, especially when combined with fluorides, saliva substitutes, stimulants, and antimicrobials using the philosophy of minimal intervention dentistry.
What is MID?
MID uses a medical model for oral disease control and comprises:
- oral disease risk assessment with early detection and prevention;
- external and internal remineralization therapy;
- use of a range of restorations, dental materials, and equipment; and
- surgical intervention only after disease is controlled.1-3
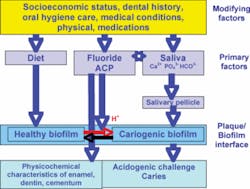
In essence, MID is a tool to help us understand and manage oral disease so that we increase the longevity of our restorations. For the management of dental caries in MID, the assessment and management of a diverse group of patient-modifying factors and primary factors is integrated with an evaluation of the plaque/biofilm interface and the resultant dynamic oral disease process (see Fig. 1).4 Such assessments can utilize tools such as Ngo’s Traffic Light system and CAMBRA.4,5 Within the mouth of an adult who has active and even rampant caries, there will be a range of low to high areas of demineralization and caries (with and without cavitation). Demineralization and remineralization are continuous, thus it is essential to assess the clinical pattern of demineralization and caries in the context of all modifying, primary, and biofilm factors.
Fluorides
Fluoride is the cornerstone of modern preventive dentistry:
- it increases enamel resistance to acid attack and remineralization via formation of fluoride enriched apatite;
- it inhibits demineralization; and
- at high concentrations inhibits bacterial metabolism.6
Frequent fluoride exposures achieve optimal low-level loading of the salivary fluoride reservoir.
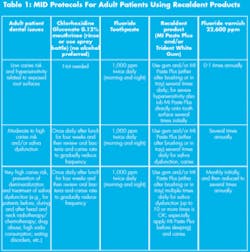
Traditionally, adults with low-caries risk have used 1,000 ppm toothpaste, which had been supplemented or replaced as caries risk increased with a 5,000 ppm prescribed toothpaste or gel. In recent years, the use of sodium fluoride mouthrinses has decreased with the introduction of the 5,000 ppm toothpastes. The use of fluoride foams (placed in trays) at 12,300 ppm, has also decreased with greater use of 22,600 ppm (5 percent) fluoride varnishes.
Recaldent: Casein Phosphopeptide-Amorphous Calcium Phosphate (CPP-ACP)
Although the use of topical fluorides has resulted in decreased coronal and root caries experience in many adults and older adults, there are patients who experience high caries rates despite use of fluoride.6 For these patients, we have sometimes used additional adjunctive therapies for saliva dysfunction and chemoprophylactics such as chlorhexidine.
Recently, an improved understanding of the oral biofilm and the continuum of remineralization/demineralization has developed sophisticated carriers for calcium and phosphate, such as the casein protein molecule (CPP-ACP) (Recaldent (Bonlac Bioscience International Pty Ltd, Australia)) and bioactive glasses (NovaMin, NovaMin Technology, Inc, Alachua, Fla.). These products have improved upon delivery problems with earlier amorphous calcium phosphate products such as Enamelon (ADA Foundation ACP).9 NovaMin is a sodium calcium phosphosilicate glass that releases calcium and phosphate ions in water and/or saliva. Exposed dentin acts as a nucleation site for these ions to form a hydroxycarbonate apatite.10
The Recaldent casein protein molecule carrier for amorphous calcium phosphate (CPP-ACP) has been researched for nearly 20 years and has a substantial evidence base.11 Stabilization of nanoclusters of amorphous calcium phosphate (ACP) with casein phosphopeptides (CPP) results in localization of CPP-ACP at the tooth surface by:
- binding to dental plaque (to the microorganisms and in extracellular matrix); and
- binding to exposed dentin.12
An acidic oral environment activates CPPs and buffers plaque pH to produce calcium and phosphate ions; in particular the neutral ion pair CaHPO40 is produced which is highly correlated with prevention of demineralization and enamel remineralization rate.12 Remineralization from fluoride ions alone is more superficial than that of calcium, phosphate, and fluoride ions in combination.11 CPP-ACP interacts with localized fluoride ions to produce a novel amorphous calcium fluoride phosphate phase.11
CPP-ACP was commercially developed as Recaldent, which is sold professionally as MI Paste (10 percent CPP-ACP) and the new MI Paste Plus (10 percent CPP-ACP; 900 ppm fluoride) (GC America, Alsip, Ill.), and in a consumer range of chewing gum products, Trident White with Recaldent (0.6 percent CPP-ACP) (Cadbury Adams). Due to the casein content, all potential users of Recaldent products must be asked, “Do you ever have any allergic reactions when you drink milk?” to investigate if they have an IgE mediated casein allergy.12 Recaldent products can be used by patients with lactose intolerance as they do not contain lactose.
MI Paste, MI Paste Plus, or Trident White with Recaldent Gum?
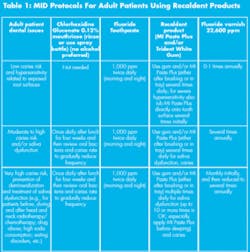
Clinical indications for Recaldent products are for:
- hypersensitivity;
- pre- and postbleaching and periodontal scaling to help reduce sensitivity;
- erosion, abrasion, reflux; and
- dry mouth (Table 1).12 Amorphous calcium phosphate products are also used off-label in clinical practice for:
- the prevention of caries and demineralization, and
- as therapies for the remineralization of dental hard tissues after a degree of demineralization/caries has occurred (e.g., around orthodontic brackets) (Table 1).12
Patients can use the MI Paste/MI Paste Plus, the gum, or both several times daily in a variety of applications. The original MI Paste has no added fluoride, and as such is safe to use by children under 6 years (who do not have a casein allergy). The new MI Paste Plus has the same components as the original MI Paste but with 900 ppm fluoride added to optimize the correct bioavailable ionic ratio of 5 calcium, 3 phosphate, and 1 fluoride ions.11 For the deepest, most thorough remineralization therapy, it is recommended to use MI Paste Plus in combination with a lower 1,000 ppm fluoride toothpaste rather than using a higher 5,000 ppm toothpaste.11 Thorough remineralization therapy may take several weeks use of Recaldent products.11 Recaldent products have been clinically useful in patients with dry mouth - the MI Paste as a saliva substitute and the Trident White with Recaldent Gum as a saliva stimulant.13
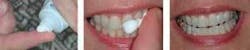
The benefit of using Recaldent products in patients with dry mouth is that their often deficient calcium, phosphate and fluoride reservoirs will be replenished with use of the products. The simplest application method is to place a ”pea-size” amount of MI Paste/MI Paste Plus on a fingertip and rub it all over teeth and soft tissues (Fig. 2).
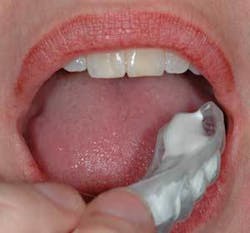
In a normal mouth, the MI Paste Plus will take some 30 seconds to a minute to dissolve, but in a dry mouth, this may take a little longer. For patients with severe hypersensitivity or who have sensitivity with bleaching, it may be helpful to do several initial applications of MI Paste Plus in a custom tray. (Note: Use one custom tray for MI Paste Plus, and a separate one for the bleaching gel) (Fig. 3).
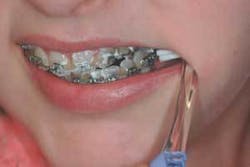
Orthodontic patients may also prefer gentle brushing of the paste onto the teeth with a soft toothbrush (Fig. 4).
Conclusion
Oral physicians, hygienists and their dental teams have the challenge to monitor the ongoing reviews of evidence for therapeutic approaches in Minimal Intervention Dentistry - for all modifying and primary factors, at the biofilm level, and for efficacious minimal combinations of therapeutic products. Recaldent and other emerging amorphous calcium phosphate products are a key component for preventing and managing new and recurrent coronal and root caries.
References
- Mount GJ, Ngo H. Minimal intervention: a new concept for operative dentistry. Quintessence Int. 2000 Sep;31(8):527-33.
- Pitts NB. Are we ready to move from operative to non-operative/preventive treatment of dental caries in clinical practice? Caries Res 2004:38(3):294-304.
- Tyas MJ, Anusavice KJ, Frencken JE, Mount GJ. Minimal Intervention Dentistry - a review. FDI Commission Project 1-97. Int Dent J 2000;50(1):1-12.
- Ngo H, Gaffney S. Chapter 6 - Risk assessment in the diagnosis and management of caries. In: Preservation and Restoration of Tooth Structure. Mount GJ and Hume WR. Knowledge Books and Software. 2005.
- Featherstone JD. The caries balance: the basis for caries management by risk assessment. Oral Health Prev Dent 2004;2 Suppl 1:259-264.
- McIntyre J. Chapter 4 - Preventive management of dental caries. In: Preservation and Restoration of Tooth Structure. Mount GJ and Hume WR. Knowledge Books and Software. 2005.
- Hicks J, Garcia-Godoy F, Donly K, Flaitz C. Fluoride-releasing restorative materials and secondary caries. J Calif Dent Assoc 2003;31(3):229-245.
- Weintraub J. Fluoride varnish for caries prevention: comparisons with other preventive agents and other recommendations for a community-based protocol. Spec Care Dent 2003;23;180-186.
- Tung MS, Eichmiller FC. Amorphous calcium phosphates for tooth mineralization. Compend Contin Educ Dent. 2004 Sep;25(9 Suppl 1):9-13.
- Marini I, Checci L, Greenspan D. Pilot clinical study evaluating efficacy of Novamin-containing dentrifice for relief of dentin hypersensitivity. Novamin Research Report. http://novamin.com Accessed 6/19/07.
- Cross KJ, Huq NL, Reynolds EC. Casein phosphopeptides in oral health - chemistry and clinical applications. Curr Pharm Des 2007;13(8):793-800.
- Reynolds EC, Walsh LJ. Chapter 8 - Additional aids to the remineralisation of tooth structure. In: Preservation and Restoration of Tooth Structure. Mount GJ and Hume WR. Knowledge Books and Software. 2005. Pages 111-118.