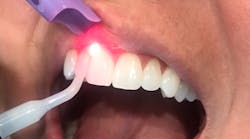
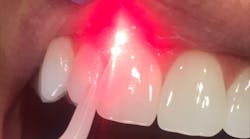
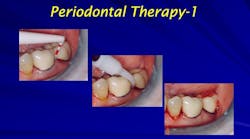
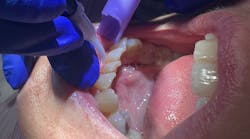
Photobiomodulation, biostimulation, low-level lasers, and red-light therapy: Uses in the dental operatory
Photobiomodulation (PBM) and other technology—e.g., low-level lasers, biostimulation, red-light therapy, soft lasers, and cold lasers—are becoming increasingly well-known in dentistry. Let’s start by looking at some of the basics of PBM.1
What is photobiomodulation?
Photobiomodulation stands for:
Photo: light from either a laser or LED
Bio: eliciting a biological response
Modulation: response to the light energy, resulting in either stimulation or inhibition
Photobiomodulation occurs when light photons act on several cell processes to stimulate the release of cellular energy in the form of ATP, which can be used to facilitate the restoration of normal cell function. PBM actions are due to stimulation of the mitochondria (at the cellular level) to increase ATP production.2
How does PBM work?
A low-level laser emits coherent and focused energy that penetrates deeply to stimulate the target tissue. A low-level laser is a therapeutic device that cannot be used to cut tissue. PBM is defined as using a laser (with output power well below surgical parameters) to elicit a biological response.
Currently, the FDA has approved the use of PBM for pain management. Light augments the metabolic rate of cells with compromised metabolism. Normal cells are not affected, but they can be used to stimulate blood flow, macrophages, and fibroblasts. PBM can reduce pain receptors and is used postsurgically for dentinal hypersensitivity and TMD.
Applications for PBM
PBM can be used to treat:
- Dentinal hypersensitivity
- Herpes simplex
- Postsurgical healing
- Paresthesia
- Mucositis
- Nerve regeneration
- Pain
- TMD
- Trigeminal neuralgia
- Bone regeneration
- Anti-inflammatory
- Accelerated tissue repair and cell growth
- Improved vascular activity
- Increased metabolic activity
- Trigger points and acupuncture points
- Reduced fibrous tissue formation
- Improved nerve function
- Immunoregulation
- Faster wound healing
Other applications of PBM in a dental office:
- Creating an analgesic in teeth so more restorations can be completed without the need for needles
- Prevention of nausea and gagging using the P6 acupuncture point (located three fingers under the wrist)
- Treatment of soft tissue lesions, cold sores, aphthous ulcers, and denture sores
- Better bone healing in implants and bone grafts
- Prevention and treatment of mucositis after chemotherapy
- Nerve regeneration
- Treatment of facial plan
- TMJ3
Overview of PBM and its effects
Output power: It is important to know what the output power for a PBM device is. Different light therapy instruments have different output power. The typical power output for a PBM device is in milliwatts (50 mW–500 mW), and there is no thermal effect possible within this range.4
Low-intensity laser therapy: low-powered devices (600 nm–1060 nm) usually for class II and III. The diode laser delivers a coherent and focused energy that penetrates deeply to stimulate target tissue. A high-powered light-emitting diode (LED) delivers a noncoherent, broad beam producing evenly distributed light energy over a large area.
Light therapy: uses light energy in the form of photons from low-level lasers or superluminous diodes to elicit cellular and biological responses in the body.
Light (red and near-infrared): can modulate biological processes, leading to beneficial clinical effects such as biostimulation, anti-inflammation, and analgesic effects.
Anti-inflammatory: causes vasodilation and reduces the lymphatic drainage system, which will drain swollen areas, and reduces swelling caused by bruising and inflammation.
Analgesic: provides an analgesic effect on nerve cells, blocks pain transmitted to these cells, and decreases nerve sensitivity. There is less edema and less pain due to decreased inflammation. Promotes high levels of pain-killing chemicals such as endorphins from the brain and adrenal glands.
Accelerated tissue repair and cell growth: photons of light from lasers penetrate deeply into tissue and accelerate cellular reproduction and growth. Laser light increases the energy available to the cell so that the cell can take on nutrients faster and get rid of waste products. The result is that damaged cells are repaired faster.
Improved vascular activity: laser light will increase the formation of new capillaries in damaged tissue, which speeds up healing, closes wounds quickly, and reduces scar tissue.
Increased metabolic activity: creates higher outputs of specific enzymes and greater oxygen loads for blood cells.
Trigger points and acupuncture points: stimulates muscle trigger points and provides musculoskeletal pain relief, reduces fibrous tissue formation, and reduces the formation of scar tissue following tissue damage from cuts, scratches, burns, or surgery.
Improved nerve function: laser light speeds the process of nerve cell reconnection and increases the amplitude of action potentials to optimize muscle healing.
Immunoregulation: laser light stimulates immunoglobulins and lymphocytes. Lasers are absorbed by chromophores that react to laser light. After exposure to the laser, the production of ATP will begin. ATP is the major carrier of cell energy in the cells.
Faster wound healing: laser light stimulates fibroblast development in damaged tissue. Fibroblasts are the building blocks of collagen, which is the protein required to replace old tissue and repair tissue injuries.
How can dental patients benefit from PBM?
PBM can improve clinical outcomes and decrease pain in patients after dental treatment.
Positive effects of PBM:
- Stimulates endorphins
- Reduces the conduction of nerve fibers (which carry pulpal pain)
- Stimulates fibroblasts, osteoblasts, and odontoblasts (which create soft tissue, bone, and dentin)
- Increases circulation and lymphatic drainage
Postsurgical benefits of PBM:
- Less pain
- Minimal swelling
- Minor bruising
- Reduced inflammation
- Reduced need for postoperative analgesics
- Accelerated healing due to the stimulation of fibroblasts
How safe is PBM?
The best part about PBM is there are no clinical side effects. Photobiomodulation merely restores ATP levels in the mitochondria to normal levels. Instead of using drugs to treat pain, light energy can be used. This is an untapped and underutilized resource in the dental industry.
Tips for using PBM
A low dose of light energy will result in cellular stimulation (stimulation of fibroblasts for improved tissue healing), which can promote healing. A high dose of light energy results in cellular inhibition (reduction of inflammatory chemicals), which can be useful for pain management. This additional cellular energy is also helpful to power many secondary side effects.5
Dosage too low: no effect
Correct dosage: desired result
Dosage too high: inhibitory effect
Acute inflammation is good: it promotes healing.
Chronic inflammation is bad: it promotes chronic wounds and impairs function
Always treat the source of the pain—not the site of the pain.6
Treatment protocol
Acute condition: Treat three to four times for one week. No further treatment for the next two weeks. Reassess the patient and the condition.
Chronic condition: Treat the patient two to three times a week in the office for three weeks. No further treatment for the next two weeks. Reassess the patient and the condition.6
The FDA’s position
Biostimulation lasers—low-level laser therapy (LLLT), cold lasers, soft lasers, or laser acupuncture devices—were cleared for marketing by the FDA through the Premarkets Notification/510(k) process as adjunctive devices for the temporary relief of pain. These clearances were based on the presentation of clinical data to support such claims. The FDA will consider similar applications for these and other claims, with the decision to require clinical data to be collected on an individual basis, taking into consideration both the device and the claim.7
Why lasers over opioids?
In 2017, 72,300 Americans died from drug overdose. Of those, 47,600 were from opioid overdose.
The CDC estimates that the total economic burden of prescription opioid misuse is $78.5 billion per year. Most of these individuals became addicted after obtaining narcotic pain prescriptions from their health-care providers.
PBM can reduce the need for narcotic prescriptions.6 When dentists hear the word “laser,” most think of hard- or soft-tissue lasers that are used to cut enamel or soft tissue. Many clinicians don’t know that lasers, low-level lasers, and LEDs can be invaluable tools in the operatory.
Editor’s note: This article first appeared in Clinical Insights newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles and subscribe.
Resources
- Academy of Laser Dentistry
- THOR Lasers
- GMA Laser Education
- Talking evidence with THOR photomedicine
- My top five LLLT would healing papers by James Carroll
References
- Carroll J. What is cold laser therapy? THOR Lasers. November 1, 2010. https://blog.thorlaser.com/?s=What+is+Cold+Laser+Therapy%3F&search1.x=0&search1.y=0
- Carroll J. Institute of physics feature on future of LLLT. THOR Lasers. April 9, 2009. https://blog.thorlaser.com/institute-of-physics-feature-on-future-of-lllt/
- What is photobiomodulation therapy (PBMT)? THOR Lasers. https://www.thorlaser.com/photobiomodulation.php
- Carroll J. LLLT / Low level laser therapy and the rise and fall of modern medicine. THOR Lasers. October 5, 2011. https://blog.thorlaser.com/lllt-andthe-rise-and-fall-of-modern-medicine/
- Carroll J. LLLT – dose rate effects. THOR Lasers. 2008. https://blog.thorlaser.com/dose-rate-effects/
- Ross G, Burchman M, Darbar A. Photobiomodulation (PBM) for accelerated healing and pain management. GMA Laser Education. https://www.gmalasereducation.com/p/photobiomodulation-pbm-for-accelerated-healing-and-pain-management
- Radiation-emitting products. U.S. Food and Drug Administration. http://www.fda.gov/Radiation-EmittingProducts
Angie Wallace, RDH, has been a clinical hygienist for more than 35 years. She is a member of the Academy of Laser Dentistry (ALD), where she obtained her advanced level proficiency, her educator status, and received her ALD Recognized Course Provider and her mastership. Angie currently serves as chair for education on the ALD Board of Directors and serves on the auxiliary committee. She was the recipient of the 2014 John G. Sulewski Distinguished Service Award from the ALD and has been recognized as a worldwide speaker and as a laser consultant for dental and dental hygiene schools, laser manufacturers, and private offices. She can be reached at [email protected].
About the Author
Angie Wallace, RDH
Angie Wallace, RDH, has been a clinical hygienist for more than 35 years. She is a member of the Academy of Laser Dentistry (ALD), where she obtained her advanced level proficiency, educator status, Recognized Course Provider status, and mastership. Angie is the chair for education on the ALD Board of Directors and serves on both the Regulatory Affairs and Auxiliary committees. She has a laser education consulting company, Laser Hygiene, LLC, and has been recognized as a worldwide speaker. Contact her at [email protected].