Editor's note: Originally published June 21, 2019. Formatting updated November 10, 2022.
Case history
Six years ago, a healthy 30-year-old female presented for a new-patient exam. She had no concerns or issues. The patient recently had tooth No. 3 removed and was returning for a full assessment.
The case of the unknown pathology
Oral symptoms of systemic pathology in a 17-year-old female
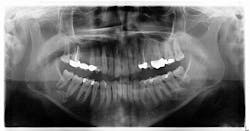
Radiographic assessment revealed a radiopaque s-/oval-shaped lesion on the right side of the mandible just inferior to the apical roots of tooth no. 31 (figure 1). The patient reported no sensitivities or tenderness in the area and was unaware of any potential pathology. Previous panoramic radiographs were not obtainable. At that time, we explained to the patient that we would reexamine the lesion with a subsequent radiograph in the next year to assess for any changes.
Six years later: Presentation and exam
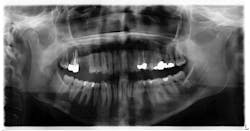
Six years later (the patient left the area and then returned), the patient presented to my office for updates with a chief complaint of caries on her wisdom teeth and a desire to have them removed. A new panoramic radiograph was taken. The lesion on the lower right side of the mandible was noted as still present with no significant changes in shape or size (figure 2).
Treatment and discussion
The patient was referred to an oral surgeon for removal of her wisdom teeth. Furthermore, it was requested that the lesion be assessed for a more definitive diagnosis, even though visibly it had not changed in shape, size, or location.
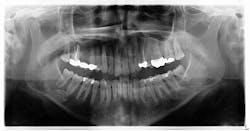
A cone beam scan was taken, and it was noted that there was no lesion within the bone of the mandible. More than likely it was a cast ghost image from a hyoid bone that sat higher than normal. As there were no complaints of neurosensory changes, bony expansion, tenderness to the area, or changes between the two radiographs, there were no treatment recommendations at this time. The area, of course, would be monitored in future radiographs for any clinical symptoms.
Differential diagnosis
With regard to a differential diagnosis, for the aforementioned reasons one could consider these:
- Sialolith
- Calcified lymph nodes
- Condensing osteitis
- Idiopathic osteosclerosis
About the Author
Stacey L. Gividen, DDS
Stacey L. Gividen, DDS, a graduate of Marquette University School of Dentistry, is in private practice in Montana. She is a guest lecturer at the University of Montana in the Anatomy and Physiology Department. Dr. Gividen has contributed to DentistryIQ, Perio-Implant Advisory, and Dental Economics. You may contact her at [email protected].