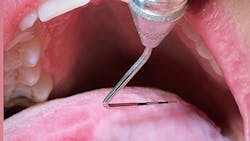
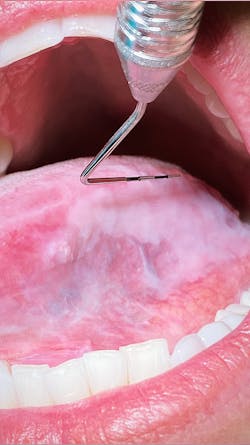
Oral pathology case: A brush with thrush...or is it?
It’s me again with another pathology case, except you get to work through this one with me, as I have a feeling it’s not unique to my practice.
An overall healthy female presented for her recall exam. As with most patients, she was pushed back for her recare due to COVID-After asking some questions, she “almost forgot to tell [me]” that back in early May (this being mid-August), she had a bout with oral thrush, which was diagnosed by a physician’s assistant at the local urgent care facility. She said it was a challenge to work through, but it finally got resolved after a few rounds of medication, to which she couldn’t remember the names.
Lately, given the trends I’m seeing in my practice regarding stress and how patients are coping with COVID-19, it’s clear that the questions begging answers are, “Did you feel you were overly stressed during this time? Did your diet change? Did your home care change? Etc.” This patient’s answer, without hesitation, was “Yes.” She, like many others, had to start working from home, she broke her wrist, had to have surgery, and financial concerns were at the forefront of her mind.
Do we see a theme here?
Backing up a bit, let’s talk about thrush. Thrush is an opportunistic fungal infection that will manifest when there is an alteration and subsequent over-growth of the fungus Candida albicans (C. albicans). Stress, hormonal imbalances, diet changes, and weakened immune systems will all have an impact on the delicate balance of flora in the mouth and other areas of the body. Thrush is commonly treated with Nystatin (as a rinse or swab), Clotrimazole (commonly prescribed as a Troche/lozenge) and Diflucan/Fluconazole (commonly prescribed as an oral medication).
Given that history, one would think that this is a residual lesion from her bout with thrush in May. But is it? Can you be certain? Lack of pain, location, and the fact that it’s getting larger don’t eliminate other possibilities, which, arguably, must be addressed.
I referred the patient for an assessment with the local oral surgeon who will likely do a biopsy. The verdict is still out. When I hear back, I’ll update you on the definitive diagnosis.
Here’s the take-home: The effects of COVID-19 on our patients’ psyches and overall health are here to stay. Our clinical assessments should include COVID-19 as a risk factor for what we are seeing manifest in dental clinical settings with increasing frequency. Upping our game regarding recognition, diagnosis, and treatment of oral lesions is more important now than ever before.
Editor’s note: This article first appeared in Through the Loupes newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles at this link and subscribe here.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].