Take this patient and let’s see how your treatment plan compares to mine
In my mind, one of the most challenging things in clinical dentistry is to pick up where another dentist left off. It’s not that the work is difficult; rather, it’s having the patient explain what needs to be done in his or her own terms (which admittedly can be confusing), what the anticipated outcome/goals are, and to be compared to the “other dentist” with regard to demeanor, work ethic, protocol, and standard of care. I cringe when I hear, “Well, my other dentist did/does this ...”
In some instances, it’s fairly black and white. In others, clues to the puzzle have to be gathered and fit together in order to marry what you see, what the patient says, and what you can plan for. Since we all have different viewpoints, it stands to reason that you and I may observe the same thing, but our recommendations for treatment may be altogether different.
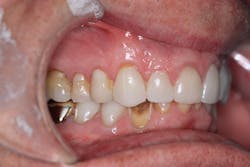
Take, for example, this 73-year-old male whose chief complaint was for his new dentist (me) to “keep doing what my other dentist was doing and fix the teeth that needed fixing.” The patient’s health history was benign, but dentally, he had the front six teeth crowned due to an accident he sustained while riding his bike. Following that, he was under the comprehensive care of a prosthodontist to restore his teeth, bite, and eliminate any issues that came about from grinding and wear.
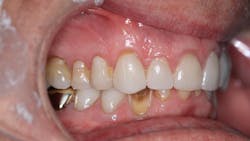
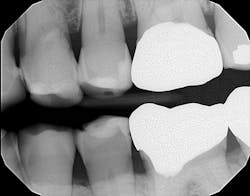
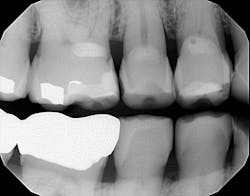
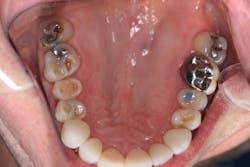
Radiographically, the first thing I noticed were the tabletopped occlusal surfaces (figures 1 and 2). Clinically, the same was evident, along with generalized wear facets on the posterior teeth (figures 3 and 4). The bite was deep (figures 5 and 6), and the lower anterior teeth had been worn down to half their original size. There were new ceramic crowns on nos. 21, 28, and 29. I also noted that there was an occlusal stop/resin on no. 13, but there was no significant effect on his occlusion as it was even on the right and left sides.
The patient was forthright and spoke in an educated manner that dictated reciprocal respect. His reason for coming to me was because he could no longer afford the specialist. Since he had insurance and I was a provider, the overall scenario was kinder on his budget. After just 15 minutes, I knew this would be a case that would both challenge and humble me.
With this information—which is all I had to go off of initially—what would you do next? Given the differences in our perception and how our practice philosophies vary, I’ll easily submit that the spectrum of recommendations will not be as black and white as you think. Why? For these very reasons:
• Occlusion is obviously an issue.
• The patient’s existing crowns do nothing to change/raise the bite, despite their recent fabrication.
• The patient wants (and clearly needs) a change in the status quo to commence with addressing the state of his existing dentition. However, what he can actually do remains to be seen.
• The factors that come into play include time, finances, and willingness on the part of the patient to move forward.
• Some of you would recommend full-mouth reconstruction to address the bite; others will consider ortho. Additionally, there are some of us who would justify maintaining things as they are but with preventive measures in place.
• Let’s not forget the mantra, “If it’s not broken, don’t fix it.” Could the patient be convinced that his teeth are fine and that a night guard is all he needs, aside from a crown on no. 27?
Share your ideas with me, and let’s see how this plays out. I will post a follow-up of what actually transpires as the case is just getting started.
Forums such as this are a melting pot of ideas to help us with the everyday and not-so-everyday clinical challenges. Do you have a case to share? Contact me and let’s chat.
Editor's note: This article originally appeared in Breakthrough Clinical, a clinical specialties newsletter from Dental Economics and DentistryIQ. Read more articles at this link.
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].