Pathology case: If it's leukoplakic, follow up
Editor's note: Originally published February 2, 2016. Updated June 2023.
A 62-year-old female presents for her biannual cleaning and checkup. Health history is noncontributory; she is taking vitamin D supplements and reports no other changes or concerns.
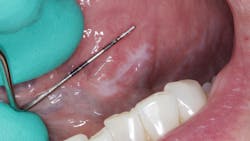
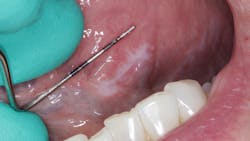
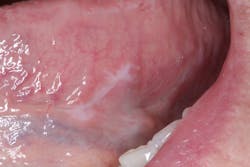
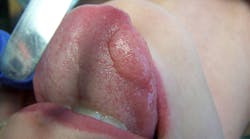
During her routine oral screening and exam, a 9 mm x 3 mm white leukoplakic patch of tissue on the left ventral surface of the tongue was noted. It was not tender to palpation, could not be scraped off, and the patient was unaware of its presence. It was recommended that the patient come back in two to three weeks to assess for continued presence.
Here are the differentials, my diagnosis, and the recommended treatment for this case ...
Differentials:
- Lichen planus/lichenoid dysplasia
- Squamous cell carcinoma (SCC)
The patient was referred to an oral surgeon where evaluation and an excisional biopsy were performed.
Definitive diagnosis: Keratosis with lichenoid chronic inflammation
The presence of leukoplakic lesions in the oral cavity is always cause for evaluation and follow-up. The World Health Organization defines leukoplakia as “a white patch or plaque that cannot be characterized clinically or pathologically as any other disease.”1 Leukoplakic lesions are one of the more common forms of epithelial dysplasia, typically discovered during routine exams; they are usually asymptomatic and represent 6.2% of all oral biopsy specimens.1 Leukoplakia and squamous cell carcinoma share many of the same etiology factors,1 and approximately 5.4% of leukoplakic lesions become SCC.2 It is, therefore, imperative that the following steps be considered:1
- Assess etiologic factors (table 1)
- Categorize the lesion as a high- or low-risk specimen (table 2)
- Assess differentials (table 3)
- Biopsy lesion (if warranted) for a definitive diagnosis
Table 1: Etiologic factors of leukoplakia
- Tobacco products
- Ethanol
- Hot, cold, spicy, and acidic foods and beverages
- Alcoholic mouth rinse
- Occlusal trauma
- Sharp edges of prosthesis or teeth
- Actinic radiation
- Syphilis
- Presence of Candida albicans
- Presence of viruses
Table 2: High-risk leukoplakias
- Red component
- Raised component
- Presence in high-risk oval
- Tobacco and alcohol use
- Nonsmoker and unknown etiology of lesion
- Nonreversible type
- Microscopic atypia
Table 3: Differential diagnosis of homogeneous leukoplakia
- Lichen planus
- Leukoedema
- Cheek-biting lesion
- Smokeless tobacco lesion
- Lupus erythematosus
- Hyperplastic or hypertrophic candidiasis
- Hairy leukoplakia
- Electrogalvanic or mercury contact allergy
- Verrucous or squamous cell carcinoma
- Verruca vulgaris
- White sponge nevus
In this particular case, the patient was a nonsmoker, and the etiology of the lesion was unknown; this alone put her in a high-risk category.
The diagnosis of lichenoid chronic inflammation is a form of “epithelial dysplasia with an associated dense infiltrate of lymphocytes that bears a striking resemblance to the dermatologic/mucosal condition of lichen planus; when an epithelial dysplasia has multiple histologic features in common with lichen planus, it is termed lichenoid dysplasia.”2 Treatment for these types of lesions is palliative unless they become widespread, persistent, or uncomfortable, in which case the use of topical steroids is common and effective.
Since the lesion in said patient was benign and excised completely, no further follow-up was recommended.
References
- Wood NK, Goas PW. Differential Diagnosis of Oral and Maxillofacial Lesions. Mosby; 1997:75-77,98-103,106-107.
- Saap JP, Eversold L, Wysocki G. Contemporary Oral and Maxillofacial Pathology. Mosby; 1997:164-165,170,250-253.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].