Inflammation and infection: What's the difference?
Infection can cause inflammation, where inflammation is a result of an infection. An infection is the invasion of the agent that comes from outside of the body to injure tissues. While inflammation is an inward reaction from the body, its purpose is an immediate response following an injury to repair and regenerate the living tissue.1 In dentistry, any calculus or tartar can act as an infectious agent, resulting in painful bleeding gums (the inflammatory reaction).
Inflammation
Inflammation is the normal tissue reaction following an injury from a traumatic agent or growth of organisms, basically an infection. It’s an interior reaction from the body’s response through the process of white blood cells. Immediately after trauma a triggered, the body’s response from causes the site of injury to become reddened, swollen, hot, and painful. The purpose is to localize and eliminate whatever caused the injury and to remove damaged tissue components so the body can begin to heal.
Inflammation can result from a variety of factors, such as environmental chemicals, injuries, scrapes, insect stings, or splinters, as well as radiation and pathogens including bacteria, fungi, or viruses.1
Inflammation is beneficial as the body’s defense protocol, but it if lasts too long in healthy tissue it can become damaging. The inflammation process begins immediately with the initial trauma. The arterioles in the surrounding tissues widen, allowing increased blood flow to the area causing the redness. This reaction increases permeability of the arterioles causing the white blood cells, prostaglandins (chemical mediators) and blood proteins and other fluid to build up in the injured location.
When this accumulation of fluid swelling happens, it compresses the nerves in the area—causing pain. Prostaglandins produced by the cells may cause irritation of the nerves and cause even more pain. At the site of injury, components transferred by the blood carry out the functions to protect the tissue by the white blood cells to eat the foreign bacteria, which begins the clotting process if bleeding is involved. This chemical process and increased blood supply cause the area to feel heated.2
Inflammatory conditions end with the suffix “itis”: periodontitis (bone and tissue), gingivitis (tissue), pulpitis (pulp), mucositis (mucous membranes), tonsilitis (tonsils), and stomatitis (mouth).
Acute and chronic inflammation
Acute inflammation comes quickly and resolves in less than two weeks; it’s the body’s routine way of responding to harmful substances, repairing damage, and carrying away dead cells. Reactions are the redness, swelling, heat, and pain.
Chronic inflammation is slower and generally less severe but can last from months to years. It extends from the acute stage when the body can no longer remove the harmful substance or heal an injury, which can put the body in a state of inflammation for long periods of time. Reactions to this prolonged state are body pain, digestion problems, depression, anxiety, mood disorders, constant fatigue, insomnia, weight gain, and more frequent infections.3
Treatment for chronic inflammation includes:
- NSAIDS: Inhibit the cells from producing prostaglandins, a group of hormones that will create the reactions that cause pain
- Corticosteroids: Inhibit prostaglandins formation by the cells and inhibits the function of white blood cells.
- Antihistamines: Histamine is produced by the white blood cells and causes local inflammation; these medications block the white blood cells from producing and secreting histamines.
- Hot and cold therapy: Cold constricts the blood vessels, inhibiting inflammation by numbing the pain and cooling the area. Heat reduces inflammation and the build-up of fluid in tissues.2
Infection
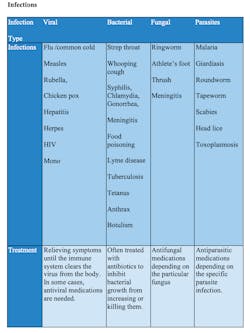
An infection is different in that it occurs via the invasion of an organism (virus, bacteria, fungi, or parasites) that enters the body and causes issues. It’s an exterior entry and growth of the organism.4
Acute infections develop suddenly and last a few days or weeks and are generally caused by a virus, infection injury, accidents, or improper use of drugs or medications. An acute infection such as a cold, flu, bronchitis, pneumonia, broken bones, asthma attack, burns, respiratory infection, or strep throat, often requires urgent short-term care.5
Chronic infections, often caused by unhealthy behaviors like poor nutrition, lack of exercise, alcohol abuse, or excessive smoking, develop slowly and worsen over months to years. Chronic infection is a condition that progresses over time with possible warning signs. Such conditions are high blood pressure, diabetes, heart disease, obesity, high cholesterol, osteoporosis, arthritis, or Alzheimer’s disease. These conditions are often then maintained and not cured.
Symptoms of infection include fever or chills, body aches and pains, coughing or sneezing, digestive upset, and feeling tired or fatigued.6
Dental infections and inflammation conditions
- Thrush: Oral fungal called candidiasis; white thick, cottage cheese-like lesions on the tongue, cheeks, palate, tonsils, back of throat, and gums.
- Hand/foot/mouth disease: Coxsackie virus infection that causes a rash of blisters specifically on the hands, feet, and around the mouth.
- Herpangina: Coxsackie virus infection that causes painful, red ulcers inside the mouth.
- Tonsilitis: Viral or bacterial infections causing swelling of the tonsils.
- Pulpitis: Bacterial-related infection causing inflammation of the inner tooth.
- Mucositis: Inflammation of the mucous lining of the inner mouth, commonly from cancer treatment.
- Stomatitis: An inflamed and sore mouth including the cheeks, tongue, and gums.
- Gingivitis: Bacterial infection causing inflammation of the gums.
- Tooth abscess: A collection of pus caused by bacteria at the tip of the root.
- Periodontal abscess: A collection of pus caused by bacteria along the side the tooth within the tissue.
- Periodontitis: A serious gum infection that damages not only the soft tissue but also the bone supporting the teeth. Since these two structures are what holds the teeth within the jaw, it’s pretty crucial to prevent or resolve the infection. Treatment to remove periodontal infection usually starts with a deep cleaning under the gumline to remove the source of the infection (known as calculus and plaque). Depending on the severity, a dental professional may recommend more periodontal surgeries.
While both an infection and inflammation are crucial to the body responding to injury, they should be resolved so they don’t cause serious issues. When it pertains to the mouth, good home care and regular dental checkups are important. Daily brushing with an electric toothbrush, flossing, and even using a water flosser help prevent oral infections and inflammation. Regular dental checkups and cleanings are beneficial for diagnosing if there’s a concern and for prevention of future oral disease.
Editor's note: This article has been updated as of November 2024.
References
1. Inflammation. National Institute of Environmental Health Sciences. March 16, 2021. https://www.niehs.nih.gov/health/topics/conditions/inflammation/index.cfm
2. Dr Chris. Inflammation — Causes, Symptoms, Process, Treatment. Health Hype. https://www.healthhype.com/inflammation-causes-symptoms-process-treatment.html
3. Acute and chronic inflammation. CBHS Health. March 20, 2020. https://www.cbhs.com.au/mind-and-body/blog/acute-and-chronic-inflammation
4. Chronic vs. acute medical conditions: What’s the Difference? August 11, 2016. https://www.ncoa.org/article/chronic-versus-acute-disease
5. Dr Samanka. Difference between inflammation and infection. September 30, 2013. https://www.differencebetween.com/difference-between-inflammation-and-infection/
6. Seladi-Schulman J.Infections: What you need to know. Healthline. https://www.healthline.com/health/infections#4
About the Author

Lara James, RDH
Lara James, RDH, is a licensed dental hygienist with more than 15-plus years of clinical hygiene experience in corporate, dental management, and private practices. She has created DentalAisle.com, a dental blog to educate consumers on dental products and dental issues. Lara also has written an online continuing education course on dentalcare.com. For more information, email her at [email protected].
Updated October 26, 2022