Treating Caries Chemically: Fact or Fiction
Educational Objectives
Upon completion of this course, the clinician will be able to do the following:
- Define the caries process
- Describe the caries balance theory
- Apply the concept of CAMBRA to prevent caries
- Identify dental therapies aligned with the goals of CAMBRA
Introduction
This paper will review the science of caries management by risk assessment (CAMBRA) and present minimally invasive treatment strategies to prevent and treat early caries by chemical reversal. It is an important topic because dental caries is an epidemic around the world. In the United States, caries is the number one reason for a dental visit. Managing caries begins by assessing risks, by evaluating the state of pathogenic factors that encourage caries as well as protective factors that work against it, and by assessing the degree of tooth involvement. Once dental professionals have assessed the risks, they can generate a treatment plan that can include an array of chemical treatments in addition to traditional drill-and-fill treatment.
The Caries Process
Dental caries is a transmissible bacterial infection.1, 2 Infants are not born with the pathogenic organisms but acquire them from other members of the family unit. Transmission from caregiver to child is called “vertical transmission”. Studies have shown that caregivers can inoculate even predentate infants.3 “Horizontal transmission” from sibling to sibling or from spouse to spouse has also been proven.2
The main etiologic agents for dental caries are mutans streptococci (MS) and Lactobacillus (LB).4 These organisms not only tolerate an acidic environment (aciduric), but they also produce small-chain organic acids (acidogenic) by fermenting dietary carbohydrates-including but not limited to sucrose. These acids are small enough to diffuse subsurface into the enamel and dentin in fluid-filled spaces between the mineral crystals. Once subsurface, the acid will dissolve minerals (calcium and phosphate) and cause them to diffuse out of the tooth, a process that is called demineralization. If this process is not halted, the subsurface will lose so much mineral that the surface will eventually collapse or cavitate. Cavitated lesions usually need to be surgically restored.
However, if the acidic pH can be neutralized, the concentration of calcium and phosphate will eventually reach equilibrium and the demineralization process will be halted. When the concentration of calcium and phosphate are greater outside the tooth than inside the tooth, the mineral will actually go back into the tooth-a process called remineralization. Remineralization is greatly enhanced by the application of topical fluoride. Chemical remineralization is a viable treatment option for patients if the dental professional has the opportunity to act before the surface cavitates. The treatment consists of manipulating the biologic and chemical environment of the oral cavity to favor such remineralization. Understanding how this process works is best illustrated by the “caries balance theory,” proposed originally by Featherstone.5
The Caries Balance Theory
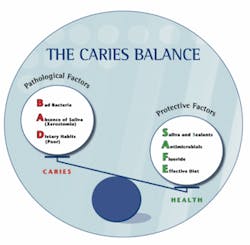
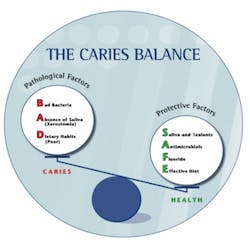
Science has identified three factors involved in decay: pathogenic bacteria (MS and LB), poor dietary habits, and xerostomia (dry mouth).5 Current protective factors include saliva, sealants, antimicrobial agents (chlorhexidine, iodine, and xylitol), fluoride, and an effective diet.5
Figure 1 depicts a balance - or scale - with pathologic factors on one side and protective factors on the other side.5 This balance dynamically changes throughout the day, even in healthy individuals. According to the caries balance theory, caries does not result from a single factor; rather, it is the outcome of the complex interaction of pathologic and protective factors. These risk factors must be assessed on a regular basis because the “weight” of each factor can change over time. For example, someone perfectly healthy today can develop xerostomia from taking certain medications and have severe decay months later. Recent research also suggests that genetics play a role in host resistance or susceptibility to dental caries.
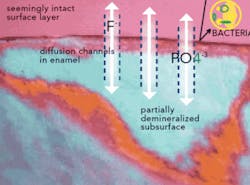
Acid: Making Channels for Caries
Sources of acid in the mouth other than from cariogenic bacteria can include dietary, stomach, and environmental acids. The subsurface dissolution of mineral that occurs during the caries process is caused by bacterially generated acids in the general range of pH 3.8 to 4.8 (Figure 2). Other acids behave differently and often cause a surface dissolution rather than a subsurface dissolution. The most dramatic example of the devastating damage to teeth caused by strong stomach acid (pH 1) is associated with gastroesophageal reflux disease (GERD) and bulimia. These extremely harsh acids attack the tooth surface directly. As with all cases of acid-to-direct-tooth-surface contact, conditions like these must be detected and managed early. Otherwise, depending on the frequency and severity of the condition, excessive amounts of mineral will be lost from the tooth surface and the rate of remineralization will not keep pace with the rate of mineral dissolution, thereby causing a net loss of mineral and increasing the chances that the tooth will require surgical restoration.
Acids from dietary sources can also cause surface dissolution. Sucking on lemons is often brought up as an example. However, it should be noted that sports drinks and carbonated beverages may have a pH as low as 3. An overly acidic oral cavity in infants and young children may also be caused by parents giving bottles of fruit juice at bedtime, which may cause early childhood caries (ECC) and baby-bottle decay (Figure 3).
Environmental acids may also be present. Industrial work places are a source of acids. Even an improperly pH-adjusted swimming pool can cause significant surface damage to the teeth over time.
Xerostomic Patients
Xerostomia (dry mouth) is a serious pathological factor because many components of saliva support dental health:
- Antibacterial agents
- Calcium
- Phosphate
- Fluoride (for remineralization)
- Lipids (for pellicle formation)
- Buffering agents (for the neutralization of acid attacks)
- Enzymes (for digestion)
- Mucins (for lubrication)
Nothing is as good as Mother Nature and there are no products that we can buy that will replace all the benefits of healthy saliva. However, it may be possible to mimic missing salivary components. Some chemical treatments include baking soda, antimicrobials such as xylitol, mineral enhancement, and topical fluoride.
Caries Management by Risk Assessment (CAMBRA)
Traditional drill-and-fill treatment will not eliminate infection. Thus, the profession is looking toward new approaches to treat the infectious component of caries. Current research does not identify a single protocol that will eliminate caries, but there have been several position papers and consensus statements to guide the dental team in using CAMBRA and subsequent chemical treatments.6
CAMBRA involves two phases. The first consists of assessing each patient’s unique caries risk (caries risk assessment). Based on the assessment of caries risk balance, the team can recommend evidence-based, tooth-preserving treatment interventions that employ minimally invasive dentistry.6,7 If the patient accepts the recommendations, the second phase will be treatment intervention. A concensus statement and CAMBRA forms can be downloaded at www.cdafoundation.org/journal.
Salivary Diagnostics
The two integral elements of the caries risk assessment (CRA) are a salivary flow rate test, to diagnose or rule out xerostomia, and a bacterial culture for mutans streptoccoci (MS) and Lactobacillus species (LB) to assess cariogenic bacterial infection. At present, there are only two commercially available bacterial culture tests for MS and LB available in the United States: CRT Bacteria from Vivadent in Amherst, New York and Dentocult from Orion Diagnostica in Espoo, Finland.
Assessing xerostomia begins with the patient interview, although simply asking patients if they have a dry mouth may not be productive. One reason is that there are degrees of xerostomia and many patients get used to the condition. It may be wise to ask a question to differentiate normal saliva flow from possible xerostomia, such as “Can you eat a large saltine cracker without sipping water?” During the medical history review, the dental professional can look for evidence of xerostomia-associated conditions, such as Sjögren’s syndrome, or ask about medications and medical treatments that can cause salivary reduction, such as antidepressants or radiation to the head and neck. During the dental history or hard tissue exam, evidence of root caries may point to dry mouth. The absence of pooling saliva in the floor of the mouth or absence of salivary flow from the Stensen’s ducts may indicate severe xerostomia but may not indicate the degree of the condition. Dental professionals should evaluate the consistency of the saliva as well. Saliva is about 99 percent water and should resemble water; thus, “frothy,” “ropey,” or “stringy” saliva are signs of moderate dry mouth.
The function of the minor salivary glands is another way to evaluate xerostomia. When the lower lip is everted and dried with gauze, it should take about 30 seconds for “spotting,” “beading,” or “sweating” to appear just under the mucosa.
Commercial tests can provide objective evaluation of the saliva. CRT Bacteria and Dentocult use stimulated saliva to inoculate the culture tubes, making it easy to test the stimulated flow rate. The patient chews on a piece of paraffin to stimulate salivation, and the saliva collects in a measuring cup over a given amount of time, such as five minutes. The amount is divided by the number of minutes to get a flow rate per minute. Flow rates below 0.7 ml/min are xerostomic. Recently, new tests have been introduced that assess pH and buffering capacity as well as flow rate. Saliva-check Buffer by GC America in Alsip, IL reports the degree of hydration, resting viscosity, resting pH, and buffering capacity. These are the kit measurements:
- Assessment of the degree of hydration by unstimulated saliva of the minor salivary glands of the lower lip
- Assessment of the resting viscosity based on the consistency of the saliva (e.g., watery, frothy, stringy)
- Testing of the resting pH of unstimulated saliva, using a pH test strip provided in the kit
- Testing of the stimulated flow rate, using that saliva to test the buffering capacity with a buffer strip provided in the kit
Normal buffering capacity can be misleading in a xerostomic patient and does not by itself indicate normal saliva function. The buffer test may indicate normal buffering capacity, but inadequate saliva production may still exist. Thus, a flow rate test is always recommended if xerostomia is suspected.
Interpretation of Salivary Diagnostics
Dehydration
Saliva tests require thoughtful interpretation if they are to be useful in determining the patient’s problems. The treatment for these problems will depend on the cause or causes.
For example, if the viscosity, consistency, and pH test are abnormal, but the stimulated salivary flow test and buffering capacity are normal, then the test indicates that the glandular function is not impaired-but the patient may be dehydrated because of inadequate fluid intake, caffeine, alcohol, strenuous physical activities, or outdoor work. In this example the supply or raw materials (water and electrolytes) needed to make the saliva are the problem, rather than a dysfunction of the glands themselves.
Compromised Gland Function
By contrast, there could be an actual problem with the salivary glands themselves due to gland pathology, radiation to the head and neck, HIV, or Sjögren’s syndrome. In these cases, the stimulated flow rate and buffering capacity would likely be abnormal.
Neural Transmission
Interference with neural transmission to salivary glands may also retard salivation. There are many potential causes of such interference, such as side effects of some medications (antidepressants, decongestants, sedatives), recreational drug use, stress, depression, or menopausal hormone imbalance. In these cases, the gland function is normal and the state of hydration can also be normal, but the signals from the brain to the salivary glands are impaired.
Caries Prevention and Minimally Invasive Treatment: Chemical Interventions
Patient compliance is essential to the chemical treatment of caries because it involves multiple treatments over time. Patients must be actively involved in their treatment since they have the daily responsibility to follow through with recommended interventions.
Antimicrobials
The chemotherapeutic agents that have been shown to reduce the pathogenic bacterial load include chlorhexidine, iodine, and xylitol.8, 9, 10 It is possible that a patient may require one or all of these chemical treatments on a regular basis before realizing a significant reduction in bacteria. More research is needed to study the combined effects of treatment interventions.
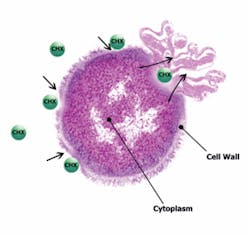
Chlorhexidine
Chlorhexidine, due to its highly cationic (positive) charge, has been shown to reduce the number of MS (Figure 4).8 It does not seem to be effective against LB.
Patients are prescribed 0.12% chlorhexidine gluconate oral rinse with instructions to rinse 0.5 oz for one minute twice a day for seven days. An alcohol-free 0.12% chlorhexidine has recently been introduced (GUM, Butler), which enables patients to obtain the benefits of chlorhexidine gluconate oral rinse without the drying effects of alcohol. Salivary bacterial culture should be performed at baseline and again after the seven days of treatment. This antimicrobial therapy is repeated with the goal of successively reducing the number of remaining pathogens.
Once the MS bacteria are eliminated, chlorhexidine rinsing is discontinued. Chlorhexidine treatment is usually followed by daily topical Fluoride, such as mouthrinse (0.05% NaF), a fluoride containing dentifrice, and xylitol gum or xylitol mints three times per day. Concurrent use of positively charged chlorhexidine and negatively charged fluoride or iodine therapy is not recommended, as they will bind and be less effective. Chlorhexidine gluconate and fluoride should be used at least 30 minutes apart. They should also not be mixed together in the same bottle.
Iodine
Iodine is a potent antimicrobial that kills on contact.9 It is a topical office procedure, not recommended for patient home use. Patients should be screened for any iodine allergies prior to use.
Studies performed in the hospital setting treating children with early childhood caries (ECC) have demonstrated that a onetime exposure of 10% Provodone iodine (1% free iodine) swabbed in the mouth significantly decreased the number of both MS and LS in children for up to three months.9 More research is required to determine if iodine is as effective for adults as it is for children.
Xylitol
Xylitol is a naturally occurring 5-carbon sugar alcohol that is totally nonfermentable by cariogenic bacteria. In addition to being a noncariogenic sugar, it appears to have unique anticaries effects. Some studies have indicated that xylitol is superior to chlorhexidine and fluoride varnish in interrupting the vertical transmission of cariogenic bacteria from caregivers to infants.11
A recent study showed that chewing xylitol gum resulted in a significant decrease in bacterial levels.10 It is unclear whether xylitol is actually lethal to bacteria or if they are cleared from the mouth by saliva because they cannot attach to the teeth, as postulated by one theory.12
The amounts of xylitol used in these studies were five to nine grams of xylitol per day, delivered to patients as xylitol-containing gum, which they chewed three to five times a day, depending on the amount of xylitol per piece of gum.The minimum dosage required for anticaries efficacy is not yet known.
Xylitol’s ability to interrupt the transmission of caries-causing bacteria makes it a candidate for use by family units in which there are pregnant mothers. The taste is almost identical to that of table sugar and should be extremely popular with patients, especially children. Xylitol can be purchased in granular form to replace table sugar. It is heat stable and can be used in cooking. Although generally safe, excessive amounts of xylitol can lead to diarrhea or gastrointestinal upset, especially upon initial use.
Topical Fluoride
No other chemotherapeutic agent in the history of modern dentistry has contributed as much to reducing caries in populations as topical fluoride. However, fluoride alone in many patients is not usually enough to tip the caries balance toward health. Careful attention to all the pathological and protective factors is advised for all patients.
Topical fluoride works by three mechanisms: inhibiting demineralization, enhancing remineralization (including fluorapatite formation), and inhibiting plaque bacteria.5 Topical Fluoride product use should be individually evaluated, taking into consideration compliance issues and daily habits of each patient. In other words, choose the fluoride product that the patient will most likely use as recommended. If compliance is a problem, the clinician can choose a fluoride varnish that is applied professionally every six months. In many cases, patients easily accept using daily home Fluoride products, such as an over-the-counter (OTC) 0.05% NaF rinse. For patients at severe risk, a higher concentration of fluoride is available at 5,000 ppm as a 1.1% sodium fluoride dentifrice that is used daily (Prevident 5000 plus, Colgate Oral Pharmaceuticals; Fluoridex Daily Defence, Discus Dental). For some patients, it may be advisable to use both an in-office fluoride and a home-use fluoride.
The daily Fluoride rinse application for remineralization is discontinued only if the patient receives a one-week chlorhexidine treatment, so as not to confuse the patient with two different rinse therapies. Additionally, young children under the age of six should not use fluoride rinses, to avoid the risk of excess Fluoride ingestion.
Calcium and Phosphate Products
Recently, products that deliver additional calcium and phosphate to the oral environment have been introduced. They include MI Paste (GC America, Alsip, IL), SootheRx (OMNII Oral Pharmaceuticals, West Palm Beach, FL), Mentadent Replenishing White, Arm and Hammer Enamel Care (Church & Dwight, Princeton, NJ), and Trident White (Cadbury Adams, Parsippany, NJ). Each of these products has different marketing claims, and careful review is recommended.
The off-label use of MI Paste for remineralization is based on several promising studies conducted to study the active molecule, casein-phosphopeptide amorphous calcium phosphate (CPP-ACP), that showed enhancement of remineralization and anticaries properties in animal studies.13, 14, 15
One study with a double-blind, randomized, crossover design investigated the acid resistance of enamel lesions that were remineralized in situ (via an intraoral appliance) by chewing a sugar-free gum containing CPP-ACP (Recaldent).14 The intervention group chewed sugar-free gum containing 18.8 mg of CPP-ACP. The control group received sugar-free gum without CPP-ACP. The level of remineralization was determined using microradiography. The results showed that the gum containing CPP-ACP produced approximately twice the level of remineralization as the control sugar-free gum. The proposed mechanism is that the CPP stabilizes calcium phosphate in solution and increases the level of calcium phosphate to help maintain a state of supersaturation. It is speculated that the anticariogenicity for the CPP-ACP occurs through localizing ACP in dental plaque, inhibiting demineralization and enhancing remineralization.16 Unlike fluoride, CPP-ACP has potential as an additive to food because it can be ingested without the risk of fluorosis. CPP-ACP is a milk derivative and should not be given to patients who have allergies to milk.
More research is needed to provide a definitive evaluation of the possible benefits of additional calcium and phosphate. Healthy saliva contains enough calcium and phosphate for remineralization, but some early studies found enhanced remineralization effects for these products.13, 14 In patients in whom there may not be enough saliva to provide adequate amounts of calcium and phosphate, such additives may prove helpful.
Baking Soda Products
Healthy saliva contains all the buffers needed to neutralize an acid attack after a meal or snack. However, where there is insufficient saliva or buffers, baking soda may help a xerostomic patient neutralize acids immediately after the ingestion of foods. Baking soda gum is available (Dental Care Gum; Church & Dwight, Princeton, NJ) or patients can simply mix two teaspoons of baking soda in eight oz of water and use the solution as a mouthrinse after eating. The patient should spit out all the liquid to minimize the ingestion of excessive sodium. Patients can also use baking soda toothpaste; however, many patients do not always brush after each snack and it may confuse patients who are also on a high-fluoride-containing toothpaste. Additional studies are needed to ascertain if more buffering in the presence of healthy saliva will help prevent caries.
Glass Ionomer: as a Chemical Caries Treatment?
Historically, glass ionomer (GI) has been viewed as a restorative material, luting cement, liner, or base, due to its retention capacity and aesthetic value. The unique chemistry of GI has led some to consider its clinical use as a means to protect teeth from caries-causing bacteria. GI can be used to seal the tooth surface to provide marginal seal and surface protection, as well as for fluoride release from harmful bacteria.
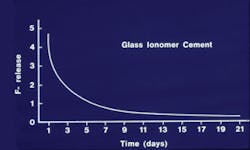
The exchange of ions between glass ionomer and the tooth has been established as the mechanism of its chemical bond to tooth mineral.17, 18, 19 The ions involved are calcium (or strontium, in some products) and fluoride from the GI material, and calcium and phosphate from the tooth. These ions migrate from the tooth and glass ionomer respectively, forming an intermediate layer that enables the glass ionomer to bond to the dentin. This “chemically fused” zone has been shown to be acid-resistant as well, implying that there is a remineralized surface internally at this interface.20, 21, 22 Figure 6 shows the fluoride release from glass ionomer cement over a period of three weeks.
Conclusion
Treating caries chemically is part of a new paradigm shift in caries management, where treating the infection is paramount. While the scientific bases for these new strategies are sound, they may take some time to be completely assimilated into routine dental care.
References
- 1. Caufield PW, Cutter GR, Dasanayake AP. Initial acquisition of mutans streptococci by infants: evidence for a discrete window of infectivity. J Dent Res. 1993;72(1):37-45.
- Berkowitz RJ. Acquisition and transmission of mutans streptococci. J Calif Dent Assoc. 2003;31(2):135-8.
- Wan AK, Seow WK, Walsh LJ, Bird P, Tudehope DL, Purdie DM. Association of Streptococcus mutans infection and oral developmental nodules in pre-dentate infants. J Dent Res. 2001;80(10):1945-8.
- Loesche WJ. Role of Streptococcus mutans in human dental decay. FEMS Microbiol Rev. 1986;50:353-80.
- Featherstone JD. The science and practice of caries prevention. J Am Dent Assoc. 2000;131(7):887-99.
- Featherstone JDB, et al. Caries management by risk assessment: consensus statement, April 2002. J Calif Dent Assoc. 2003;31(3):257-69.
- Young DA. New caries detection technologies and modern caries management: merging the strategies. Gen Dent. 2002;50(4):320-31.
- Anderson MH. A review of the efficacy of chlorhexidine on dental caries and the caries infection. J Calif Dent Assoc. 2003;31(3):211-4.
- DenBesten P, Berkowitz R. Early childhood caries: an overview with reference to our experience in California. J Calif Dent Assoc. 2003;31(2):139-43.
- Makinen KK, Isotupa KP, Makinen PL, Soderling E, Song KB, Nam SH, et al. Six-month polyol chewing-gum programme in kindergarten-age children: a feasibility study focusing on mutans streptococci and dental plaque. Int Dent J.2005;55(2):81-8.
- Isokangas P, Soderling E, Pienihakkinen K, Alanen P. Occurrence of dental decay in children after maternal consumption of xylitol chewing gum; a follow-up from 0 to 5 years of age. J Dent Res. 2000;79(11):1885-9.
- Anderson M. Chlorhexidine and xylitol gum in caries prevention. Spec Care Dentist 2003;23(5):173-6.
- Reynolds EC, Cai F, Shen P, Walker GD. Retention in plaque and remineralization of enamel lesions by various forms of calcium in a mouthrinse or sugar-free chewing gum. J Dent Res. 2003;82(3):206-11.
- Iijima Y, Cai F, Shen P, Walker G, Reynolds C, Reynolds EC. Acid resistance of enamel subsurface lesions remineralized by a sugar-free chewing gum containing casein phosphopeptide-amorphous calcium phosphate. Caries Res. 2004;38(6):551-6.
- Reynolds EC, Cain CJ, Webber FL, Black CL, Riley PF, Johnson IH, et al. Anticariogenicity of calcium phosphate complexes of tryptic casein phosphopeptides in the rat. J Dent Res. 1995;74(6):1272-9.
- Reynolds EC. Anticariogenic complexes of amorphous calcium phosphate stabilized by casein phosphopeptides: a review. Spec Care Dentist 1998;18(1):8-16.
- Yoshida Y, Van Meerbeek B, Nakayama Y, Snauwaert J, Hellemans L, Lambrechts P, et al. Evidence of chemical bonding at biomaterial-hard tissue interfaces. J Dent Res. 2000;79(2):709-14.
- Sennou HE, Lebugle AA, Gregoire GL. X-ray photoelectron spectroscopy study of the dentin-glass ionomer cement interface. Dent Mater. 1999;15(4):229-37.
- Ngo H, Mount GJ, Peters MC. A study of glass-ionomer cement and its interface with enamel and dentin using a low-temperature, high-resolution scanning electron microscopic technique. Quintessence Int. 1997;28(1):63-9.
- Milicich G. A resin impression SEM technique for examining the glass-ionomer cement chemical fusion zone. J Microsc. 2005;217(Pt 1):44-8.
- Mount G, Hume W. Preservation and Restoration of Tooth Structure. 2nd ed. Queensland, Australia: Knowledge Books and Software; 2005.
- Mount G. An Atlas of Glass-Ionomer Cements. 3rd ed. London, UK: Martin Dunitz; 2002.
Author Profile
Douglas A. Young, DDS, MS, MBA
Dr. Young is an active and ardent educator in the field of minimally invasive dentistry, dental materials, and cariology. He serves on several boards and has presented at congresses around the world, including the World Clinical Laser Institute, the Academy of Laser Dentistry, the World Congress of Minimally Invasive Dentistry, as well as at several universities.
Dr. Young has also been published in several peer-reviewed dental journals and textbooks.
In addition to speaking and publishing, Dr. Young also conducts extensive research on minimally invasive dentistry, lasers, and cariology. He has performed clinical trials using lasers and has studied caries inhibition by laser irradiation and optical caries detection technologies.
Dr. Young is an associate professor in the Department of Restorative Dentistry at the University of the Pacific School of Dentistry and is also an associate clinical professor, adjunct, at the University of California, San Francisco.
Dr. Young has a BA in bacteriology from the University of California, Berkeley; a DDS from the University of California, San Francisco; an MBA from the University of the Pacific, Stockton; and an MS in oral biology from the University of California, San Francisco. Dr. Young completed a general practice residency at the VA Hospital, San Francisco, in 1982. He decided to pursue full-time teaching after 15 years of successful private practice in California. He is currently active in teaching clinical dentistry to the students at UOP and in research at UCSF.
If you have any questions or comments for the author of this CE course, please send an e-mail to [email protected]. Please reference the course title and author’s name.
Disclaimer
This course has been made possible through an unrestricted educational grant by GC America. The author of this course has no commercial ties with the sponsors or the providers of the unrestricted educational grant for this course.
Reader Feedback
We encourage your comments on this or any ADTS course. For your convenience, an online feedback form is available at www.ineedce.com.