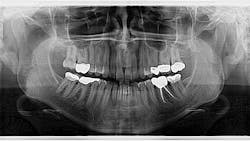
Oral pathology case: The common but not-so-common radiopacity
Case presentation and clinical assessment
A healthy 45-year-old female presents for her recare exam and an update on her panoramic radiograph. She reports no concerns or complaints.
An assessment of her pan reveals two radiopaque lesions apical to the root tips of nos. 8 and 9, measuring approximately 8 x 4 mm (figure 1). There was no tenderness on palpation in the generalized area. These lesions were noted on previous radiographs, and no changes were present.
Differentials and diagnosis
Differential considerations include supernumerary teeth, compound odontomas, false periapical radiopacities, maxillary tori, retained roots, and various anatomic structures (i.e., alae of the nose, etc.).
Using the Clark tube-shift technique, the positions of both lesions were determined to be separate from the apices of the central incisors. The definitive diagnosis was determined to be impacted supernumerary teeth, or more specifically to this area, mesiodens.
Discussion
Supernumerary teeth are teeth in excess of the normal number. When located between the maxillary central incisors, they are referred to as mesiodens. These teeth often appear near the apices of an erupted tooth, but the density, shape, and shifting of the images via the Clark tube-shift technique classifies them as false periapical radiopacities.
Supernumerary teeth most commonly occur in the maxilla (90%), with the most prevalent being the mesiodens; the most common supernumerary teeth in the mandible are the premolars.1,2 The occurrence of mesiodens in primary dentition is quite rare.2 Studies suggest that there is a genetic etiology behind the formation of mesiodens.2
The shape of these teeth can be diverse, from resembling a natural tooth to a conglomerate of dense, irregular tooth structure. They can be single (76%–86%) or multiple (12%–23%); erupted or impacted.1,2 Complications in the presence of mesiodens include delayed eruption, crowding, spacing, impaction of permanent incisors, abnormal root formation, alteration in the path of eruption of permanent incisors, median diastema, cystic lesions, intraoral infections, rotations, root resorption of the adjacent teeth, or even eruption of incisors in the nasal cavity.2
Treatment
Management of supernumerary teeth depends on the location, position, and any potential issues the tooth may be causing. Immediate removal is indicated in the following situations: inhibition or delay of eruption, displacement of the adjacent tooth, interference with orthodontic appliances, presence of pathologic condition, or spontaneous eruption of the supernumerary tooth.2 If there are no symptoms or issues, the teeth can be left as is with regular monitoring.
Editor’s note: This article first appeared in Through the Loupes newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles at this link and subscribe here.
References
- Sapp JP, Eversole LR, Wysocki GP. Contemporary Oral and Maxillofacial Pathology. Mosby; 1997:4-5.
- Meighani G, Pakdaman A. Diagnosis and management of supernumerary (mesiodens): a review of the literature. J Dent (Tehran). 2010;7(1):41-49.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].