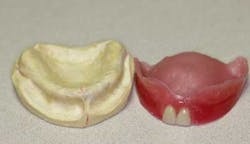
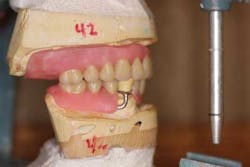
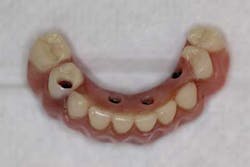
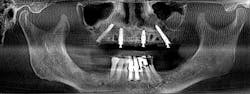
Dentures, partials, and their role in dentistry
It has been said, “A patient without eyes cannot see and a patient without legs cannot run, yet a patient without teeth expects to eat and act with dentures as they do with natural teeth.” There is truth to this statement if you have ever fabricated dentures or partial dentures.
ALSO BY DR. STACEY SIMMONS |Braces: the good, the bad, and the ugly
What would it be like if we could replace every missing tooth with an implant? The possibilities for implants and their implication in the future of dentistry are endless, and yet not all people are candidates or are able to do implants (financially, medically, etc.). We have to acknowledge these circumstances that dictate us to consider and offer alternative replacement means to these patients, mainly dentures and partial dentures.
ALSO BY DR. STACEY SIMMONS |Watch, fill, or crown? How you can involve your patients in the dental treatment planning process
Dentures and partial dentures are treatment options that are an acceptable way to replace function and missing teeth. Unfortunately, many practitioners find the creation of said prostheses frustrating and difficult. Not only can the fabrication be challenging, but, statistically, these populations of patients have the highest percentage of dental complaints. Why? Because the loss of the problematic natural teeth is often considered a way to eliminate dental woes. Instead, a removable prosthesis is actually an introduction into a new realm of challenges. Regardless of these concerns, when treatment planned and fabricated correctly, the outcome for partials and dentures can be predictable.
An established, step-by-step protocol needs to be set and maintained from the initial to the final treatment, so the patient is fully aware of what to expect.
1. Assess the patients’ needs and listen to their goals and expectations. It is not uncommon to hear patients say they don’t want to lose any more teeth. Unfortunately, many are unaware of those factors that make keeping their teeth impractical — advanced periodontal disease, caries condition, etc. Many patients are open to the idea of partials and/or dentures; others are not.
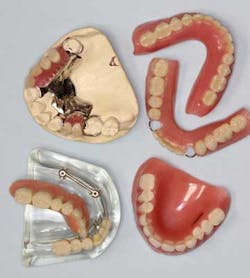
2. Discuss ALL restorative and replacement options — have models available showing implants, partials, dentures, bridges, etc. As oral health-care providers, it is our job to diagnose and then present ways to restore form and function. Educating the patient allows for a good patient/provider relationship and ultimately a better long-term outcome.
3. Have the patient sign a consent form prior to taking ANY impressions. In this form, discuss expectations with the interims and/or the definitive restorations. Review changes in function — speech, mastication, how fit changes over time due to the constant bone resorption, and the potential need for relines, etc. Discuss what you as a provider can do for patients when these issues arise.
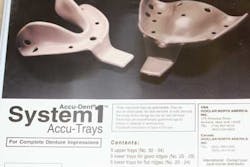
4. Take reliable impressions and bite registrations. The denture/partial is based off what you send to the lab. If the process begins with a poor impression, then you have set yourself up for countless visits with that patient in the chair for adjustments and relines. An excellent final impression material is Acugel/AcuDent by Ivoclar Vivodent. The extended borders on the trays (both for edentulous and dentate impressions) eliminate the need for border molding; furthermore, it is very accurate due to the material’s wettability. Retakes are very few.
5. For large spans or for full edentulism, make interim dentures/partials. By allowing the tissue and bone to heal properly, the stage is set for a better-fitting definitive prosthesis. It also gives patients an “extra set” should they lose or break their final denture/partial down the road.
6. Don’t skip steps! Verifying the midline, high lip line, vertical dimension, phonetics, and esthetics are essential to achieving a functional and acceptable prosthesis.
The use of adhesives and inherent hassle of dentures and partials will often give rise to the incentive to look into more permanent options. Again (assuming medical history is not an issue), review implant alternatives and how patients can improve the status quo — bridges, All-On-4, implant-supported dentures, fixed hybrid prostheses, etc.
Remember that success with partials and dentures is only partially defined by technical excellence and is not an exclusive dentist-determined prerogative — don’t allow patients to set their expectations too high! If you do, it can set the stage for failure, despite your best intentions and effort.