This should be a slam dunk oral pathology case. If it’s not, read up!
Right away I asked, “Has your diet changed? Have you had changes in your medication? Drier mouth? Have you been stressed?” No, no, yes, and especially yes.
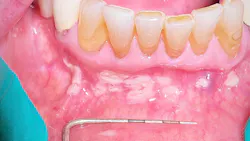
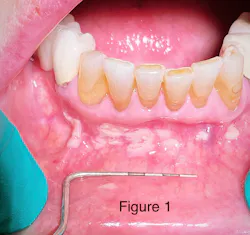
Take a look at the initial photograph. What’s the first thing that comes to your mind? Scattered, white, creamy patches in the lower anterior vestibule, each measuring approx. 3–6 mm (figure 1). Now, take a look at the second picture after the white patches were easily wiped off with gauze (figure 2). Note the red, thin membraned tissue? It was very tender to the touch.This diagnosis should be a slam dunk by now. Yup, you guessed it. Good ol’ pseudomembranous candidiasis, aka thrush.
Let’s have a refresher on thrush. See table 1. Candida albicans presents as commensals that become infective when an alteration in the immunity of the host occurs. It’s opportunistic and usually the first to take advantage of any reduction in the defense system of the host cell. Oral imbalances are common and a frequent place for these infections to occur.1 Oral clinical appearances vary; some present as white patches/lesions (some rub off, others don’t), while others appear bright red in color.
C. albicans takes on various forms, each presenting slightly differently:
- Acute pseudomembranous candidiasis consists of creamy, loose patches of desquamative epithelium that are easily removed.1 Red tissue tender to the touch is what is painful to the patient.
- Atrophic (erythematous) candidiasis presents with bright red, thinned, and smooth mucosa with burning and sensitivity; it is commonly referred to as “denture sore mouth.”1
- Chronic hyperplastic candidiasis consists of white plaques or papules against an erythematous background; it’s asymptomatic and does not rub off.1 A case presented earlier was diagnosed to be this form of thrush.
Common oral lesions associated with C. albicans include the following:
- Angular cheilitis (perleche) occurs when the bilateral fissures of the mouth are overclosed and subsequently become infected; common with loss of dentition and denture wearers.1
- Median rhomboid glossitis is an asymptomatic, elongated, erythematous patch of atrophic mucosa of the middorsal surface of the tongue due to a candidiasis infection; this is common in smokers and denture wearers.1
With all C. albicans infections, treatment is nystatin (as a rinse or swab), clotrimazole (commonly prescribed as a troche/lozenge), and Diflucan (fluconazole; commonly prescribed as an oral medication). Magic mouthwash, in cases where pain in present, helps manage the symptoms until the lesions are healed. (Recipe: one part viscous 2% lidocaine, one part Maalox, and one part diphenhydramine 12.5 mg/5 ml. Dosage: 1–2 tsp. 2–3x/day prn. I usually give 1–2 refills with a 150 ml bottle.)
With this particular patient, it was advised that she try to reduce her stress. Dry mouth management modalities were also discussed. Additionally, scripts for Magic mouthwash and troche lozenges were dispensed.
Editor’s note: This article first appeared in Through the Loupes newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles at this link and subscribe here.
Reference
- Sapp JP, Eversole LR, Wysocki GP. Contemporary Oral and Maxillofacial Pathology. Mosby; 1997:4-5.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].