The highest caries risk I've ever seen: A case for 3M Ketac Universal glass ionomer restorative
Joshua Austin, DDS, FAGD, recounts the case of a teenage patient with high caries risk and high esthetic demands and explains why he thinks a glass ionomer restorative material such as 3M's Ketac Universal would have slowed the cycle of rerestoration for her, had one been available at the time he treated her.
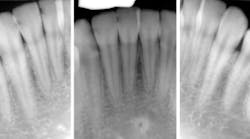
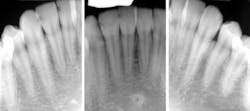
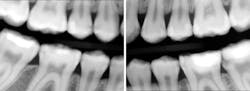
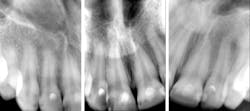
Sydney was always one of those patients I never loved seeing on the schedule. It’s not that she wasn't nice. She was very sweet and outgoing. She was one of those drama kids, the ones who are in all of the school plays and musicals. She was 17 and determined to work in the arts after school. The reason Sydney always gave me anxiety was her off-the-charts caries risk, the likes of which I rarely see. Between her astronomical caries risk and high esthetic demand (because of the acting), Sydney was—and probably still is—a challenging patient.
Sydney came in like clockwork every six months for recall. And at every recall appointment, she left with a treatment plan for restorative dentistry. I would start with the upper-right quadrant and work my way through over several weeks after each recall visit. After a couple of years of this, the cycle of rerestoration came full circle, and it was time for me to begin rerestoring teeth that I had worked on before. It was the same story for each restoration: recurrent decay interproximally at the gingival margin and a high plaque index, especially around the resins. At first, I took this poorly. I thought I must have sloppily placed those restorations before. I restored them again—this time bigger—with a rubber dam and moved on.
Always pleasant, Sydney would insist that she was brushing three to four times a day, flossing morning and night with string floss, and using interproximal brushes after lunch. Despite all of this, Sydney had a hard time controlling plaque, especially around the existing resin restorations. We worked with Sydney on technique. We worked with Sydney on products, and she began using a 5000-ppm sodium fluoride dentifrice, xylitol gum, and rinses. Sydney got a Sonicare. Sydney kept getting decay.
When Sydney started getting recurrent decay in the same areas around restorations that I had placed with a rubber dam, I began to understand that Sydney was different. I had already known she was different, but I had underestimated just how different she really was. She had the highest caries risk I have ever seen in my career. Three years ago, she moved to Washington, DC, for school. Her parents moved to the East Coast as well, so Sydney has become someone else’s problem.
I often think about Sydney and wonder what condition she must be in at this point. Deep down, I know what Sydney’s future holds. It’s a future of titanium and zirconia. My hope, however, is that dentistry can delay that as much as possible. If I knew then what I know now, I would have treated Sydney differently.
While her off-the-charts caries risk was the source of these problems, I don’t think resin composite did her any favors. Plaque loves composite and adheres to it much more tenaciously than it does enamel or amalgam. (1) Because of her esthetic demands, however, amalgam would have been a no-go.
Although it wasn't available at the time I treated Sydney, 3M’s Ketac Universal would have been a tremendous choice in her case. Ketac Universal would have given me a tooth-colored option that would not have attracted plaque, and ultimately recurrent decay, like resin composite did. The fluoride release and recharge would have been a handy weapon to have in the battle against Sydney’s caries.
I was taught in dental school that glass ionomers were not to be used on the occlusal surfaces of permanent teeth. For the majority of my career, I took that as dogma and never thought differently. Recent research on products in the same class as Ketac Universal has shown their tremendous success in Class I and II situations, with fracture rates similar to those of resin composites at recall visits up to six years after placement. (2) The high success rates of these new glass ionomers at six-year recall mean it's time to start reevaluating material choices when it comes to patients with high caries risk.
For a teenage patient like Sydney, would it have been better to use a glass ionomer material such as Ketac Universal, knowing that the restorations would at some point need to be replaced? In my mind, yes! My opinion is that the cycle of rerestoration for Sydney would have been slowed tremendously if I had used a product that had the excellent properties of traditional glass ionomers but with beefed-up wear and fracture resistance. It is not time to trash your resin composite. But it is my opinion—and I think the data backs this up—that the new generations of glass ionomer, such as Ketac Universal, deserve a spot on the shelf of every restorative dentist.
References
1. Cazzaniga G, Ottobelli M, Ionescu A, Garcia-Godoy F, Brambilla E. Surface properties of resin-based composite materials and biofilm formation: A review of the current literature. Am J Dent. 2015;28(6):311-320.
2. Gurgan S, Kutuk ZB, Ergin E, Oztas SS, Cakir FY. Clinical performance of a glass ionomer restorative system: A 6-year evaluation [published online December 20, 2016]. Clin Oral Investig. doi: 10.1007/s00784-016-2028-4.
Editor's note: Do you have a question for Dr. Austin? Is there a product you'd like to see him review? Or would you like to submit your own Pearl? Send an e-mail to [email protected]. You might just see it in the e-newsletter, Pearls for Your Practice: The Product Navigator! If you're not a Product Navigator subscriber, click here to sign up.
More enhanced Pearls
Joshua Austin, DDS, FAGD, demos the Brasseler EndoSync (VIDEO)
Front Office Rocks staff training videos (VIDEO)
Joshua Austin, DDS, FAGD, demos the Anutra Medical Dental Anesthetic Buffering System (VIDEO)
For the most current dental headlines, click here.
About the Author

Joshua Austin, DDS, MAGD
Joshua Austin, DDS, MAGD, writes the Pearls for Your Practice column in Dental Economics. After graduating from the University of Texas Health Science Center Dental School, Dr. Austin associated for several years. In October 2009, he opened a solo general practice in a suburban area of San Antonio, Texas. Dr. Austin is involved in all levels of organized dentistry and can be reached at [email protected].