Restoring the endodontically treated tooth with CEREC 3D
WRITTEN BY
Suzette Stines, DDS
Restoring the endodontically treated tooth can provide challenges when planning all-ceramic restorations. As dentistry shifts from metal-based restorations to newer nonmetal restorative materials, we face evaluating the physical properties of a suite of materials. In the restorative scenario of post choices, core choices, and resin cements, all of the elements must be compatible with each other, provide adequate resistance and retention, withstand fracture, and meet esthetic demands.
As a CEREC dentist, I evaluate each step in restoring an endodontically treated tooth because material selection is as important to success as preparation form.
For this reason, if a post is to be placed, I choose a fiber post for fracture resistance and long-term success. Conventional fiber and ceramic posts provide an advantage over conventional posts in that they result in fewer nonrestorable root fractures, superior retrievability, and demonstrate a similar value of force to failure.1
The hygroscopic expansion of resin-modified, glass ionomer cements or compomer materials leads to failure of all-ceramic crowns when used as a core and when used as a bonding cement. Sindel, Frandenberger, Kramer, and Petschelt reported in their 1999 study that after 12 months, all of the porcelain crowns over resin-modified, glass ionomer cement or compomers as well as those luted with RMGIC or compomers developed cracks. None of the restorations over resin buildups or luted with resin cements exhibited crack formation.2 In comparing glass ionomer, resin-modified glass ionomer, titanium-reinforced composite, composite resin with fluoride, and amalgam for fracture toughness, titanium-reinforced composite resin and composite resin with fluoride and amalgam material are the ones that show fracture toughness most likely to withstand the stresses generated during mastication.3 There is no demonstrated difference in the compressive strength of crowns placed over dentin, amalgam, or composite.4 With research supporting the strength and fracture resistance of resin-core materials, I choose a composite resin core for esthetic compatibility with my CEREC all-ceramic crowns. Choosing a core shade that most closely mimics the dentin shade of the tooth will also optimize the esthetics of the cemented restoration.
The requirements for resistance and retention in all-ceramic restorations differ from those of porcelain-fused-to-metal or all-metal restorations in that the resin cement, rather than the preparation form, provides the majority of resistance and retention. This allows me to feel comfortable in restoring teeth that are severely broken down, lacking in occlusal gingival dimension, or both. The resin bond is sufficiently strong to withstand occlusal forces, even in cases with reduced stump form.5
Otto, Bindl, Richter, and Mormann investigated the five-year survival of CAD/CAM restorations with reduced stump form. This study is interesting in that crowns were bonded to preparations with normal stump height, reduced stump height, and no stump (only pulp chamber retention). After five years, they determined that endo preparations were completely adequate for molar restorations while inadequate for premolars (87 percent retention for molars and 68 percent for premolars). Retention on reduced-stump preparations was rated at 92 percent for both molars and premolars. For classic preparations with normal stump height, survival was rated at 97 percent for molars and 95 percent for premolars. It is always advisable to build up some core form on premolars even though it may be a reduced stump. Molars do not require a buildup.6 I have cemented molars with no stump form and only pulp chamber retention that have survived five years in my practice. I have not found this formation to be retentive enough for premolars.
CEREC restorations are an excellent choice when choosing an all-ceramic restoration. They have been reported to have a 90 to 95 percent survival rate of 10 years or better.7,8 These restorations are reported to have excellent marginal integrity and little postoperative sensitivity.9,10
CASE STUDY
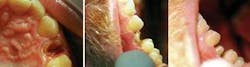
A 53-year-old male presented with a severely broken-down maxillary first premolar. The crown height was completely fractured away at the level of the gingival (Figure 1). Radiographic evaluation revealed satisfactory endodontic treatment without periodontal involvement. Adequate tooth structure remained above the bone for crown preparation. A treatment plan was developed that included gingival surgery to expose the clinical crown and increase crown length, placement of a fiber post, core buildup with resin, and an all-ceramic crown.
Soft-tissue surgery was performed with an Odyssey Diode Laser, which I find easy to use because of its excellent control and great postoperative results. I use this diode laser with many of my CEREC restorations to expose the restoration margin prior to optical imaging. In this instance, I was able to gain 4 to 5 millimeters of crown height while simultaneously removing the hyperplastic tissue in the interproximal area to reveal the hidden interproximal tooth structure (Figure 2).
I followed this surgery with caries removal, ensuring that only sound tooth structure remained. I placed a fiber post (FiberKor, Jeneric Pentron) in the palatal canal. I bonded the post into place with Multilink (Ivoclar) no-etch resin cement. I built up the core to an ideal stump form with 4 Seasons composite material (Ivoclar). I prepared the tooth for a CEREC all-ceramic crown. I was careful to retain as much tooth structure as possible while maintaining the requirements of material thickness in the preparation form (Figure 3).
Then I took a polyvinylsiloxane bite registration (Patterson Bite Registration Material). I powdered the bite with optical imaging agent (Vita) and took an optical impression with the bite registration in place over the preparation. I removed the bite registration, powdered the preparation, and took an optical impression of the preparation. The CEREC 3D system automatically correlates these two optical impressions by accurately suspending the antagonist in a data cloud over the preparation’s optical impression.
CEREC 3D then generated a virtual model. The bite registration generates a virtual model of the antagonist occlusion that can then be used to virtually articulate the restoration to develop accurately the occlusion of the restoration. I trimmed the bite to include only the useful occlusal contacts (Figures 4, 5).
The CEREC 3D system’s new R2005 software includes significant software improvements. The new crown-design software automatically positions the crown in the arch, locates the cusps in the ideal position, and virtually grinds to develop an accurate occlusion. The positions of the crown and the cusps are determined by the software analysis of the data provided by the bite registration of the antagonist occlusion (Figure 6). The practitioner can define the proximal contact location. The software will then automatically locate and adjust the density of the proximal contacts.
All of these improvements make crown design so much easier and faster than in previous software versions. I chose my tooth from one of the many new tooth libraries available in the new R2005 software. The new libraries allow practitioners to choose from youthful, adult, mature, Asian, oval, square, or tapering libraries to find the most compatible tooth shapes. The software then generates a restoration proposal that automatically aligns the arch in the most optimal position. I evaluated the bite and with a click virtually ground the restoration into occlusion (Figure 7). I then used the automatic proximal contact feature to adjust the proximal contacts to my preferred contact density. In just a few minutes, the crown was ready for milling.
The R2005 CEREC 3D software can mill restorations with a 30 percent reduction in milling time. This restoration milled in about seven minutes. I chose a block of Vita Mark II feldspathic porcelain (Vident) for this restoration. I tried in the restoration and verified the occlusal contacts (Figure 8). No occlusal adjustment was required and the contacts were as represented in the virtual restoration. I stained and glazed the restoration using Vita stains and glazes (Vident) to achieve esthetic compatibility with the surrounding dentition. After staining and glazing, I cleaned and etched the crown with hydrofluoric Vita ceramic etching agent (Vident). Next, I sinalated the crown with Kerr Silane for one minute to create an organic-inorganic bond.
I isolated the area with an Isolite to ensure a dry field, cementing the restoration with Multilink (Ivoclar). I tacked the cement with a light until the cement achieved a gel-like state. I thoroughly cleaned the area of all excess cement. Finally, I cured the cement with a high-speed curing light for 10 seconds from each aspect.
By carefully choosing the materials employed in each step, I ended up with a clinically superior result (Figure 9). The patient was satisfied and pleased that all of this was accomplished in one appointment. I performed the soft-tissue surgery, placed the post, built up the core form, and prepared and cemented the crown in one appointment. The CEREC 3D system with the new R2005 software is a great way to provide your endodontic patients with beautiful all-ceramic restorations quickly and easily.
References
1 Cormier CJ, Burns DR, Moon P: In vitro comparison of the fracture resistance and failure mode of fiber, ceramic, and conventional post systems at various stages of restoration. J Prosthodont. 2001 Mar;10(1):26-36.
2 Sindel J, Frankenberger R, Kramer N, Petschelt A: Crack formation of all-ceramic crowns dependent on different core build-up and luting materials. J Dent. 1999 Mar; 27 (3):175-81.
3 Bonilla ED, Mardirossian G, Caputo AA: Fracture toughness of various core build-up materials. J Prosthodont. 2000 Mar; 9(1):14-18.
4 Azer SS, Drummond JL, Campbell SD, El Moneim ZA: Influence of core build-up material on the fatigue strength of an all-ceramic crown. J Prosthet Dent 2001 Dec; 86(6):624-31.
5 Otto T: Computer-aidfed direct all-ceramic crowns: preliminary 1-year results of a prospective clinical study. Int J Periodontics Restorative Dent 2004 Oct; 24(5):446-55.
6 Bindl A, Richter B, Mormann WH: Survival of ceramic computer-aided design/manufacturing crowns bonded to preparations with reduced macroretention geometry. Int J Prosthodon 2005 May-Jun;18(3):219-24.
7 Posselt A, Derschbaum T: Longevity of 2328 chairside CEDREC inlays and onlays. In J. Computer Dent 2003;6(3):231-248.
8 Otto T, De Nisco S: Computer-aided direct ceramic restorations: a 10-year prospective clinical study of CEREC CAD/CAM inlays and onlays. Int J Prosthodont 2002 Mar-Apr; 15(2):122-8.
9 CRA News Nov 1999; 23(11).
10 Estefan D, Dussetschleger F, Agosta C, Reich, S. Scanning electron microscope evaluation of CEREC12 and CEREC 3 inlays. Gen Dent Sept/Oct 2003.
Suzette Stines, DDS
Dr. Stines is a 1981 graduate of the University of North Carolina School of Dentistry. She is a frequent lecturer to dental societies and study clubs on techniques of computerized dentistry and porcelain. She may be reached at (910) 654-4235 or via email, [email protected].