Case report: Replacing a failing composite using G-Premio Bond and G-aenial Sculpt
Gregori M. Kurtzman, DDS, MAGD, details a case in which he replaced a failing composite restoration on a maxillary left lateral incisor, and he explains what products he chose to use for the case and why.
Between placing new restorations and replacing failing restorations, direct resin composite restorations are among the most frequently performed treatments in general dental practice. With recent advances in bonding agents (adhesives) and composites, direct restorations are easier and more predictable. Better esthetics are more easily achievable, and less time is needed for placement. A new self-etch adhesive and a nanocomposite, formulated to pair with each other, will be discussed with regard to a case involving the replacement of a defective anterior composite restoration.
Case report
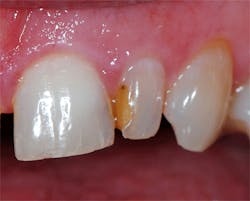
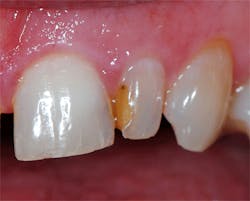
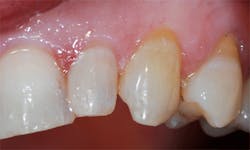
A 62-year-old female patient presented with the complaint of discoloration of a maxillary left lateral incisor. She reported slight, periodic sensitivity to cold on the tooth. Examination disclosed that an old composite restoration was "washing out" (figure 1). The treatment recommended consisted of replacing the defective composite with a new composite.
Figure 1: A defective composite was noted during a hygiene recall appointment, and the patient was advised it needed to be replaced.
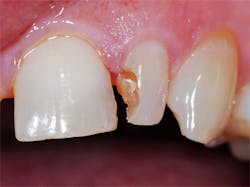
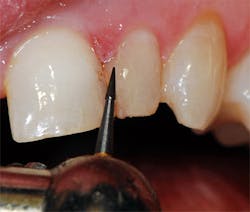
A local anesthetic (4% Septocaine with 1:100,000 epi, Septodont) was administered. The defective composite was removed with a 330 carbide bur (SS White) in a high-speed handpiece with water. Recurrent decay was noted at the gingival margin and was removed to reveal sound, intact dentin. An old cavity liner had been placed under the defective composite, and a small portion of this was left intact over the center of the preparation. The cavity liner was intact and not displaceable with an explorer (figure 2). To minimize postoperative sensitivity, a selective-etch technique was used. A 37% etching gel was applied to the enamel areas of the tooth for 20 seconds, then rinsed and dried. Cotton roll isolation was placed.
Figure 2: The old composite was removed with a carbide bur, and the enamel margins were roughened with a diamond bur in a high-speed handpiece.
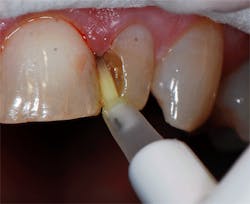
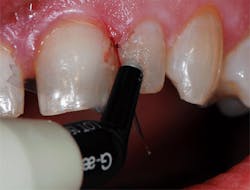
G-Premio Bond (GC America Inc.), a new universal eighth-generation bonding agent, was applied with a microbrush to all enamel and dentin surfaces and left undisturbed for 10 seconds. (figure 3). This was followed by application of a light air stream from the air/water syringe for 5 seconds to aid the evaporation of any remaining solvent in the adhesive, and then the bonding agent was light cured for 20 seconds. To ensure a thorough coating, a second coating of the adhesive was applied to the dentin areas of the prep and light cured.
A glossy surface on the dentin indicates that adhesive is fully coating the surface to be bonded. If any areas do not appear glossy, additional applications of G-Premio Bond can be applied. G-Premio Bond is compatible with total-etch, self-etch, and selective-etch techniques, providing excellent versatility for whichever technique the situation requires or the practitioner prefers.
Figure 3: G-Premio Bond was applied to the dentin and enamel margins and light cured for 20 seconds.
An Epitex clear matrix strip (GC America Inc.) was placed interproximally on the mesial, and the preparation was filled with G-ænial Sculpt (GC America Inc.), a compactable, universal composite, in shade A3 to build out a contact with the adjacent central incisor (figure 4). The composite was placed from the unitip and adapted with an instrument to cover the dentin and contact the Epitex strip.
Figure 4: An Epitex clear matrix strip was placed interproximally, and G-ænial Sculpt in shade A3 was placed into the preparation incrementally, shaped, and light cured for 20 seconds.
Because a significant portion of the tooth was missing on the mesial after removal of the defective composite, the restoration needed to be built up in increments. First, the contact was established and light cured with an LED curing light (The Light 405, GC America Inc.). Next, composite was added to the lingual to build the desired anatomy and light cured. Finally, the anatomy was constructed on the facial to the full contour, completing the restoration. The author recommends covering the entire facial surface with at least a thin layer of composite to place the margin between the resin and tooth structure in a nonvisible area. Should any staining occur in the future, it will help to hide any possible future color changes at the margin.
Author's note: G-ænial Sculpt has a high radiopacity (>300% Al), making identification of recurrent decay on recall radiographs easy. It also provides a strong, wear-resistant finished restoration with beautiful esthetics. This composite has good body, allowing sculpting of anatomy without slumping prior to light curing, yet it also has very good surface adaptation when placed against tooth structure. G-ænial Sculpt has uniform nanofiller dispersion technology, which provides high wear resistance and long-term gloss retention. Available in 17 shades, with opaque and translucent options, it can meet all esthetic needs that may present clinically. As illustrated in this case, the "chameleon" effect provided using a single-shade material can allow a natural blend matching adjacent unrestored teeth.
After full contour was achieved, the Epitex clear strip was removed. Tightness of the contact was verified with floss to ensure that the new restoration was making intimate contact with the adjacent tooth. Epitex finishing strips (fine and extra-fine) were used interproximally to achieve a smooth well-contoured surface. The anatomy was refined with safe-ended, 12-bladed finishing carbide burs (Ultimate F&P Kit, GC America Inc.) in a high-speed handpiece with water (figure 5). Occlusion was checked with articulating film (Accufilm II, Parkell Inc.) and adjusted with the Ultimate F&P Kit.
Figure 5: Finishing carbides were used for the final contouring of the restoration. Then, the restoration was polished with a polishing cup, and Epitex strips in medium and extra-fine grit were used interproximally.
Following anatomy refinement, final polishing was achieved using one-step, diamond-impregnatedabrasives from the Ultimate F&P Kit in a slow-speed handpiece to achieve a high gloss. These one-step polishers are available in point, cup, and wheel (knife-edge) shapes to accommodate polishing different tooth surfaces. The author recommends using an electric slow-speed handpiece (if one is available) with water because it helps to remove debris on the surface from the abrasive point, and it seems to yield a better gloss than an air-driven slow-speed handpiece. The final result is a natural-looking direct restoration that blends well with the adjacent tooth and has a high-gloss finish (figure 6).
Figure 6: The final restoration following finishing and polishing. Gingiva that has been irritated by the interproximal finishing strips will heal uneventfully.
Conclusion
Direct restorations remain a fundamental part of the general practice. With improvements in the adhesives available, we are able to achieve a consistent, predictable bond to both enamel and dentin. With the new nanocomposites that offer improved handling and easier polishing, we are able to provide better direct restorations in less time, improving the quality of care we are rendering.
Editor's Note: This article first appeared in Pearls for Your Practice: The Product Navigator.Click here to subscribe. Click here to submit a products article for consideration.